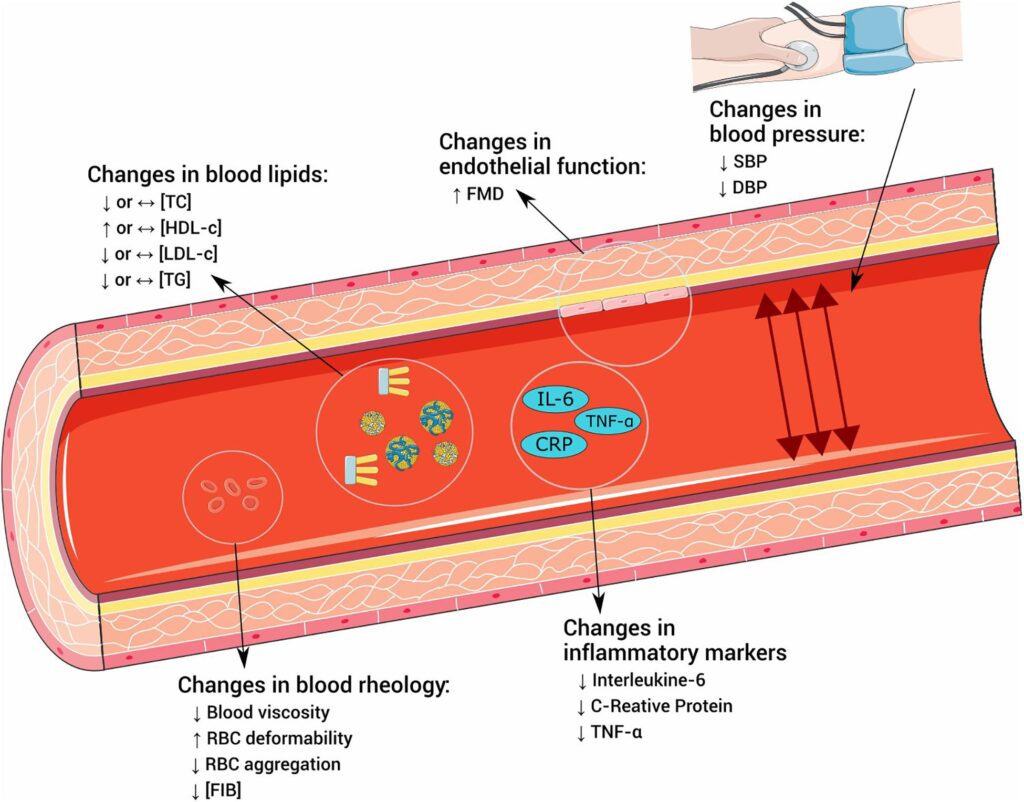
Hardening of the arteries, commonly referred to as arteriosclerosis, is a progressive condition that affects the cardiovascular system. It involves the thickening and stiffening of artery walls, which can restrict blood flow and lead to serious health complications. This condition is often abbreviated as AS, but for the purposes of this article, we will explore it in full detail without abbreviations.
