Arteriovenous malformation, commonly abbreviated as AVM, is a rare and complex condition that affects the blood vessels in the body. This disorder involves an abnormal connection between arteries and veins, disrupting the normal flow of blood. While arteriovenous malformations can occur anywhere in the body, they are most commonly found in the brain or spinal cord, where they can pose serious health risks if left untreated. Understanding this condition, its causes, symptoms, and treatment options is essential for early diagnosis and effective management.
What Is Arteriovenous Malformation?
An arteriovenous malformation occurs when there is an abnormal tangle of blood vessels connecting arteries and veins. In a healthy circulatory system, arteries carry oxygen-rich blood from the heart to various parts of the body, while veins return oxygen-depleted blood back to the heart. Capillaries, which are tiny blood vessels, act as intermediaries, allowing for the exchange of oxygen, nutrients, and waste products between blood and tissues.
In individuals with arteriovenous malformations, this process is disrupted because the capillaries are bypassed. Instead, arteries connect directly to veins through a tangled web of abnormal vessels. This direct connection increases the pressure within the veins, making them more prone to rupture. When these malformations occur in critical areas such as the brain or spinal cord, they can lead to severe complications, including bleeding, seizures, or neurological deficits.
How Common Are Arteriovenous Malformations?
Arteriovenous malformations are considered rare, affecting less than one percent of the general population. They are typically present at birth but may not cause noticeable symptoms until later in life. The exact prevalence of this condition is difficult to determine because many cases remain undiagnosed until complications arise. It is also important to note that arteriovenous malformations can vary significantly in size, location, and severity, which influences the symptoms and treatment approach.
Causes of Arteriovenous Malformations
The exact cause of arteriovenous malformations remains unknown. However, researchers believe that these malformations develop during fetal development, suggesting a congenital origin. During the early stages of pregnancy, the formation of blood vessels is a highly regulated process. Any disruption in this process can lead to the development of abnormal connections between arteries and veins.
Potential Risk Factors
While the precise cause is unclear, certain factors may increase the likelihood of developing arteriovenous malformations:
- Genetic Factors: Some evidence suggests that genetic mutations or hereditary conditions may play a role in the development of arteriovenous malformations. For example, individuals with hereditary hemorrhagic telangiectasia, a genetic disorder affecting blood vessels, are at a higher risk.
- Environmental Influences: Although no definitive environmental triggers have been identified, exposure to certain toxins or infections during pregnancy could potentially disrupt normal blood vessel development.
- Unknown Factors: In many cases, arteriovenous malformations occur sporadically without any identifiable cause or risk factors.
Symptoms of Arteriovenous Malformations
The symptoms of arteriovenous malformations depend largely on their size, location, and whether they have caused any complications. In some cases, individuals may remain asymptomatic for years, only discovering the condition after diagnostic imaging for unrelated issues. However, when symptoms do occur, they can range from mild to life-threatening.
Common Symptoms
When arteriovenous malformations affect the brain or spinal cord, they can produce a variety of neurological symptoms, including:
- Headaches: Persistent or severe headaches are one of the most common symptoms. These headaches may feel different from typical migraines and often worsen over time.
- Seizures: Abnormal electrical activity in the brain caused by the malformation can trigger seizures. These seizures may vary in intensity and frequency.
- Neurological Deficits: Depending on the location of the malformation, individuals may experience weakness, numbness, difficulty speaking, or problems with coordination and balance.
- Bleeding: One of the most serious complications of arteriovenous malformations is bleeding into the surrounding tissue. In the brain, this can result in a hemorrhagic stroke, which requires immediate medical attention.
Symptoms Based on Location
The location of the arteriovenous malformation plays a significant role in determining the specific symptoms experienced:
- Brain: Malformations in the brain can cause headaches, seizures, cognitive impairments, and sensory disturbances.
- Spinal Cord: When located in the spinal cord, arteriovenous malformations may lead to back pain, muscle weakness, or loss of bladder and bowel control.
- Other Areas: Although less common, arteriovenous malformations in other parts of the body, such as the lungs or liver, can cause localized pain, swelling, or dysfunction of the affected organ.
