Pressure ulcers, commonly referred to as bed sores, are a significant health concern for individuals who are bedridden, use wheelchairs, or have limited mobility. These injuries occur when prolonged pressure is applied to the skin, leading to damage in the underlying tissues. Understanding the causes, recognizing the stages of development, and implementing effective prevention and care strategies are essential for managing this condition. In this article, we will explore all these aspects in detail.
What Are Pressure Ulcers?
Pressure ulcers are localized injuries to the skin and underlying tissue, usually over bony areas of the body. They develop when sustained pressure restricts blood flow to the affected area, depriving it of oxygen and nutrients. This can result in tissue damage or even tissue death if left untreated. These injuries are most commonly found on areas such as the hips, heels, elbows, and tailbone.
Who Is at Risk?
- Individuals who are bedridden or confined to wheelchairs
- People with limited mobility due to injury or illness
- Patients with chronic conditions like diabetes or vascular disease
- Elderly individuals, especially those with frail skin
- Those who are malnourished or dehydrated
Causes of Pressure Ulcers
Several factors contribute to the development of pressure ulcers. Understanding these causes can help caregivers and healthcare professionals take preventive measures.
Prolonged Pressure
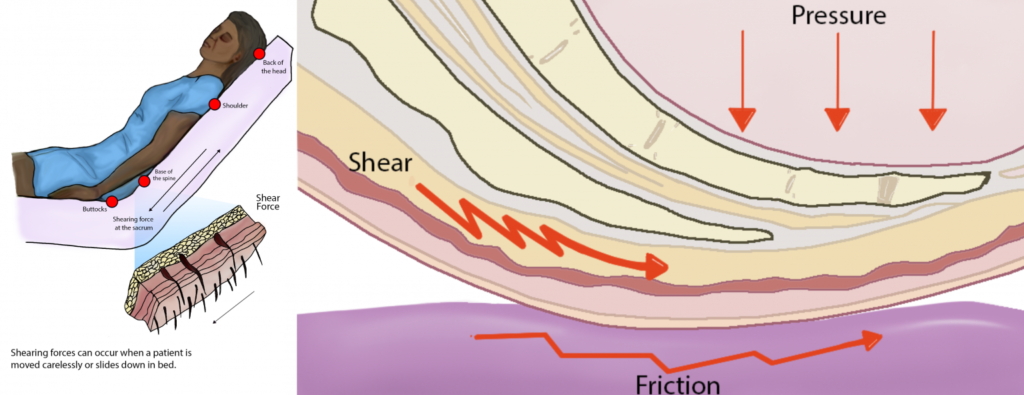
The primary cause of pressure ulcers is sustained pressure on a specific area of the body. When pressure is applied continuously, it compresses blood vessels, reducing or cutting off blood flow to the skin and underlying tissues. Without adequate blood supply, the tissues begin to break down and eventually die.
Friction and Shear
Friction occurs when the skin rubs against clothing or bedding, causing abrasions that make the skin more vulnerable to injury. Shear happens when the skin remains stationary while the underlying bone moves, stretching and tearing blood vessels. Both friction and shear can exacerbate the effects of pressure, increasing the risk of developing ulcers.
Moisture
Excessive moisture from sweat, urine, or feces can soften the skin, making it more susceptible to damage. Prolonged exposure to moisture weakens the skin’s protective barrier, increasing the likelihood of ulcer formation.
Poor Nutrition and Hydration
A lack of proper nutrition and hydration can impair the body’s ability to repair damaged tissues. Proteins, vitamins, and minerals are essential for maintaining healthy skin and promoting healing. Dehydration further compromises skin integrity, making it more prone to injury.
Stages of Pressure Ulcers
Pressure ulcers progress through distinct stages, each characterized by varying degrees of tissue damage. Recognizing these stages is crucial for determining the appropriate treatment plan.
