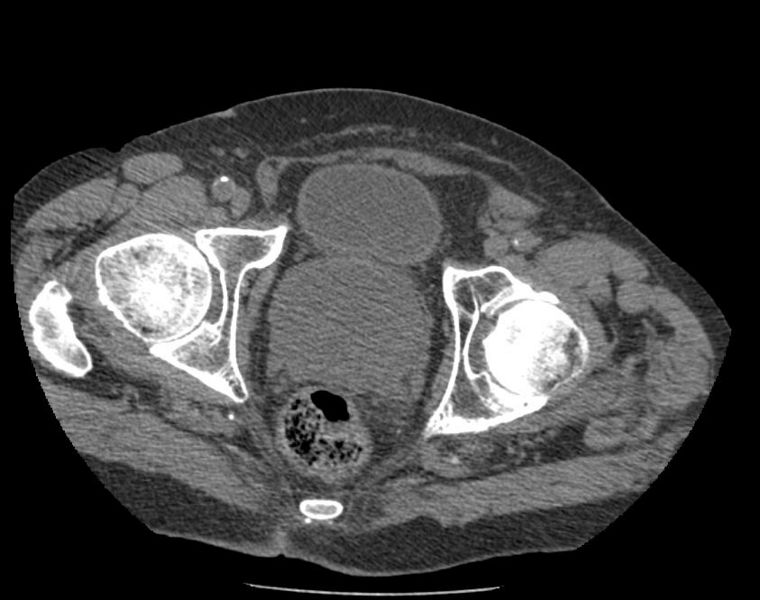
Benign Prostatic Hyperplasia, commonly referred to as BPH, is a condition that affects a significant number of men, particularly as they age. It involves the non-cancerous enlargement of the prostate gland, which can lead to various urinary symptoms and complications. Understanding this condition is essential for managing it effectively and improving quality of life. In this article, we will explore the overview, causes, symptoms, and care options associated with an enlarged prostate.
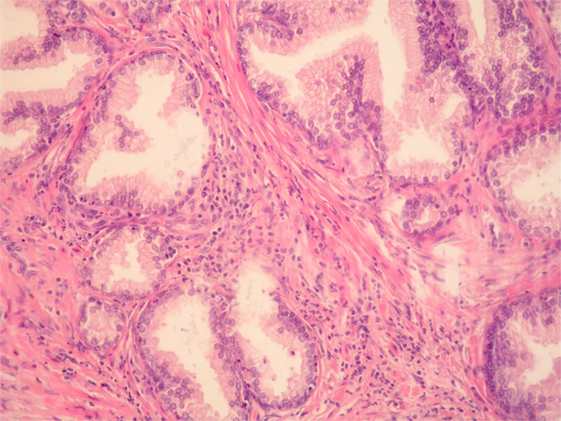
What is an Enlarged Prostate?
The prostate gland is a small, walnut-shaped organ located below the bladder in men. Its primary function is to produce fluid that nourishes and transports sperm. As men age, the prostate gland often grows larger, a process known as benign prostatic hyperplasia. This growth is not cancerous but can cause significant discomfort and urinary issues due to its proximity to the urethra, the tube through which urine passes out of the body.
How Common is Benign Prostatic Hyperplasia?
- It is estimated that more than half of men over the age of fifty experience some degree of prostate enlargement.
- The likelihood of developing this condition increases with age, affecting nearly ninety percent of men over eighty years old.
Causes of an Enlarged Prostate
While the exact cause of prostate enlargement remains unclear, several factors are believed to contribute to its development:
Hormonal Changes
As men age, hormonal changes occur within the body. One key factor is the balance between testosterone and estrogen. Testosterone levels decrease gradually, while estrogen levels remain stable or increase slightly. This imbalance may stimulate prostate cell growth. Additionally, a hormone called dihydrotestosterone plays a role in maintaining prostate health. However, elevated levels of this hormone have been linked to prostate enlargement.
Cell Growth and Aging
The natural aging process contributes to the accumulation of prostate cells. Over time, these cells multiply, leading to an increase in the size of the prostate gland. This growth is considered normal but can become problematic when it begins to interfere with urinary function.
Genetic Factors
Family history can also play a role in the development of an enlarged prostate. Men with close relatives who have experienced prostate issues are at a higher risk of developing similar problems themselves.