Diagnosis of Arteriovenous Malformations
Diagnosing arteriovenous malformations can be challenging, especially since many individuals remain asymptomatic until complications arise. However, several diagnostic tools and techniques can help identify and evaluate these malformations.
Imaging Techniques
Advanced imaging plays a crucial role in diagnosing arteriovenous malformations. Some of the most commonly used techniques include:
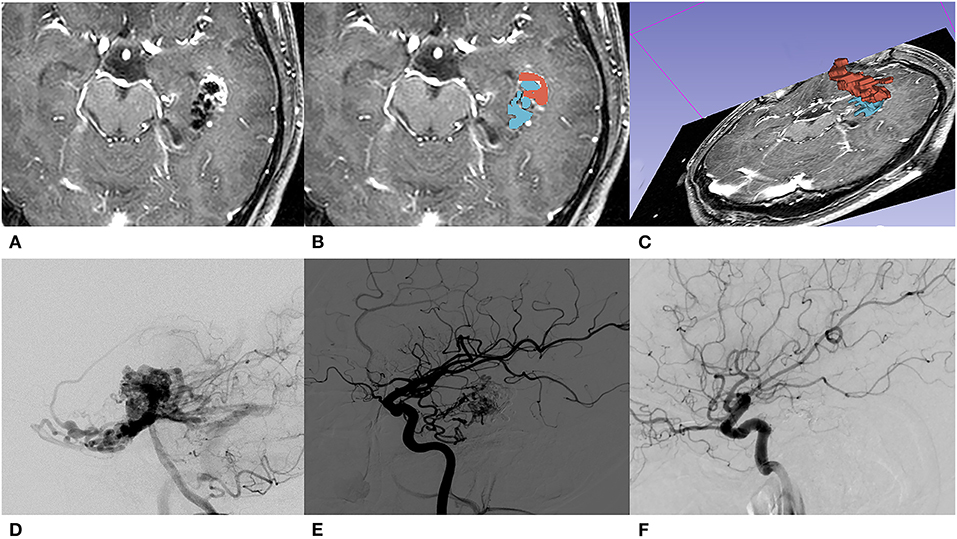
- Magnetic Resonance Imaging (MRI): MRI provides detailed images of the brain and spinal cord, making it an excellent tool for identifying arteriovenous malformations. It can also help assess the size, location, and potential impact of the malformation.
- Computed Tomography (CT) Scan: CT scans are particularly useful for detecting bleeding caused by ruptured arteriovenous malformations. They provide cross-sectional images of the affected area and can help guide treatment decisions.
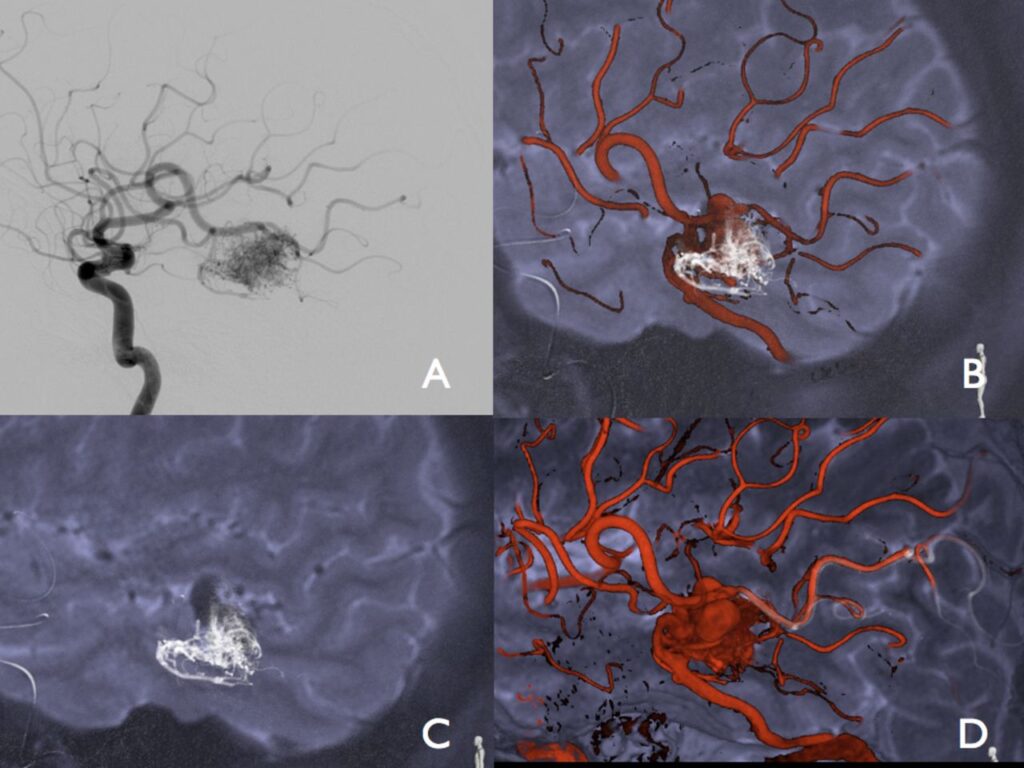
- Angiography: Also known as cerebral angiography, this procedure involves injecting a contrast dye into the blood vessels to visualize their structure. Angiography is considered the gold standard for diagnosing arteriovenous malformations and planning surgical interventions.
