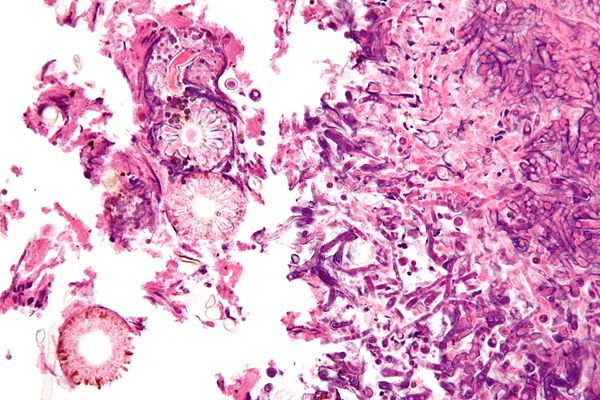
Aspergillosis, often abbreviated as ASP, is a group of diseases caused by fungi belonging to the Aspergillus species. These fungi are commonly found in the environment, particularly in decaying vegetation, soil, and dust. While most people breathe in Aspergillus spores daily without getting sick, individuals with weakened immune systems or underlying lung conditions may develop serious infections. This article explores the causes, symptoms, diagnosis, and treatments for this condition.
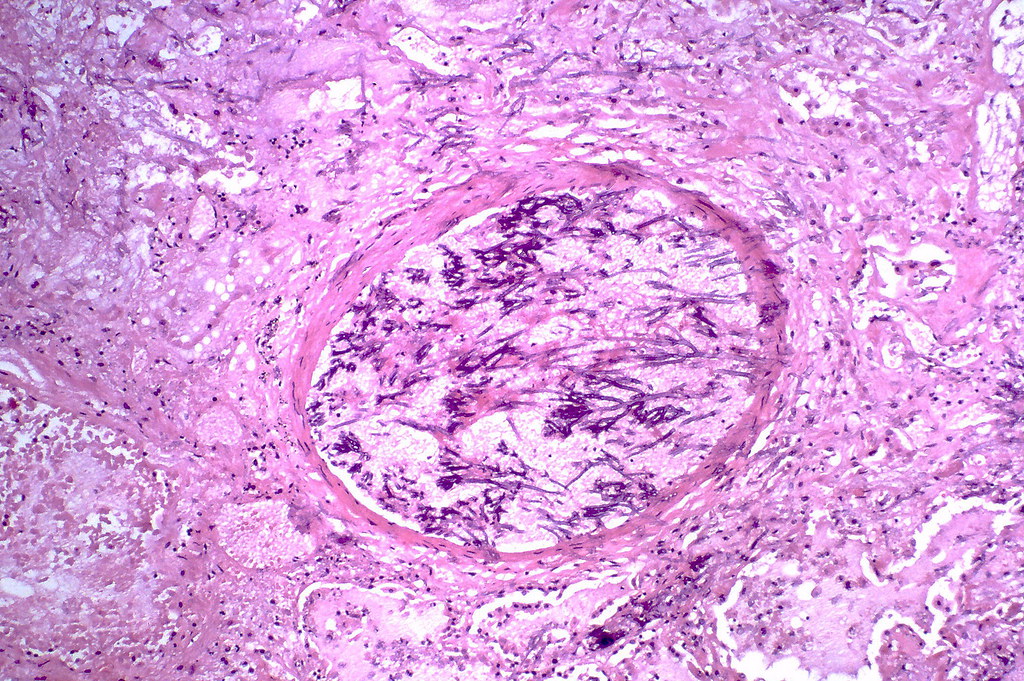
What Causes Aspergillosis?
The primary cause of aspergillosis is exposure to Aspergillus fungi. These fungi thrive in warm and humid environments, making them widespread in nature. When people inhale the tiny spores released by these fungi, they can settle in the respiratory system. For healthy individuals, the immune system typically eliminates these spores before they cause harm. However, certain factors increase the risk of developing aspergillosis:
- Weakened Immune System: People undergoing chemotherapy, organ transplants, or those with conditions like HIV/AIDS have compromised immune systems, making them more vulnerable to infection.
- Lung Conditions: Individuals with chronic obstructive pulmonary disease, asthma, or cystic fibrosis are at higher risk due to pre-existing damage to their respiratory systems.
- Environmental Exposure: Occupations such as farming, gardening, or construction expose workers to large amounts of Aspergillus spores, increasing the likelihood of infection.
- Prolonged Use of Medications: Long-term use of corticosteroids or other immunosuppressive drugs can reduce the body’s ability to fight off fungal infections.
