Autonomic dysfunction, also known as dysautonomia, refers to a group of conditions that affect the autonomic nervous system. The autonomic nervous system is responsible for regulating involuntary bodily functions such as heart rate, blood pressure, digestion, and temperature control. When this system malfunctions, it can lead to a wide range of symptoms and complications. This guide will explore the symptoms, causes, and treatments associated with autonomic dysfunction in detail.
Understanding the Autonomic Nervous System
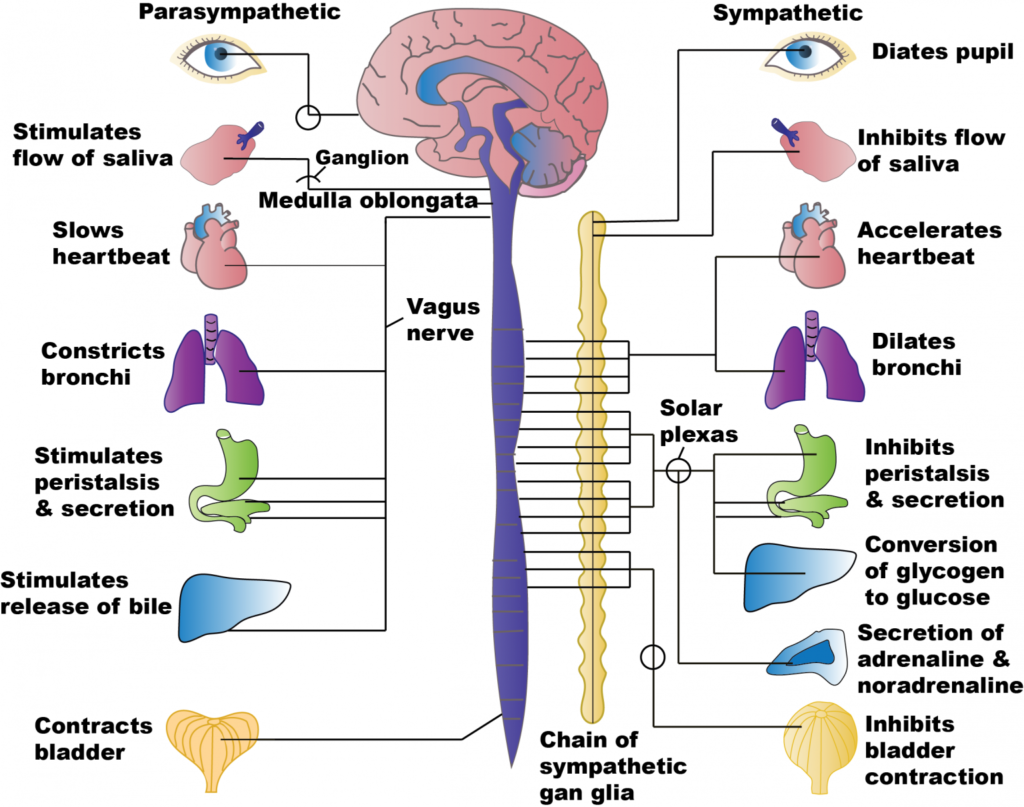
The autonomic nervous system is a critical part of the body’s overall nervous system. It operates without conscious control and is divided into two main branches:
- Sympathetic Nervous System: Often referred to as the “fight or flight” system, it prepares the body for stressful situations by increasing heart rate, dilating pupils, and redirecting blood flow to muscles.
- Parasympathetic Nervous System: Known as the “rest and digest” system, it promotes relaxation and recovery by slowing the heart rate, aiding digestion, and conserving energy.
When these systems are out of balance due to autonomic dysfunction, it can disrupt the body’s ability to maintain homeostasis.
Common Symptoms of Autonomic Dysfunction
The symptoms of autonomic dysfunction can vary widely depending on which parts of the autonomic nervous system are affected. Some of the most common symptoms include:
Cardiovascular Symptoms
- Dizziness or lightheadedness, especially when standing up (orthostatic hypotension)
- Rapid heart rate (tachycardia) or irregular heartbeats
- Fainting episodes (syncope)
Gastrointestinal Symptoms
- Bloating, nausea, or vomiting
- Constipation or diarrhea
- Difficulty swallowing
Thermoregulatory Symptoms
- Excessive sweating or inability to sweat
- Intolerance to heat or cold
Other Symptoms
- Fatigue and weakness
- Blurred vision
- Difficulty emptying the bladder completely
- Sleep disturbances
Causes of Autonomic Dysfunction
There are many potential causes of autonomic dysfunction, ranging from genetic factors to acquired conditions. Below are some of the most common causes:
Primary Causes
These are conditions that directly affect the autonomic nervous system:
- Pure autonomic failure: A degenerative condition that primarily affects autonomic nerve cells.