Additional Tests
In some cases, additional tests may be necessary to rule out other conditions or assess the extent of damage caused by the malformation:
- Electroencephalogram (EEG): An EEG measures electrical activity in the brain and can help identify seizure activity associated with arteriovenous malformations.
- Lumbar Puncture: If bleeding is suspected, a lumbar puncture may be performed to analyze cerebrospinal fluid for signs of blood.
Treatment Options for Arteriovenous Malformations
The treatment of arteriovenous malformations depends on several factors, including the size, location, and severity of the malformation, as well as the individual’s overall health and symptoms. In some cases, observation may be recommended for small, asymptomatic malformations. However, for larger or symptomatic malformations, more aggressive interventions may be necessary to prevent complications.
Observation and Monitoring
For individuals with small arteriovenous malformations that are not causing symptoms, regular monitoring may be the best course of action. This approach involves periodic imaging studies to track any changes in the size or structure of the malformation. Observation is often recommended for individuals who are at low risk of complications or who are not suitable candidates for more invasive treatments.
Surgical Removal
Surgical removal is a common treatment option for arteriovenous malformations that are accessible and pose a significant risk of bleeding or other complications. During surgery, a neurosurgeon carefully removes the abnormal blood vessels to restore normal blood flow. While surgery can be highly effective, it carries risks, including infection, bleeding, and damage to surrounding tissues.
Endovascular Embolization
Endovascular embolization is a minimally invasive procedure used to reduce blood flow to the arteriovenous malformation. During this procedure, a catheter is inserted into a blood vessel and guided to the site of the malformation. A special material, such as glue or coils, is then injected to block the abnormal vessels. Embolization is often used as a standalone treatment or in combination with surgery or radiation therapy.
Radiosurgery
Radiosurgery involves delivering highly focused beams of radiation to the arteriovenous malformation. Over time, the radiation causes the abnormal blood vessels to shrink and close off. This non-invasive treatment is particularly useful for malformations located in hard-to-reach areas of the brain. However, it may take months or even years for the full effects of radiosurgery to become apparent.
Combination Therapies
In some cases, a combination of treatments may be necessary to effectively manage arteriovenous malformations. For example, endovascular embolization may be used to reduce the size of the malformation before surgical removal or radiosurgery. The choice of treatment depends on the unique characteristics of the malformation and the individual’s specific needs.
Living with Arteriovenous Malformations
Managing arteriovenous malformations requires a multidisciplinary approach involving neurologists, neurosurgeons, radiologists, and other healthcare professionals. Regular follow-up appointments and imaging studies are essential to monitor the condition and detect any changes early. Additionally, individuals with arteriovenous malformations should be aware of potential warning signs, such as sudden severe headaches or neurological symptoms, and seek immediate medical attention if they occur.
While living with arteriovenous malformations can be challenging, advancements in diagnostic and treatment technologies have significantly improved outcomes for affected individuals. By staying informed and working closely with healthcare providers, individuals can take proactive steps to manage their condition and minimize the risk of complications.