Types of Aspergillosis and Their Symptoms
Aspergillosis manifests in various forms, depending on the part of the body affected and the individual’s immune response. Below are the most common types of aspergillosis and their associated symptoms:
Allergic Bronchopulmonary Aspergillosis
This type occurs when the immune system overreacts to Aspergillus spores in the lungs. It is most commonly seen in individuals with asthma or cystic fibrosis. Symptoms include:
- Wheezing and shortness of breath
- Coughing, sometimes accompanied by mucus or blood
- Fever and general fatigue
- Asthma flare-ups that do not respond well to standard treatments
Chronic Pulmonary Aspergillosis
Chronic pulmonary aspergillosis affects individuals with pre-existing lung conditions, such as tuberculosis or emphysema. It develops slowly over time and can lead to significant lung damage. Common symptoms include:
- Weight loss and reduced appetite
- Coughing up blood
- Fatigue and weakness
- Recurrent chest infections
Invasive Aspergillosis
Invasive aspergillosis is the most severe form and primarily affects individuals with severely weakened immune systems. The infection can spread from the lungs to other organs, such as the brain, heart, or kidneys. Symptoms vary depending on the organs involved but may include:
- Fever and chills
- Chest pain and difficulty breathing
- Headaches, seizures, or confusion if the infection spreads to the brain
- Swelling or pain in the sinuses if the infection begins there
Aspergilloma
An aspergilloma, also known as a “fungus ball,” forms when Aspergillus fungi grow in cavities within the lungs. This condition is often asymptomatic but can cause complications over time. Symptoms may include:
- A persistent cough
- Coughing up blood
- Shortness of breath during physical activity
How Is Aspergillosis Diagnosed?
Diagnosing aspergillosis can be challenging because its symptoms often mimic those of other respiratory conditions. A combination of tests is usually required to confirm the presence of Aspergillus infection. Some common diagnostic methods include:
Imaging Tests
Doctors often begin with imaging tests to assess the condition of the lungs and other organs:
- Chest X-rays: These can reveal abnormalities such as nodules, cavities, or masses in the lungs.
- Computed Tomography Scans: CT scans provide detailed images that help identify fungal growths or areas of inflammation.
Laboratory Tests
Laboratory tests are essential for detecting the presence of Aspergillus fungi or the body’s immune response to them:
- Sputum Culture: A sample of mucus coughed up from the lungs is examined under a microscope to check for fungal growth.
- Blood Tests: These measure levels of specific antibodies or antigens produced in response to Aspergillus infection.
- Bronchoscopy: A thin tube with a camera is inserted into the airways to collect tissue or fluid samples for analysis.
Biopsy
In some cases, a biopsy may be necessary to confirm the diagnosis. A small sample of affected tissue is removed and examined under a microscope for signs of fungal infection.
Treatment Options for Aspergillosis
The treatment for aspergillosis depends on the type and severity of the infection, as well as the patient’s overall health. Below are the main approaches used to manage this condition:
Antifungal Medications
Antifungal drugs are the cornerstone of aspergillosis treatment. They work by targeting and eliminating the fungi causing the infection. Commonly prescribed antifungal medications include:
- Voriconazole: Often used as the first-line treatment for invasive aspergillosis due to its effectiveness against Aspergillus species.
- Itraconazole: Typically prescribed for chronic pulmonary aspergillosis and allergic bronchopulmonary aspergillosis.
- Amphotericin B: Reserved for severe cases when other treatments fail, though it may cause significant side effects.
Corticosteroids
For allergic bronchopulmonary aspergillosis, corticosteroids are often combined with antifungal medications to reduce inflammation and control the immune system’s overreaction to the fungi.
Surgical Intervention
In cases where an aspergilloma causes severe symptoms or complications, surgery may be necessary to remove the fungal mass. Similarly, invasive aspergillosis that spreads to vital organs may require surgical intervention to prevent further damage.
Oxygen Therapy
Individuals with chronic pulmonary aspergillosis or invasive aspergillosis may experience difficulty breathing. Oxygen therapy can help improve oxygen levels in the blood and alleviate symptoms.
Lifestyle Modifications
While medical treatments are crucial, lifestyle changes can also play a role in managing aspergillosis:
- Avoiding environments with high concentrations of dust or mold
- Maintaining good hygiene to prevent secondary infections
- Adhering to prescribed medication regimens and attending regular follow-up appointments
Preventing Aspergillosis
Although it is impossible to completely avoid exposure to Aspergillus fungi, certain measures can reduce the risk of infection:
- Wearing masks in dusty or moldy environments, especially for those with weakened immune systems
- Using air purifiers to minimize airborne spores in indoor spaces
- Keeping living areas clean and free of moisture to prevent mold growth
- Seeking prompt treatment for respiratory symptoms to prevent complications