Atelectasis, often abbreviated as AT, is a medical condition that refers to the partial or complete collapse of a lung or a section of it. This happens when the tiny air sacs in the lungs, known as alveoli, deflate or fill with fluid, preventing the normal exchange of oxygen and carbon dioxide. Atelectasis can occur due to various reasons and may affect people of all ages, from newborns to adults. Understanding this condition is crucial for early detection and effective management. In this article, we will explore the types, causes, symptoms, and treatment options available for this respiratory issue.
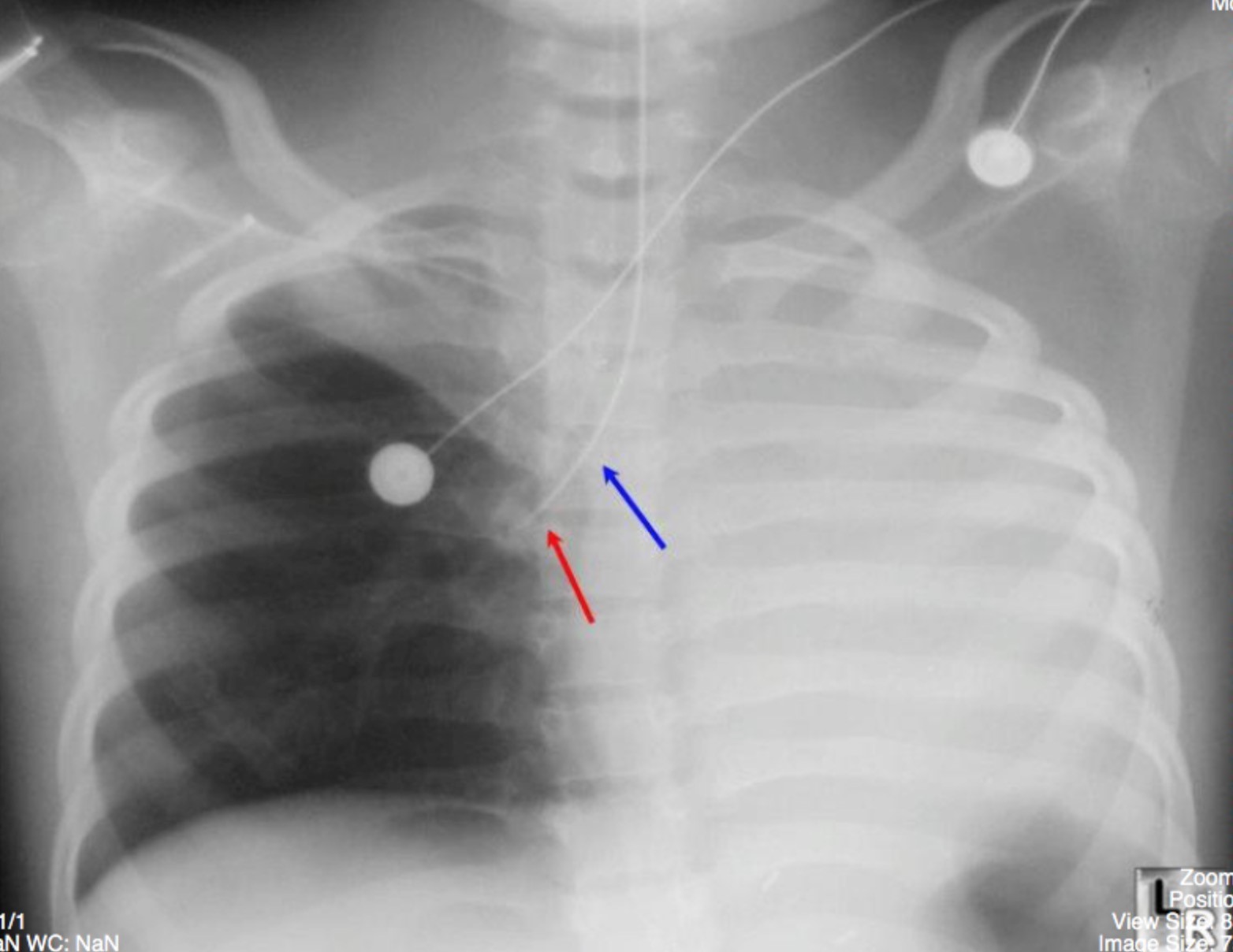
What Is Atelectasis?