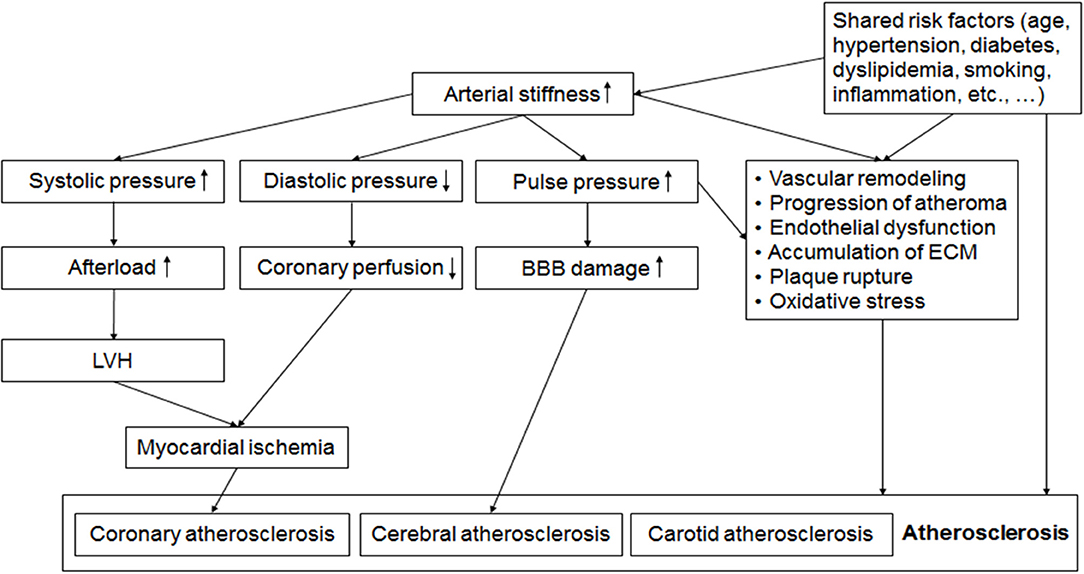
Understanding the Condition
Arteriosclerosis is a broad term that describes the hardening and loss of elasticity in the arteries. While it is often confused with atherosclerosis, the two are distinct yet related conditions. Atherosclerosis refers specifically to the buildup of plaque within the arterial walls, while arteriosclerosis encompasses a wider range of arterial changes, including calcification and fibrosis.
Types of Arteriosclerosis
- Monckeberg’s arteriosclerosis: Characterized by calcium deposits in the muscular walls of arteries, typically affecting smaller vessels.
- Atherosclerosis: The most common form, marked by the accumulation of fatty deposits, cholesterol, and other substances in the arteries.
- Arteriolosclerosis: Involves the hardening of small arteries and arterioles, often associated with high blood pressure and diabetes.
Causes of Hardening of the Arteries
The exact cause of arteriosclerosis is multifactorial, involving a combination of genetic, lifestyle, and environmental factors. Below are some of the primary contributors to the development of this condition.
Unhealthy Diet
A diet high in saturated fats, trans fats, cholesterol, and sodium can significantly increase the risk of developing hardened arteries. These dietary components contribute to the buildup of plaque within the arterial walls, narrowing the passageways for blood flow.
Lack of Physical Activity
Sedentary lifestyles are closely linked to the development of arteriosclerosis. Regular physical activity helps maintain healthy blood pressure levels, improves circulation, and reduces the risk of obesity, all of which are protective against arterial hardening.
Tobacco Use
Smoking is one of the leading causes of arteriosclerosis. The chemicals in tobacco smoke damage the lining of the arteries, promoting inflammation and the formation of plaque. Additionally, smoking reduces oxygen levels in the blood, further straining the cardiovascular system.
High Blood Pressure
Hypertension places excessive stress on the arterial walls, causing them to thicken and lose elasticity over time. This chronic pressure can accelerate the progression of arteriosclerosis and increase the likelihood of complications such as heart attacks and strokes.
Diabetes
Individuals with diabetes are at a higher risk of developing hardened arteries due to elevated blood sugar levels. High glucose levels can damage blood vessels and impair their ability to function properly, contributing to the progression of arteriosclerosis.
Genetic Factors
A family history of cardiovascular disease or arteriosclerosis can predispose individuals to the condition. Genetic mutations affecting lipid metabolism, inflammation, and blood vessel integrity may play a role in its development.
Symptoms of Hardening of the Arteries
In its early stages, arteriosclerosis often does not produce noticeable symptoms. However, as the condition progresses and blood flow becomes restricted, various signs and symptoms may emerge depending on the affected arteries.
Coronary Arteries
When arteriosclerosis affects the coronary arteries, which supply blood to the heart, it can lead to angina or chest pain. Individuals may experience discomfort, tightness, or pressure in the chest, particularly during physical exertion or emotional stress.
Carotid Arteries
The carotid arteries supply blood to the brain. When these arteries are affected, individuals may experience symptoms such as dizziness, confusion, difficulty speaking, or even transient ischemic attacks, which are temporary episodes resembling strokes.
Peripheral Arteries
Hardening of the peripheral arteries, which supply blood to the limbs, can cause pain, numbness, or weakness in the legs and arms. This condition, known as peripheral artery disease, often worsens with physical activity and improves with rest.