Stage One: Non-Blanchable Redness
In the first stage, the skin appears red and does not turn white when pressed. The affected area may feel warm, firm, or painful. At this stage, the damage is limited to the outermost layer of the skin, and prompt intervention can prevent further progression.
Stage Two: Partial-Thickness Skin Loss
At this stage, the skin begins to break open, forming a shallow ulcer or blister. The damage extends into the deeper layers of the skin but does not penetrate through to the underlying tissue. Proper wound care is essential to prevent infection and promote healing.
Stage Three: Full-Thickness Skin Loss
In stage three, the ulcer extends through all layers of the skin and into the subcutaneous tissue, exposing fat. The wound may appear crater-like, and there may be signs of infection, such as pus or foul odor. Treatment at this stage requires careful cleaning and possibly surgical intervention.
Stage Four: Extensive Tissue Damage
Stage four ulcers involve severe damage to muscles, tendons, and even bones. These wounds are deep and often accompanied by significant infection and necrosis. Medical intervention is critical, and treatment may include debridement, antibiotics, and surgery.
Unstageable Ulcers
Sometimes, the extent of tissue damage cannot be determined due to the presence of dead tissue or eschar covering the wound. In such cases, the ulcer is classified as unstageable until the debris is removed, allowing for a proper assessment.
Prevention of Pressure Ulcers
Preventing pressure ulcers is far more effective than treating them. Implementing proactive measures can significantly reduce the risk of developing these painful injuries.
Frequent Repositioning
Changing positions regularly is one of the most effective ways to relieve pressure on vulnerable areas. For bedridden individuals, repositioning every two hours is recommended. Wheelchair users should shift their weight every 15 to 30 minutes to redistribute pressure.
Use of Supportive Devices
Specialized cushions, mattresses, and overlays can help reduce pressure on high-risk areas. Foam, gel, or air-filled devices are designed to distribute weight evenly and minimize the risk of tissue damage.
Maintaining Skin Health
Keeping the skin clean and dry is essential for preventing ulcers. Regularly inspecting the skin for signs of redness or irritation allows for early intervention. Moisturizers can be used to prevent dryness, but they should not be applied to already damaged skin.
Proper Nutrition and Hydration
A balanced diet rich in proteins, vitamins, and minerals supports skin health and aids in the healing process. Adequate hydration ensures that the skin remains supple and resilient. Nutritional supplements may be recommended for individuals with deficiencies.
Care for Pressure Ulcers
Once a pressure ulcer has developed, proper care is essential to promote healing and prevent complications. The treatment approach depends on the stage and severity of the ulcer.
Cleaning the Wound
For stage one and two ulcers, gentle cleansing with mild soap and water is sufficient. More advanced ulcers require thorough cleaning with saline solution to remove debris and prevent infection. Avoid using harsh chemicals or antiseptics, as they can damage healthy tissue.
Dressing the Wound
Applying an appropriate dressing helps protect the ulcer from further injury and promotes healing. Hydrocolloid dressings, foam dressings, and alginate dressings are commonly used depending on the wound’s characteristics. Dressings should be changed regularly to maintain cleanliness and monitor progress.
Managing Infection
Infections are a common complication of pressure ulcers, especially in later stages. Signs of infection include increased redness, swelling, warmth, pus, and fever. Antibiotics may be prescribed to treat bacterial infections, and debridement may be necessary to remove dead tissue.
Pain Management
Pressure ulcers can be extremely painful, particularly during dressing changes. Pain management strategies may include over-the-counter pain relievers, topical anesthetics, or prescription medications. Ensuring comfort is an important aspect of care.
Surgical Intervention
In severe cases, surgical treatment may be required to close the wound and restore function. Procedures such as skin grafts, flap surgery, or vacuum-assisted closure can help accelerate healing and reduce the risk of complications.
Conclusion
Pressure ulcers are a serious yet preventable condition that requires vigilance and proactive care. By understanding the causes, recognizing the stages, and implementing effective prevention and treatment strategies, individuals and caregivers can significantly reduce the impact of these injuries.