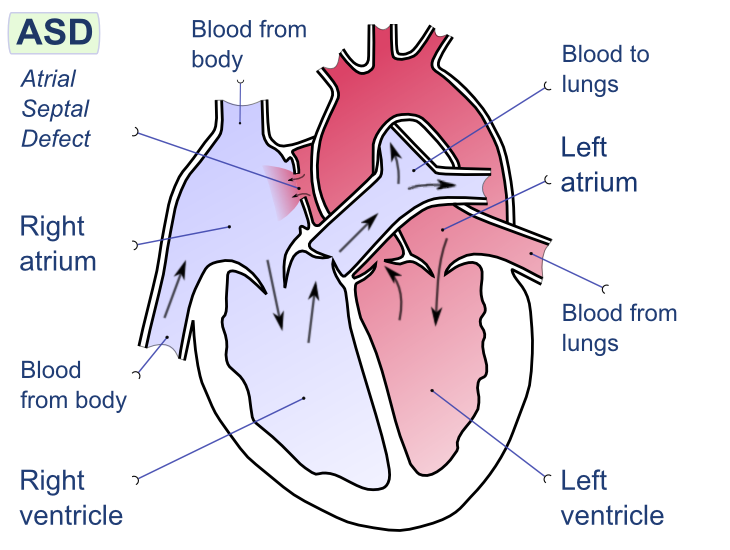
Atrial Septal Defect, commonly abbreviated as ASD, is a congenital heart condition that affects the structure of the heart. It occurs when there is an abnormal opening in the wall that separates the two upper chambers of the heart. This defect allows oxygen-rich blood to mix with oxygen-poor blood, leading to potential complications if left untreated. In this article, we will explore the details of this condition, including its causes, symptoms, diagnostic methods, and available treatment options.
Understanding Atrial Septal Defect
An atrial septal defect is a type of congenital heart defect, meaning it is present at birth. The heart has four chambers: two upper chambers called atria and two lower chambers called ventricles. The wall that separates the two atria is known as the atrial septum. In individuals with this condition, there is a hole or defect in the atrial septum, which disrupts the normal flow of blood through the heart.
This abnormality can vary in size, from small holes that may close on their own to larger defects that require medical intervention. The severity of the condition depends on the size of the defect and the amount of blood that flows between the two atria.
Causes of Atrial Septal Defect
The exact cause of this heart condition is not always clear, but several factors may contribute to its development. These include:
- Genetic Factors: Some cases are linked to genetic disorders, such as Down syndrome, which increases the likelihood of congenital heart defects.
- Environmental Factors: Exposure to certain substances during pregnancy, such as alcohol, drugs, or infections like rubella, can increase the risk.
- Developmental Issues: Problems during fetal development, particularly in the formation of the heart, can lead to this condition.
While some cases are inherited, many occur spontaneously without a clear family history.
Symptoms of Atrial Septal Defect
Not all individuals with this condition experience noticeable symptoms, especially in cases where the defect is small. However, as the defect grows or remains untreated, symptoms may become more apparent. Common signs and symptoms include:
- Shortness of Breath: Individuals may feel breathless during physical activity or even at rest.
- Fatigue: A general feeling of tiredness or exhaustion is common, especially after exertion.
- Swelling: Swelling in the legs, feet, or abdomen may occur due to fluid retention.
- Heart Palpitations: Irregular heartbeats or a sensation of fluttering in the chest may be experienced.
- Frequent Respiratory Infections: Children with this condition may have recurring lung infections.
- Growth Delays: In infants and young children, poor weight gain and delayed growth can be indicators.
In some cases, symptoms may not appear until adulthood, making early detection challenging. Regular check-ups and awareness of family medical history can aid in identifying the condition sooner.
Diagnosing Atrial Septal Defect
Diagnosing this heart condition typically involves a combination of physical examinations, imaging tests, and other diagnostic procedures. Early diagnosis is crucial for preventing complications and ensuring timely treatment.
Physical Examination
During a routine physical examination, a healthcare provider may detect signs of this condition by listening to the heart with a stethoscope. A characteristic heart murmur, caused by the abnormal flow of blood through the defect, is often one of the first indicators.