- Multiple system atrophy: A progressive neurological disorder that includes autonomic dysfunction as a key feature.
- Postural orthostatic tachycardia syndrome: A condition characterized by an abnormal increase in heart rate upon standing.
Secondary Causes
These are conditions or factors that indirectly lead to autonomic dysfunction:
- Diabetes: High blood sugar levels can damage autonomic nerves over time, leading to diabetic autonomic neuropathy.
- Autoimmune diseases: Conditions like lupus or Sjogren’s syndrome can attack the autonomic nervous system.
- Infections: Certain viral or bacterial infections, such as Lyme disease, can trigger autonomic dysfunction.
- Trauma: Injuries to the brain or spinal cord can disrupt autonomic pathways.
Genetic Factors
Some forms of autonomic dysfunction are inherited and linked to specific genetic mutations. For example, familial dysautonomia is a rare genetic disorder that affects the development and function of the autonomic nervous system.
Diagnosing Autonomic Dysfunction
Diagnosing autonomic dysfunction can be challenging because its symptoms often overlap with those of other medical conditions. Healthcare providers typically use a combination of methods to confirm a diagnosis:
Clinical Evaluation
- A thorough review of the patient’s medical history and symptoms.
- A physical examination to assess signs such as blood pressure changes, heart rate variability, and reflexes.
Diagnostic Tests
- Tilt table test: This evaluates how the body responds to changes in position and helps diagnose conditions like postural orthostatic tachycardia syndrome.
- Autonomic reflex screen: A series of tests that measure sweat production, heart rate variability, and blood pressure responses.
- Electromyography: Used to assess the health of muscles and the nerves that control them.
Treatment Options for Autonomic Dysfunction
While there is no cure for many forms of autonomic dysfunction, treatment focuses on managing symptoms and improving quality of life. The approach to treatment depends on the underlying cause and the specific symptoms experienced by the individual.
Lifestyle Modifications
Making certain lifestyle changes can help alleviate symptoms:
- Increase fluid and salt intake to combat low blood pressure.
- Wear compression stockings to improve circulation.
- Avoid triggers such as extreme temperatures or prolonged standing.
- Engage in regular, moderate exercise to enhance cardiovascular fitness.
Medications
Several medications may be prescribed to address specific symptoms:
- Fludrocortisone: Helps retain salt and water to raise blood pressure.
- Midodrine: Constricts blood vessels to prevent drops in blood pressure.
- Beta-blockers: May be used to regulate heart rate in cases of rapid heartbeat.
- Antidepressants: Can help manage pain and improve mood in some patients.
Physical Therapy
Physical therapy can play a crucial role in managing autonomic dysfunction:
- Gradual conditioning exercises to build strength and endurance.
- Techniques to improve balance and reduce the risk of falls.
- Breathing exercises to enhance parasympathetic activity and promote relaxation.
Specialized Treatments
In some cases, more advanced interventions may be necessary:
- Pacemakers: For individuals with severe heart rate abnormalities.
- Intravenous fluids: To stabilize blood pressure during acute episodes.
- Nerve blocks: To target specific areas of nerve dysfunction.
Living with Autonomic Dysfunction
Managing autonomic dysfunction requires a proactive approach and collaboration between patients and healthcare providers. Education about the condition is essential for making informed decisions about care. Support groups and counseling can also provide emotional support and practical advice for coping with daily challenges.
Tips for Daily Management
- Keep a symptom diary to track patterns and identify triggers.
- Stay hydrated and monitor electrolyte levels regularly.
- Prioritize rest and avoid overexertion.
- Communicate openly with your healthcare team about any new or worsening symptoms.
Research and Future Directions
Ongoing research is exploring new treatments and therapies for autonomic dysfunction. Advances in neurology, genetics, and regenerative medicine hold promise for better understanding and managing this complex condition. Patients are encouraged to stay informed about clinical trials and emerging options that may benefit their care.