Atelectasis occurs when part of the lung becomes airless and collapses. The lungs rely on the proper inflation of their air sacs to function correctly. When these air sacs collapse, the affected area of the lung cannot participate in the exchange of gases, leading to reduced oxygen levels in the blood. Depending on the severity and location of the collapse, atelectasis can cause mild discomfort or lead to life-threatening complications if left untreated.
How Does It Happen?
The process of atelectasis begins when something prevents the lungs from fully expanding. This could be due to an obstruction in the airways, pressure from outside the lungs, or a lack of surfactant, a substance that keeps the air sacs open. Without proper intervention, the collapsed portion of the lung may remain nonfunctional, leading to breathing difficulties and other complications.
Types of Atelectasis
Atelectasis can be classified into several types based on its underlying cause and mechanism. Each type has distinct characteristics and requires specific treatment approaches.
Obstructive Atelectasis
Obstructive atelectasis occurs when something blocks the airways, preventing air from reaching certain parts of the lung. Common causes include mucus plugs, tumors, foreign objects, or swollen tissues. When the airway is blocked, the air trapped beyond the obstruction is absorbed into the bloodstream, causing the lung tissue to collapse.
Nonobstructive Atelectasis
Nonobstructive atelectasis happens when the lung collapses without any blockage in the airways. This type can result from external pressure on the lungs, such as from a tumor, fluid buildup, or surgical complications. Other factors like chest injuries or certain medical conditions can also contribute to this form of atelectasis.
Compressive Atelectasis
Compressive atelectasis occurs when pressure from outside the lungs forces them to collapse. This can happen due to the presence of fluid, blood, or air in the pleural space, which is the area between the lungs and the chest wall. Conditions like pleural effusion or pneumothorax are common causes of compressive atelectasis.
Adhesive Atelectasis
Adhesive atelectasis happens when the lining of the lungs loses its ability to stick to the chest wall. This type is often seen in premature infants who lack sufficient surfactant, a substance that helps keep the air sacs open. Adhesive atelectasis can also occur in adults with certain lung diseases or after surgeries involving the chest.
Causes of Atelectasis
Atelectasis can result from a variety of factors, ranging from medical conditions to lifestyle choices. Identifying the root cause is essential for determining the appropriate treatment plan.
Post-Surgical Complications
One of the most common causes of atelectasis is surgery, particularly procedures involving the chest or abdomen. During surgery, patients are often placed under general anesthesia, which can suppress the normal functioning of the respiratory system. Shallow breathing or limited movement after surgery can lead to the collapse of lung tissue.
Respiratory Disorders
- Pneumonia: Infections in the lungs can cause inflammation and mucus buildup, leading to airway obstruction and subsequent lung collapse.
- Cystic Fibrosis: This genetic disorder causes thick mucus to accumulate in the airways, increasing the risk of atelectasis.
- Chronic Obstructive Pulmonary Disease (COPD): People with COPD may experience repeated episodes of atelectasis due to narrowed airways and weakened lung function.
Trauma and Injury
Chest injuries, such as rib fractures or blunt force trauma, can damage the lungs and surrounding structures. This damage can interfere with the normal expansion of the lungs, leading to atelectasis. Additionally, injuries that cause bleeding or fluid accumulation in the chest cavity can exert pressure on the lungs, causing them to collapse.
Foreign Objects
In children, swallowing small objects like toys or food particles can lead to airway obstruction and atelectasis. Adults may also experience this if they accidentally inhale foreign substances. Prompt removal of the object is critical to prevent further complications.
Prolonged Bed Rest
Individuals who are bedridden for extended periods, such as those recovering from surgery or suffering from severe illnesses, are at higher risk of developing atelectasis. Lack of movement can lead to shallow breathing and reduced lung expansion, increasing the likelihood of lung collapse.
Symptoms of Atelectasis
The symptoms of atelectasis can vary depending on the extent of lung involvement and the underlying cause. Some individuals may experience mild symptoms, while others may face more severe complications.