Imaging Tests
To confirm the presence of the defect and assess its size and location, doctors may order one or more imaging tests:
- Echocardiogram: This ultrasound of the heart provides detailed images of the heart’s structure and function. It is the primary tool used to diagnose this condition.
- Chest X-ray: An X-ray of the chest can reveal an enlarged heart or other abnormalities associated with the defect.
- Magnetic Resonance Imaging (MRI): In some cases, an MRI may be used to obtain more detailed images of the heart.
- Computed Tomography (CT) Scan: A CT scan can provide additional information about the heart’s anatomy.
Other Diagnostic Procedures
In addition to imaging tests, doctors may use the following methods to gather more information:
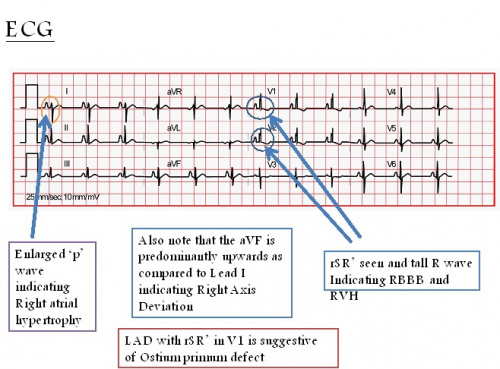
- Electrocardiogram (ECG): This test records the electrical activity of the heart and can detect irregular heart rhythms.
- Cardiac Catheterization: A thin tube is inserted into a blood vessel and guided to the heart to measure pressure and oxygen levels. This procedure is less common but may be used in complex cases.
Treatment Options for Atrial Septal Defect
Treatment for this condition depends on the size of the defect, the severity of symptoms, and the age of the individual. In some cases, no treatment may be necessary, while in others, medical or surgical interventions are required.
Observation and Monitoring
For small defects that do not cause symptoms, regular monitoring by a healthcare provider may be sufficient. Many small defects close on their own during infancy or early childhood. During this time, doctors will monitor the child’s growth, heart function, and overall health to ensure the defect does not worsen.
Medications
While medications cannot repair the defect itself, they can help manage symptoms and prevent complications. Commonly prescribed medications include:
- Diuretics: These medications help reduce fluid buildup in the body by promoting urine production.
- Beta-Blockers: These drugs can help regulate heart rate and reduce strain on the heart.
- Anticoagulants: Blood-thinning medications may be prescribed to prevent blood clots in individuals with larger defects.
Catheter-Based Procedures
For certain types of defects, a minimally invasive procedure called cardiac catheterization may be used to close the hole. During this procedure:
- A thin tube is inserted into a blood vessel, usually in the groin, and guided to the heart.
- A special device, such as an occluder, is placed over the defect to seal it.
- This approach avoids the need for open-heart surgery and typically results in a quicker recovery.
Surgical Repair
In cases where the defect is large or cannot be closed using catheter-based methods, open-heart surgery may be necessary. During surgery:
- The surgeon makes an incision in the chest to access the heart.
- The defect is repaired using a patch or stitches to close the hole.
- This procedure is highly effective but requires a longer recovery period.
Lifestyle Modifications
In addition to medical treatments, individuals with this condition may benefit from lifestyle changes to support heart health. These include:
- Maintaining a healthy diet low in salt and saturated fats.
- Engaging in regular, moderate exercise as recommended by a doctor.
- Avoiding smoking and excessive alcohol consumption.
- Managing stress through relaxation techniques or therapy.
Potential Complications
If left untreated, this condition can lead to serious complications, including:
- Heart Failure: The heart may become overworked and unable to pump blood effectively.
- Pulmonary Hypertension: Increased blood flow to the lungs can raise blood pressure in the pulmonary arteries.
- Stroke: Blood clots can form and travel to the brain, causing a stroke.
- Arrhythmias: Irregular heart rhythms may develop, increasing the risk of further complications.
Early diagnosis and treatment are essential for minimizing these risks and improving long-term outcomes.