Asthma is a chronic respiratory condition that affects millions of people worldwide. Known for its recurring episodes of wheezing, shortness of breath, and chest tightness, this condition can significantly impact an individual’s quality of life if not properly managed. The term “asthma” itself comes from the Greek word meaning “panting” or “gasping,” which aptly describes the struggle many patients face during an asthma attack. For those unfamiliar with the condition, it may be referred to as bronchial asthma in medical contexts. Understanding what asthma is, its causes, symptoms, and management strategies is essential for both patients and caregivers.

What Is Asthma?
Asthma is a long-term inflammatory disease that primarily affects the airways, which are the tubes responsible for carrying air in and out of the lungs. In individuals with this condition, these airways become inflamed and narrow, making it difficult to breathe. This inflammation also leads to increased mucus production, further obstructing airflow. The severity of asthma can vary widely among individuals, ranging from mild and intermittent symptoms to severe and persistent challenges.
One of the defining characteristics of asthma is its episodic nature. People with this condition often experience periods of symptom-free living followed by sudden flare-ups, commonly referred to as asthma attacks. These attacks can be triggered by various factors, including allergens, infections, exercise, and even emotional stress. During an attack, the muscles around the airways tighten, causing them to constrict and making it harder for air to pass through.
Types of Asthma
- Allergic Asthma: Triggered by exposure to allergens such as pollen, dust mites, or pet dander.
- Non-Allergic Asthma: Caused by irritants like smoke, strong odors, or changes in weather.
- Exercise-Induced Asthma: Occurs during or after physical activity, particularly in cold or dry environments.
- Occupational Asthma: Develops due to exposure to workplace irritants such as chemicals or dust.
- Nocturnal Asthma: Symptoms worsen at night, disrupting sleep and leading to daytime fatigue.
Causes of Asthma
The exact cause of asthma remains unknown, but researchers believe it results from a combination of genetic and environmental factors. While some individuals may have a genetic predisposition to developing the condition, certain external triggers can exacerbate or initiate symptoms.
Genetic Factors
Family history plays a significant role in the development of asthma. If one or both parents have the condition, their children are more likely to develop it as well. Specific genes associated with the immune system and lung function have been identified as potential contributors to asthma susceptibility. However, having a genetic predisposition does not guarantee that an individual will develop asthma; environmental influences often act as catalysts.
Environmental Triggers
Environmental factors are critical in both the onset and worsening of asthma symptoms. Some common triggers include:
- Allergens: Substances such as pollen, mold spores, animal dander, and dust mites can provoke allergic reactions that lead to inflammation in the airways.
- Air Pollution: Exposure to pollutants like smog, tobacco smoke, and industrial emissions can irritate the respiratory system and trigger asthma symptoms.
- Infections: Respiratory infections, especially viral ones like the common cold or flu, can exacerbate asthma by increasing inflammation in the airways.
- Physical Activity: Exercise can induce symptoms in individuals with exercise-induced asthma, particularly when performed in cold or dry conditions.
- Emotional Stress: Strong emotions such as anxiety or excitement can sometimes lead to an asthma attack by affecting breathing patterns.
Symptoms of Asthma
Asthma symptoms can vary in intensity and frequency depending on the individual and the type of asthma they have. Some people experience mild symptoms that occur infrequently, while others may deal with severe and persistent issues. Recognizing these symptoms early is crucial for effective management and prevention of complications.
Common Symptoms
- Wheezing: A whistling or squeaky sound heard when breathing, especially during exhalation.
- Shortness of Breath: Difficulty catching one’s breath, even during minimal physical exertion.
- Chest Tightness: A feeling of pressure or constriction in the chest area.
- Coughing: Persistent coughing, particularly at night or early in the morning.
Signs of an Asthma Attack
An asthma attack occurs when symptoms suddenly worsen, requiring immediate attention. Key signs include:
- Rapid breathing accompanied by wheezing.
- Difficulty speaking due to extreme shortness of breath.
- Bluish tint to lips or fingernails caused by low oxygen levels.
- Feelings of panic or anxiety as breathing becomes increasingly labored.
Management of Asthma
While there is no cure for asthma, proper management can help control symptoms and reduce the risk of severe attacks. Effective management involves a combination of medication, lifestyle adjustments, and regular monitoring under the guidance of a healthcare provider.
