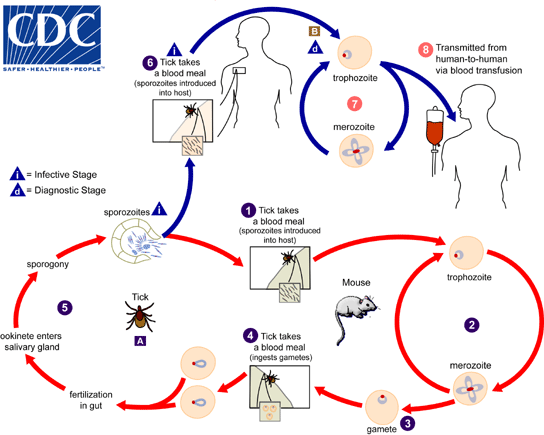
Babesiosis, often abbreviated as BAB, is a tick-borne disease caused by microscopic parasites that infect red blood cells. This condition has become an increasing concern in recent years due to its potential severity and the rising incidence of tick-related illnesses worldwide. The disease is primarily transmitted through the bite of infected ticks, but other modes of transmission also exist. Understanding the nature of this illness, its symptoms, diagnosis, treatment, and prevention is essential for safeguarding public health.
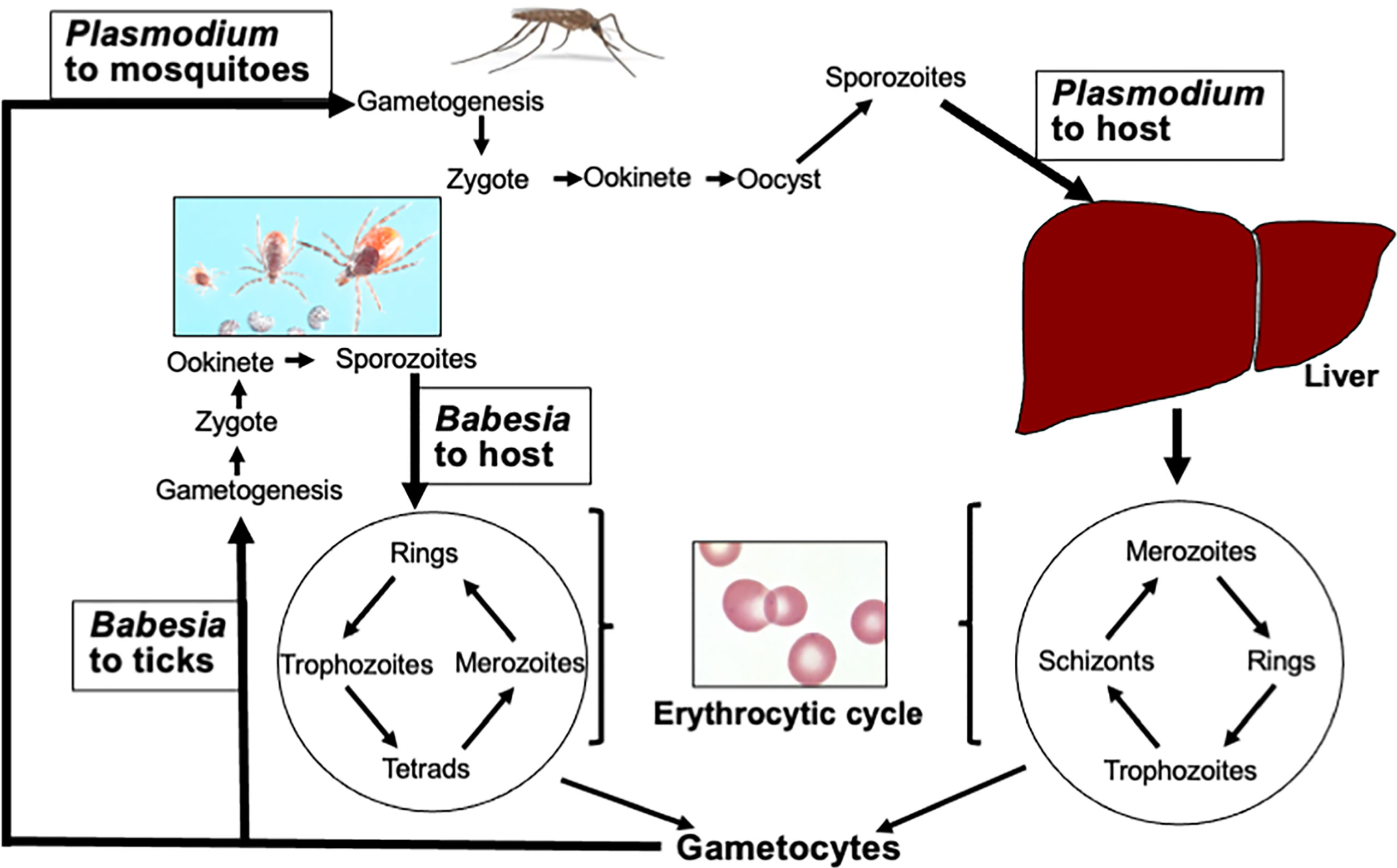
What is Babesiosis?
Babesiosis is an infectious disease caused by protozoan parasites belonging to the genus Babesia. These parasites invade and destroy red blood cells, leading to a range of symptoms that can vary from mild to life-threatening. The disease is most commonly found in specific regions, including parts of the United States, Europe, and Asia, where ticks carrying the parasite are prevalent.
The primary vector responsible for transmitting Babesiosis is the blacklegged tick, also known as the deer tick. These ticks are often found in wooded or grassy areas and are particularly active during warmer months. While Babesiosis shares some similarities with other tick-borne diseases like Lyme disease, it presents unique challenges due to its impact on the blood and immune system.
