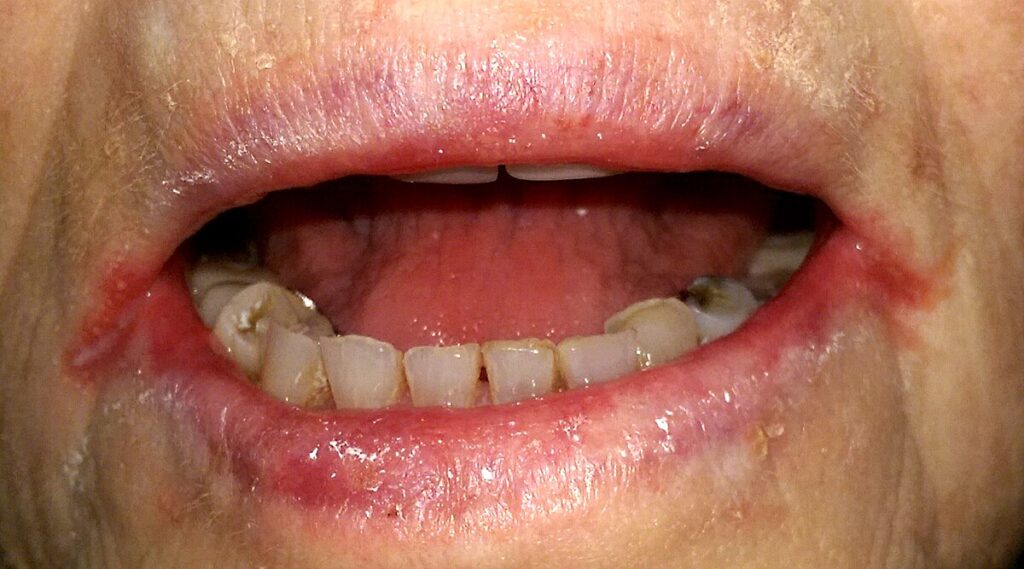
Angular Cheilitis, often abbreviated as AC, is a common condition that affects the corners of the mouth. It is characterized by redness, swelling, cracking, and sometimes bleeding at the edges of the lips. While it may seem like a minor issue, Angular Cheilitis can cause significant discomfort and affect daily activities such as eating, speaking, and smiling. This article delves into the causes, symptoms, and treatments for this condition to help you better understand and manage it.
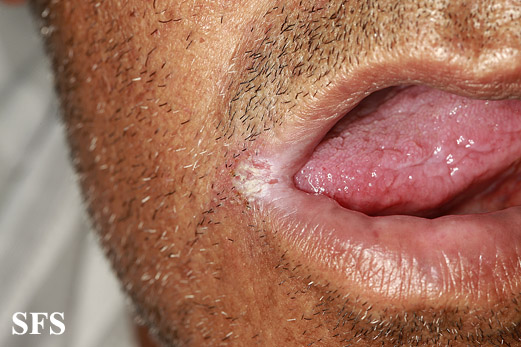
What is Angular Cheilitis?
Angular Cheilitis refers to inflammation or infection that occurs at the corners of the mouth. The affected areas often become cracked, sore, and irritated, making it painful to open the mouth wide or eat certain foods. The condition can occur in people of all ages but is more commonly seen in older adults, children, and individuals with compromised immune systems.
Common Symptoms
- Redness and swelling at the corners of the mouth
- Pain or tenderness when opening the mouth
- Cracking or splitting of the skin
- Bleeding from the cracked areas
- Dryness and flakiness around the affected regions
- In severe cases, pus or discharge may develop
Causes of Angular Cheilitis
The development of Angular Cheilitis can be attributed to various factors, ranging from nutritional deficiencies to infections. Understanding the root cause is essential for effective treatment and prevention.
Nutritional Deficiencies
One of the most common causes of Angular Cheilitis is a lack of essential nutrients in the diet. Deficiencies in vitamins such as B2 (riboflavin), B3 (niacin), B6 (pyridoxine), and B12, as well as iron and zinc, can weaken the immune system and make the skin more prone to irritation and infection.
Fungal Infections
Fungal infections, particularly those caused by Candida yeast, are another leading cause of this condition. Candida naturally resides in the mouth and digestive tract, but an overgrowth can lead to infection. People who wear dentures, have diabetes, or take antibiotics are more susceptible to fungal infections.
Bacterial Infections
Bacterial infections can also contribute to Angular Cheilitis. Staphylococcus aureus and Streptococcus bacteria are common culprits. Poor oral hygiene, frequent lip licking, or drooling can create an environment where bacteria thrive, leading to infection at the corners of the mouth.