Medications for Asthma
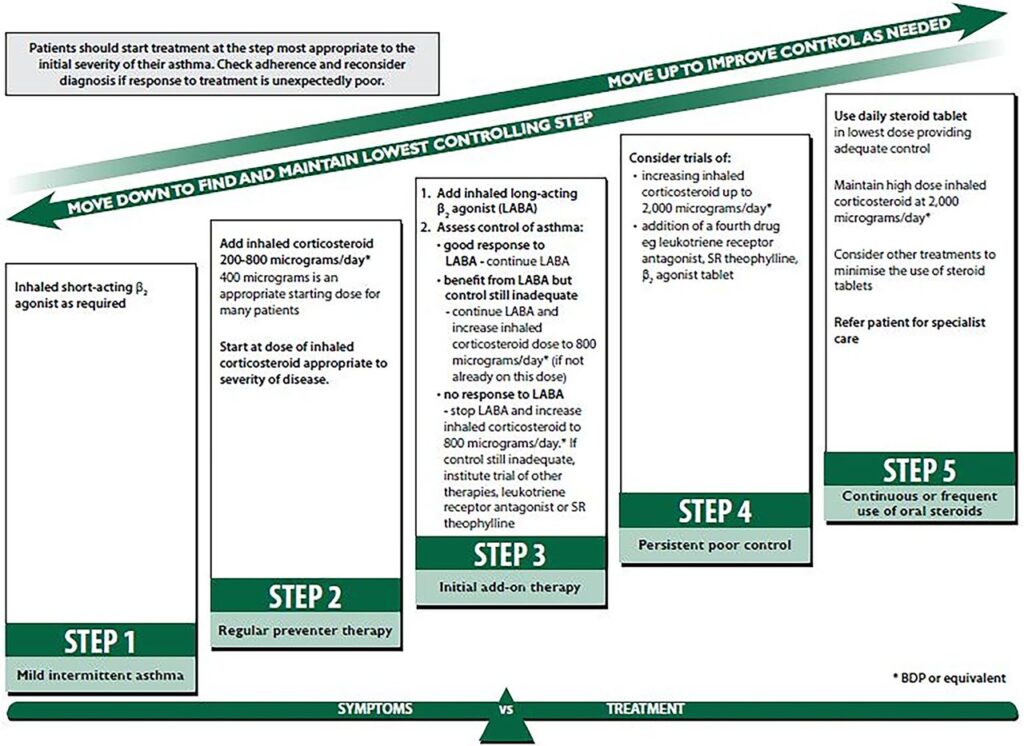
There are two main categories of medications used to treat asthma: controllers and relievers.
- Controllers: These medications are taken daily to prevent inflammation and keep symptoms under control. Examples include inhaled corticosteroids, leukotriene modifiers, and long-acting beta agonists.
- Relievers: Also known as rescue medications, these provide quick relief during an asthma attack. Short-acting beta agonists are commonly used for this purpose.
Lifestyle Adjustments
Making certain changes in daily habits can significantly improve asthma management:
- Avoid known triggers such as cigarette smoke, strong perfumes, and allergens.
- Maintain a clean living environment by regularly vacuuming, dusting, and washing bedding.
- Engage in regular physical activity, but consult a doctor about safe exercises for your condition.
- Adopt a balanced diet rich in fruits, vegetables, and omega-3 fatty acids to support overall health.
Monitoring and Education
Regular monitoring of lung function using tools like peak flow meters can help track the effectiveness of treatment plans. Additionally, educating oneself about the condition empowers patients to recognize warning signs and take proactive measures. Attending asthma education programs or support groups can provide valuable insights and foster a sense of community among individuals managing similar challenges.
Action Plans
Healthcare providers often recommend creating an asthma action plan tailored to each patient’s needs. This written document outlines steps to follow based on symptom severity, including when to use specific medications and when to seek emergency care. Having a clear plan in place ensures timely intervention and minimizes the risk of complications.
Living with Asthma
Managing asthma requires ongoing commitment and collaboration between patients, caregivers, and healthcare professionals. By understanding the nature of the condition, identifying personal triggers, and adhering to prescribed treatments, individuals can lead fulfilling lives despite their diagnosis. Regular check-ups and open communication with doctors are vital components of successful asthma management.
Support Systems
Building a strong support system can make a significant difference for those living with asthma. Family members, friends, teachers, and coworkers should be informed about the condition so they can offer assistance during emergencies. Support groups, both online and offline, provide opportunities to connect with others who share similar experiences, offering encouragement and practical advice.
Future Directions
Ongoing research continues to explore new treatments and therapies aimed at improving outcomes for individuals with asthma. Advances in biologic medications, immunotherapy, and personalized medicine hold promise for more targeted and effective interventions. Staying informed about these developments can empower patients to advocate for themselves and participate actively in their care.