Athlete’s Foot, also known as Tinea Pedis, is a common fungal infection that affects the skin on the feet. This condition is highly contagious and can spread easily in warm, moist environments such as locker rooms, showers, and swimming pools. While the abbreviation “TP” is sometimes used in medical contexts, this article will focus on providing a comprehensive understanding of the condition without relying on abbreviations.
What is Athlete’s Foot?
Athlete’s Foot is a fungal infection caused by a specific type of fungus called dermatophytes. These fungi thrive in warm, damp environments and feed on keratin, a protein found in the outer layer of the skin. The infection typically begins between the toes but can spread to other parts of the foot if left untreated. It is one of the most common fungal infections worldwide and affects people of all ages, though it is more prevalent among athletes and those who frequently wear tight or non-breathable footwear.
Causes of Athlete’s Foot
The primary cause of Athlete’s Foot is exposure to dermatophytes, which are microscopic fungi that live on dead tissue, such as skin, hair, and nails. Several factors can increase the risk of developing this condition:
- Damp Environments: Walking barefoot in public places like locker rooms, saunas, and communal showers increases the likelihood of coming into contact with the fungi.
- Poor Foot Hygiene: Failing to keep the feet clean and dry creates an ideal environment for fungi to grow.
- Tight Footwear: Shoes that do not allow proper ventilation trap moisture and heat, promoting fungal growth.
- Weakened Immune System: Individuals with compromised immune systems are more susceptible to infections, including Athlete’s Foot.
- Sharing Personal Items: Using someone else’s shoes, socks, or towels can lead to the transmission of the fungi.
How Does the Infection Spread?
Athlete’s Foot spreads through direct contact with infected skin or contaminated surfaces. For example, stepping on a floor where an infected person has walked barefoot can result in transmission. Additionally, scratching or touching an infected area and then touching another part of the body can cause the infection to spread to areas such as the hands or groin.
Symptoms of Athlete’s Foot
The symptoms of Athlete’s Foot can vary depending on the severity of the infection and the individual’s immune response. Common signs include:
- Itching and Burning: One of the earliest symptoms is intense itching, particularly between the toes. This may be accompanied by a burning sensation.
- Cracking and Peeling Skin: The skin between the toes often becomes dry, flaky, and prone to cracking. This can lead to discomfort and pain.
- Redness and Inflammation: Infected areas may appear red and swollen, indicating inflammation caused by the fungal infection.
- Blisters: In some cases, small blisters filled with fluid may form on the soles of the feet or between the toes.
- Odor: A foul smell may develop due to the combination of sweat and fungal activity.
Types of Athlete’s Foot
There are three main types of Athlete’s Foot, each with distinct characteristics:
- Interdigital: This is the most common form and affects the skin between the toes, especially the fourth and fifth toes.
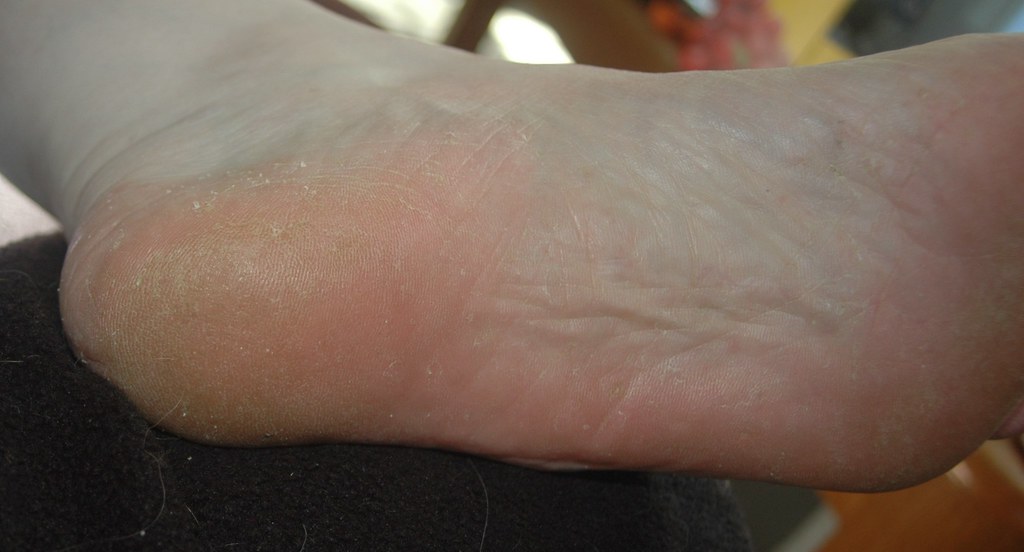
- Moccasin-Type: This type causes dry, scaly skin on the soles of the feet and may extend up the sides of the foot.