How is Babesiosis Transmitted?
Besides tick bites, Babesiosis can also be transmitted through other means:
- Blood transfusions: Infected blood products can unknowingly transmit the parasites to recipients.
- Congenital transmission: Pregnant individuals infected with the parasite can pass it to their unborn child.
- Organ transplantation: Rarely, infected organs donated for transplantation can transmit the disease.
Symptoms of Babesiosis
The symptoms of Babesiosis can vary widely depending on the individual’s age, overall health, and immune status. Some people may experience mild or no symptoms at all, while others may develop severe complications. Common symptoms include:
- Fever and chills
- Sweats and headaches
- Muscle aches and joint pain
- Fatigue and weakness
- Nausea and loss of appetite
In more severe cases, especially among individuals with weakened immune systems, the elderly, or those without a spleen, Babesiosis can lead to complications such as:
- Low blood pressure
- Severe anemia due to the destruction of red blood cells
- Organ failure, including kidney or liver damage
- Respiratory distress
When to Seek Medical Attention
If you live in or have recently visited an area where ticks are common and begin experiencing flu-like symptoms, it is important to seek medical attention promptly. Early diagnosis and treatment can prevent complications and improve outcomes. Inform your healthcare provider if you suspect you may have been bitten by a tick or exposed to ticks during outdoor activities.
Diagnosing Babesiosis
Diagnosing Babesiosis can be challenging because its symptoms often resemble those of other illnesses, such as the flu or malaria. Healthcare providers typically rely on a combination of clinical evaluation, patient history, and laboratory tests to confirm a diagnosis.
Laboratory Tests for Babesiosis
Several laboratory tests can help identify the presence of Babesia parasites in the blood:
- Blood smear examination: A stained blood sample is examined under a microscope to detect the presence of parasites within red blood cells.
- Polymerase chain reaction (PCR): This molecular test detects the genetic material of the parasite and is highly sensitive for diagnosing Babesiosis.
- Serologic testing: Blood tests that look for antibodies against Babesia can help confirm exposure to the parasite.
It is important to note that early-stage infections may produce negative results on some tests, so repeated testing may be necessary if the disease is strongly suspected.
Treatment Options for Babesiosis
Treatment for Babesiosis depends on the severity of the infection and the patient’s overall health. Mild cases may resolve on their own without specific treatment, but most patients require medication to eliminate the parasites and manage symptoms.
Medications Used to Treat Babesiosis
The standard treatment for Babesiosis involves a combination of two medications:
- Atovaquone: An antiprotozoal drug that inhibits the growth of the parasite.
- Azithromycin: An antibiotic that works synergistically with Atovaquone to enhance its effectiveness.
For severe cases, particularly in hospitalized patients, a different combination of drugs may be used:
- Clindamycin: An antibiotic administered intravenously to target the parasite.
- Quinine: A medication that helps reduce the number of parasites in the bloodstream.
In addition to these medications, supportive care may be necessary to manage complications such as anemia, low blood pressure, or organ dysfunction. Blood transfusions may be required in cases of severe anemia.
Preventing Babesiosis
Prevention is key to reducing the risk of Babesiosis, as there is currently no vaccine available to protect against the disease. Taking proactive measures to avoid tick bites is the most effective way to prevent infection.
Tips for Avoiding Tick Bites
Here are some practical steps to minimize your risk of encountering ticks:
- Wear protective clothing: When spending time outdoors in wooded or grassy areas, wear long sleeves, pants, and closed-toe shoes. Tuck pants into socks to create a barrier against ticks.
- Use insect repellents: Apply EPA-approved repellents containing DEET, picaridin, or permethrin to exposed skin and clothing.
- Perform regular tick checks: After being outdoors, thoroughly inspect your body, clothing, and gear for ticks. Pay special attention to areas such as the scalp, armpits, groin, and behind the knees.
- Shower after outdoor activities: Showering within two hours of coming indoors can help wash away unattached ticks.
- Treat pets: Use tick prevention products on pets to reduce the likelihood of bringing ticks into your home.
Creating a Tick-Safe Environment
You can also take steps to make your yard less hospitable to ticks:
- Keep grass mowed and remove leaf litter.
- Create a barrier of wood chips or gravel between wooded areas and recreational spaces.
- Discourage wildlife, such as deer and rodents, which can carry ticks, by using fencing or removing food sources.
Raising Awareness About Babesiosis
Educating the public about Babesiosis is crucial for early detection and prevention. Many people are unaware of the risks associated with tick bites or the potential severity of Babesiosis. Public health campaigns, community workshops, and informational resources can play a vital role in spreading awareness.
Healthcare Provider Education
Equipping healthcare providers with up-to-date information about Babesiosis is equally important. Clinicians should be trained to recognize the signs and symptoms of the disease, especially in regions where tick-borne illnesses are common. Improved diagnostic tools and standardized treatment protocols can further enhance patient outcomes.
Research and Development
Ongoing research into Babesiosis is essential for advancing our understanding of the disease and developing new strategies for prevention and treatment. Scientists are exploring potential vaccines, improved diagnostic methods, and novel therapies to combat this growing public health threat.
Living with Babesiosis
For individuals diagnosed with Babesiosis, managing the disease involves adhering to prescribed treatments and monitoring for any lingering effects. While most patients recover fully with appropriate care, some may experience prolonged fatigue or other post-infection symptoms. Staying informed and maintaining open communication with healthcare providers can help ensure a smooth recovery process.
Support Networks
Connecting with support groups or online communities can provide valuable emotional and practical support for individuals affected by Babesiosis. Sharing experiences and advice with others who have faced similar challenges can foster resilience and empowerment.