Renal Arteries
When arteriosclerosis impacts the renal arteries, which supply blood to the kidneys, it can lead to high blood pressure or kidney failure. Symptoms may include swelling in the legs, fatigue, and changes in urination patterns.
Diagnosis of Hardening of the Arteries
Early detection of arteriosclerosis is crucial for preventing complications. Healthcare providers use a variety of diagnostic tools to assess the condition of the arteries and identify any blockages or abnormalities.
Physical Examination
A thorough physical examination can reveal signs of arteriosclerosis, such as weak or absent pulses, abnormal heart sounds, or bruits, which are unusual whooshing noises heard over narrowed arteries.
Blood Tests
Blood tests can measure cholesterol levels, triglycerides, and other markers of cardiovascular health. Elevated levels of these substances may indicate an increased risk of arteriosclerosis.
Imaging Tests
Several imaging techniques are used to visualize the arteries and assess their condition. These include ultrasound, computed tomography scans, magnetic resonance imaging, and angiography. Each method provides valuable information about the extent and location of arterial hardening.
Treatments for Hardening of the Arteries
The treatment of arteriosclerosis focuses on slowing its progression, managing symptoms, and reducing the risk of complications. Treatment plans are tailored to the individual’s specific needs and may involve lifestyle changes, medications, and surgical interventions.
Lifestyle Modifications
Making healthy lifestyle choices is the cornerstone of managing arteriosclerosis. These changes can help improve overall cardiovascular health and prevent further damage to the arteries.
- Dietary Changes: Adopting a heart-healthy diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can lower cholesterol levels and reduce inflammation.
- Regular Exercise: Engaging in moderate-intensity physical activity for at least 150 minutes per week can improve circulation and strengthen the cardiovascular system.
- Smoking Cessation: Quitting smoking is essential for halting the progression of arteriosclerosis and improving overall health.
- Weight Management: Maintaining a healthy weight reduces strain on the heart and lowers the risk of complications.
Medications
Various medications are available to manage arteriosclerosis and its associated risk factors. These drugs work by lowering cholesterol, reducing blood pressure, preventing blood clots, and controlling diabetes.
- Statins: These medications lower cholesterol levels by inhibiting the production of cholesterol in the liver.
- Antihypertensives: Drugs such as beta-blockers, ACE inhibitors, and diuretics help control high blood pressure.
- Antiplatelet Agents: Aspirin and similar medications reduce the risk of blood clots by preventing platelets from sticking together.
- Diabetes Medications: Insulin and oral hypoglycemic agents help regulate blood sugar levels in individuals with diabetes.
Surgical Interventions
In severe cases of arteriosclerosis, surgical procedures may be necessary to restore blood flow and prevent life-threatening complications.
- Angioplasty: This minimally invasive procedure involves inserting a balloon-tipped catheter into the blocked artery to widen it and improve blood flow.
- Stent Placement: A stent, or small mesh tube, may be inserted during angioplasty to keep the artery open.
- Bypass Surgery: In this procedure, a healthy blood vessel is grafted around the blocked artery to create a new pathway for blood flow.
- Endarterectomy: This surgery involves removing plaque from the arterial walls to restore normal blood flow.
Prevention of Hardening of the Arteries
While some risk factors for arteriosclerosis, such as age and genetics, cannot be controlled, many preventive measures can significantly reduce the likelihood of developing the condition.
Healthy Eating Habits
Consuming a balanced diet low in saturated fats, trans fats, and sodium can help maintain healthy cholesterol levels and reduce inflammation. Incorporating foods rich in omega-3 fatty acids, fiber, and antioxidants can further support cardiovascular health.
Regular Health Screenings
Routine check-ups and screenings can detect early signs of arteriosclerosis and allow for timely intervention. Monitoring blood pressure, cholesterol levels, and blood sugar levels is essential for maintaining optimal health.
Stress Management
Chronic stress can contribute to the development of arteriosclerosis by raising blood pressure and promoting unhealthy behaviors such as overeating or smoking. Practicing relaxation techniques like meditation, yoga, or deep breathing can help mitigate these effects.
Avoiding Tobacco and Excessive Alcohol
Eliminating tobacco use and limiting alcohol consumption are critical steps in preventing arteriosclerosis. Both habits can damage blood vessels and increase the risk of cardiovascular complications.