- Vesicular: Characterized by the sudden appearance of fluid-filled blisters, this form is less common but can be more painful.
Treatments for Athlete’s Foot
Treating Athlete’s Foot involves a combination of antifungal medications, lifestyle changes, and preventive measures. Early intervention is key to preventing the infection from worsening or spreading to other parts of the body.
Over-the-Counter Medications
For mild cases of Athlete’s Foot, over-the-counter antifungal treatments are often effective. These include:
- Creams and Ointments: Antifungal creams containing ingredients like clotrimazole, miconazole, or terbinafine are applied directly to the affected areas.
- Sprays and Powders: These products help reduce moisture and prevent the spread of fungi. They are particularly useful for treating shoes and socks.
- Lotions: Lotions provide a convenient way to apply medication to larger areas of the foot.
Prescription Medications
If over-the-counter treatments fail to resolve the infection, a healthcare provider may prescribe stronger antifungal medications. These may include:
- Oral Antifungal Drugs: Medications such as itraconazole or fluconazole are taken orally to target the infection from within.
- Topical Prescription Creams: These contain higher concentrations of active ingredients and are designed for more severe cases.
Home Remedies and Natural Treatments
In addition to conventional treatments, some individuals opt for home remedies to alleviate symptoms and support healing. While these methods are not substitutes for medical treatment, they can complement other therapies:
- Tea Tree Oil: Known for its antifungal properties, tea tree oil can be applied directly to the affected area after dilution with a carrier oil.
- Vinegar Soaks: Soaking the feet in a mixture of vinegar and water helps restore the skin’s natural pH balance, making it less hospitable to fungi.
- Ginger Tea Baths: Ginger has natural antifungal and anti-inflammatory properties that may help reduce symptoms.
Lifestyle Changes and Prevention
Preventing Athlete’s Foot requires adopting good hygiene practices and making lifestyle adjustments. Here are some tips to minimize the risk of infection:
- Keep Feet Dry: Always dry your feet thoroughly after bathing or swimming, paying special attention to the spaces between the toes.
- Wear Breathable Footwear: Choose shoes made from breathable materials like leather or mesh to allow air circulation.
- Change Socks Regularly: Wear clean, dry socks and change them at least once a day, or more frequently if your feet sweat heavily.
- Avoid Walking Barefoot: Wear sandals or flip-flops in public areas such as locker rooms, showers, and pool decks.
- Disinfect Shoes and Towels: Regularly wash and disinfect items that come into contact with your feet to prevent reinfection.
When to See a Doctor
While many cases of Athlete’s Foot can be managed at home, certain situations warrant professional medical attention. You should consult a healthcare provider if:
- The infection does not improve after two weeks of self-treatment.
- Symptoms worsen or become increasingly painful.
- You have diabetes or a weakened immune system, as these conditions increase the risk of complications.
- Secondary bacterial infections develop, indicated by increased redness, swelling, or pus.
Complications of Untreated Athlete’s Foot
If left untreated, Athlete’s Foot can lead to several complications, including:
- Spread to Other Areas: The infection can spread to the hands, nails, or groin, causing additional discomfort and requiring more extensive treatment.
- Bacterial Infections: Cracks in the skin caused by the infection can serve as entry points for bacteria, leading to secondary infections.
- Allergic Reactions: Some individuals may develop an allergic reaction to the fungi, resulting in widespread inflammation and itching.
Impact on Quality of Life
Chronic or severe cases of Athlete’s Foot can significantly impact an individual’s quality of life. Persistent itching, discomfort, and odor can affect self-esteem and social interactions. Addressing the condition promptly is essential to avoid long-term consequences.