Lifestyle Factors
Although lifestyle choices do not directly cause prostate enlargement, certain habits can exacerbate symptoms. These include:
- Consuming excessive amounts of alcohol or caffeine
- A sedentary lifestyle with little physical activity
- Poor dietary habits, such as diets high in red meat and low in fruits and vegetables
Symptoms of an Enlarged Prostate
The symptoms of an enlarged prostate vary from person to person and depend on the severity of the condition. Some individuals may experience mild discomfort, while others face significant challenges in their daily lives. Common symptoms include:
Urinary Issues
- Frequent urination, especially during the night (nocturia)
- Difficulty starting urination
- A weak or interrupted urine stream
- A feeling of incomplete bladder emptying
- Dribbling after urination
Bladder Problems
An enlarged prostate can put pressure on the bladder, causing it to become overactive. This may result in:
- Urgency to urinate
- Involuntary leakage of urine (urinary incontinence)
Complications
If left untreated, an enlarged prostate can lead to more serious complications, including:
- Urinary tract infections due to stagnant urine in the bladder
- Kidney damage caused by prolonged obstruction of urine flow
- Bladder stones formed from mineral deposits in retained urine
Diagnosis of an Enlarged Prostate
To diagnose an enlarged prostate, healthcare providers typically perform a series of tests and evaluations. These assessments help determine the severity of the condition and rule out other potential causes of urinary symptoms.
Medical History and Physical Examination
The first step in diagnosing an enlarged prostate involves taking a detailed medical history and conducting a physical examination. During this process, the doctor may ask about urinary habits, family history, and any medications being taken. A digital rectal exam is often performed to assess the size and texture of the prostate gland.
Urinalysis
A urinalysis is conducted to check for signs of infection, blood, or other abnormalities in the urine. This test helps identify underlying conditions that could mimic the symptoms of an enlarged prostate.
Prostate-Specific Antigen Test
A blood test measuring prostate-specific antigen levels may be recommended. Elevated levels of this protein can indicate prostate issues, although they are not specific to benign prostatic hyperplasia and may also suggest prostate cancer.
Urodynamic Tests
These tests evaluate how well the bladder and urethra store and release urine. They provide valuable information about bladder function and the extent of obstruction caused by the enlarged prostate.
Treatment Options for an Enlarged Prostate
Treatment for an enlarged prostate depends on the severity of symptoms, the impact on quality of life, and the presence of complications. There are several approaches to managing this condition, ranging from lifestyle modifications to surgical interventions.
Lifestyle Changes
Making simple adjustments to daily habits can alleviate mild symptoms and improve overall urinary health:
- Limiting fluid intake before bedtime to reduce nocturia
- Avoiding caffeine and alcohol, which can irritate the bladder
- Engaging in regular physical activity to promote healthy circulation
- Practicing pelvic floor exercises to strengthen bladder control
Medications
Several types of medications are available to treat an enlarged prostate:
- Alpha-blockers relax the muscles around the prostate and bladder neck, making it easier to urinate.
- 5-alpha reductase inhibitors shrink the prostate by blocking the production of hormones responsible for prostate growth.
- Combination therapy using both alpha-blockers and 5-alpha reductase inhibitors may be prescribed for severe cases.
Minimally Invasive Procedures
For individuals who do not respond to medication or prefer non-surgical options, minimally invasive procedures may be recommended:
- Transurethral microwave thermotherapy uses heat to destroy excess prostate tissue.
- Urethral stents are inserted to keep the urethra open and improve urine flow.
Surgical Interventions
In cases where symptoms are severe or complications arise, surgery may be necessary:
- Transurethral resection of the prostate removes excess prostate tissue through the urethra.
- Laser therapy uses concentrated light energy to vaporize obstructive tissue.
- Open prostatectomy is performed for very large prostates and involves removing the central portion of the gland.
Caring for an Enlarged Prostate
Managing an enlarged prostate requires ongoing care and attention. By adopting healthy habits and working closely with healthcare providers, individuals can minimize symptoms and prevent complications.
Regular Monitoring
Men diagnosed with an enlarged prostate should schedule regular check-ups with their healthcare provider. These visits allow for the monitoring of symptoms, assessment of treatment effectiveness, and early detection of potential complications.
Healthy Diet and Hydration
Eating a balanced diet rich in fruits, vegetables, whole grains, and lean proteins supports overall prostate health. Staying hydrated is equally important, though it is advisable to spread fluid intake throughout the day rather than consuming large amounts at once.
Stress Management
Chronic stress can exacerbate urinary symptoms. Practicing relaxation techniques such as deep breathing, meditation, or yoga can help manage stress levels and improve overall well-being.
Education and Support
Learning about the condition and connecting with support groups can empower individuals to take an active role in their care. Sharing experiences with others facing similar challenges provides emotional support and practical advice.