Mild Symptoms
- Shortness of breath, especially during physical activity
- Rapid, shallow breathing
- A persistent cough
Severe Symptoms
- Chest pain or discomfort
- Bluish discoloration of the skin due to low oxygen levels
- Fever, which may indicate an infection
- Increased heart rate
Diagnosis of Atelectasis
Diagnosing atelectasis typically involves a combination of physical examinations, imaging tests, and laboratory studies. Early and accurate diagnosis is essential to prevent complications and ensure timely treatment.
Physical Examination
During a physical exam, healthcare providers listen to the patient’s breathing using a stethoscope. Abnormal breath sounds, such as wheezing or crackling, may indicate lung collapse. Providers may also check for signs of low oxygen levels, such as rapid breathing or cyanosis.
Imaging Tests
- Chest X-ray: This is the most common diagnostic tool used to identify atelectasis. A chest X-ray can reveal areas of collapsed lung tissue and help determine the extent of the condition.
- CT Scan: Computed tomography provides detailed images of the lungs and can help identify the underlying cause of atelectasis, such as tumors or fluid buildup.
- Bronchoscopy: This procedure involves inserting a thin, flexible tube with a camera into the airways to examine them for obstructions or abnormalities.
Laboratory Tests
Blood tests may be performed to measure oxygen and carbon dioxide levels in the blood. Low oxygen levels can confirm the presence of atelectasis and help assess its severity.
Treatment Options for Atelectasis
The treatment of atelectasis depends on its cause, severity, and the patient’s overall health. The primary goal of treatment is to re-expand the collapsed lung tissue and address the underlying cause to prevent recurrence.
Physical Therapy and Breathing Exercises
For mild cases of atelectasis, physical therapy and breathing exercises are often recommended. Techniques such as deep breathing, incentive spirometry, and coughing can help reopen the airways and improve lung function. These exercises are particularly beneficial for post-surgical patients or those with prolonged bed rest.
Oxygen Therapy
Supplemental oxygen may be administered to patients with low oxygen levels. Oxygen therapy helps ensure that the body receives adequate oxygen while the lungs recover from the collapse.
Medications
- Bronchodilators: These medications help relax the muscles around the airways, making it easier to breathe.
- Mucolytics: Mucolytic drugs thin mucus, making it easier to clear from the airways and reducing the risk of obstruction.
- Antibiotics: If an infection is present, antibiotics may be prescribed to treat the underlying cause of atelectasis.
Drainage Procedures
In cases where fluid or air is compressing the lungs, drainage procedures may be necessary. For example, a chest tube can be inserted to remove excess fluid or air from the pleural space, allowing the lungs to re-expand.
Surgical Interventions
If atelectasis is caused by a tumor or other structural abnormalities, surgery may be required to remove the obstruction or repair damaged tissues. In some cases, minimally invasive procedures like bronchoscopy can be used to clear blockages without the need for major surgery.
Preventive Measures
Preventing atelectasis involves addressing risk factors and adopting healthy habits. Regular physical activity, avoiding smoking, and managing chronic respiratory conditions can significantly reduce the risk of developing this condition. Patients undergoing surgery should follow their healthcare provider’s recommendations for post-operative care, including breathing exercises and early mobilization.
Complications of Untreated Atelectasis
If left untreated, atelectasis can lead to serious complications that affect both the respiratory and cardiovascular systems. Understanding these potential risks underscores the importance of seeking prompt medical attention.
Low Oxygen Levels
Prolonged atelectasis can result in hypoxemia, a condition characterized by abnormally low levels of oxygen in the blood. This can lead to fatigue, confusion, and organ damage if not addressed promptly.
Pneumonia
Collapsed lung tissue creates an environment where bacteria can thrive, increasing the risk of pneumonia. This infection can further complicate recovery and may require aggressive treatment with antibiotics.
Respiratory Failure
In severe cases, atelectasis can progress to respiratory failure, a life-threatening condition where the lungs cannot provide enough oxygen to the body. Immediate medical intervention is necessary to stabilize the patient and restore lung function.