Saliva Accumulation
Excess saliva pooling at the corners of the mouth can irritate the skin and create cracks. This is often seen in individuals who drool during sleep, have misaligned teeth, or wear ill-fitting dentures. The constant moisture weakens the skin barrier, making it more vulnerable to infection.
Environmental Factors
Cold weather, dry air, and excessive sun exposure can dry out the skin around the mouth, increasing the likelihood of cracking. Similarly, habits like licking the lips or using harsh skincare products can exacerbate the problem.
Underlying Health Conditions
Certain health conditions, such as diabetes, anemia, and autoimmune disorders, can predispose individuals to Angular Cheilitis. These conditions often compromise the immune system, making it harder for the body to fight off infections.
Symptoms of Angular Cheilitis
Recognizing the symptoms of Angular Cheilitis is crucial for early intervention. While the severity of symptoms may vary, the following signs are commonly observed:
Mild Symptoms
- Minor redness and irritation at the corners of the mouth
- Occasional dryness or flaking of the skin
- Mild discomfort when opening the mouth wide
Moderate Symptoms
- Noticeable cracking or splitting of the skin
- Swelling and tenderness in the affected areas
- Pain while eating or speaking
Severe Symptoms
- Deep cracks that may bleed or ooze
- Formation of crusts or scabs
- Persistent pain and discomfort
- Presence of pus or discharge, indicating infection
Treatment Options for Angular Cheilitis
Treating Angular Cheilitis involves addressing the underlying cause while alleviating the symptoms. Depending on the severity of the condition, treatment may include lifestyle changes, topical medications, or oral supplements.
Topical Antifungal Creams
If a fungal infection is the cause, antifungal creams containing clotrimazole or miconazole are often prescribed. These medications help eliminate the overgrowth of yeast and reduce inflammation. Applying the cream directly to the affected areas two to three times a day can provide relief within a few days.
Antibacterial Ointments
For bacterial infections, antibacterial ointments such as Neosporin or Bacitracin may be recommended. These ointments help kill bacteria and prevent further infection. It is important to clean the area gently before applying the ointment to ensure maximum effectiveness.
Nutritional Supplements
If a nutrient deficiency is contributing to the condition, taking vitamin supplements can be beneficial. For example, adding riboflavin, niacin, or zinc supplements to your diet can strengthen the immune system and promote healing. A healthcare provider can recommend the appropriate dosage based on individual needs.
Moisturizers and Barrier Creams
Using moisturizers or barrier creams can help protect the skin from further irritation. Products containing petroleum jelly or beeswax create a protective layer that prevents saliva or other irritants from aggravating the skin. Applying these creams after cleaning the area can speed up the healing process.
Improving Oral Hygiene
Maintaining good oral hygiene is essential for preventing and treating Angular Cheilitis. Brushing and flossing regularly, using an antibacterial mouthwash, and ensuring dentures fit properly can reduce the risk of infection. If drooling is an issue, sleeping with your head slightly elevated can help minimize saliva accumulation.
Avoiding Irritants
To prevent worsening the condition, it is important to avoid irritants such as spicy foods, acidic beverages, and harsh skincare products. Lip licking and biting should also be avoided, as these habits can further damage the skin.
Medical Intervention
In severe cases, medical intervention may be necessary. A healthcare provider may prescribe oral antifungal or antibiotic medications if topical treatments are not effective. Additionally, underlying health conditions such as diabetes or anemia should be addressed to prevent recurrence.
Preventing Angular Cheilitis
Prevention is always better than cure. By adopting healthy habits and making lifestyle changes, you can reduce the risk of developing Angular Cheilitis.
Maintaining a Balanced Diet
Eating a diet rich in vitamins and minerals is key to preventing nutrient deficiencies. Incorporating foods such as leafy greens, whole grains, lean proteins, and dairy products can provide the nutrients needed for healthy skin.
Staying Hydrated
Drinking plenty of water keeps the skin hydrated and reduces the likelihood of dryness and cracking. Avoiding excessive caffeine and alcohol consumption can also help maintain skin health.
Protecting the Skin
Using a lip balm with SPF protection can shield the skin from harmful UV rays. During cold weather, covering the mouth with a scarf can prevent dryness caused by harsh winds.
Regular Dental Checkups
Visiting the dentist regularly ensures that any dental issues, such as misaligned teeth or ill-fitting dentures, are addressed promptly. Proper dental care can prevent saliva buildup and reduce the risk of infection.
Managing Underlying Health Conditions
If you have a chronic health condition such as diabetes or anemia, managing it effectively can lower the risk of developing Angular Cheilitis. Regular checkups and adherence to treatment plans are essential for maintaining overall health.