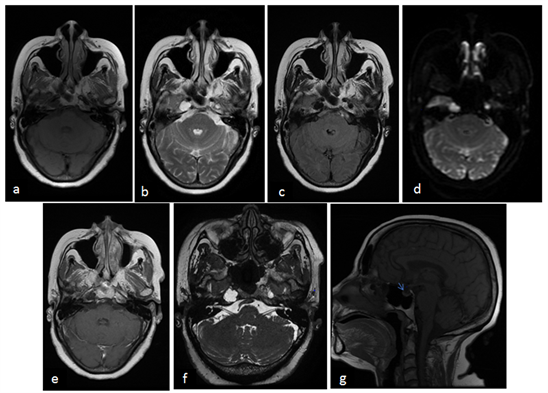
Arachnoid cysts, often abbreviated as ACs, are benign fluid-filled sacs that form within the arachnoid membrane, one of the three protective layers surrounding the brain and spinal cord. These cysts are typically filled with cerebrospinal fluid and can occur in various locations within the central nervous system. While many individuals with arachnoid cysts remain asymptomatic, others may experience a range of neurological symptoms depending on the size and location of the cyst. This article delves into the causes, symptoms, diagnostic methods, and treatment options for this condition.
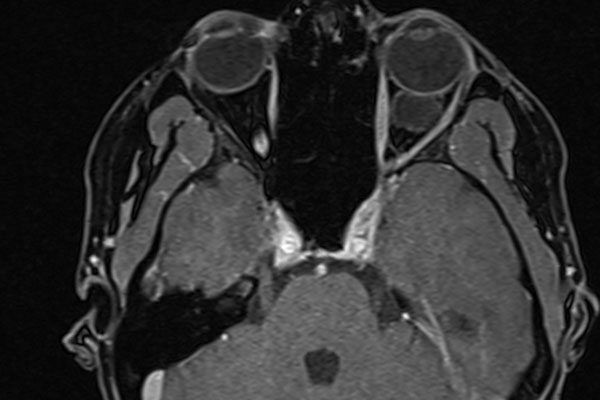
What Are Arachnoid Cysts?
Arachnoid cysts are congenital or acquired formations that develop between the arachnoid membrane and the underlying structures of the brain or spinal cord. They are most commonly found in the brain, particularly in areas such as the middle cranial fossa, the posterior fossa, and the suprasellar region. Less frequently, these cysts can also develop along the spine. The exact prevalence of arachnoid cysts is not well-documented, but they are considered relatively rare, affecting approximately one percent of the population.
Types of Arachnoid Cysts
- Congenital Arachnoid Cysts: These cysts are present at birth and are believed to arise due to abnormal development of the arachnoid membrane during fetal growth.
- Acquired Arachnoid Cysts: These cysts develop later in life and may result from trauma, infection, or complications following surgery.
Causes of Arachnoid Cysts
The exact cause of arachnoid cysts remains unclear, but researchers have identified several potential factors that may contribute to their formation. Understanding these causes is crucial for both prevention and management.
Congenital Factors
Congenital arachnoid cysts are thought to arise due to developmental abnormalities during fetal growth. During early brain development, the arachnoid membrane may fail to form properly, leading to the creation of a fluid-filled sac. Genetic predisposition may also play a role, although specific genes linked to arachnoid cysts have yet to be identified.
Trauma and Injury
In some cases, arachnoid cysts may develop as a result of head or spinal injuries. Trauma can damage the arachnoid membrane, causing cerebrospinal fluid to accumulate abnormally and form a cyst. This type of cyst is classified as an acquired arachnoid cyst.
Infections and Inflammation
Infections such as meningitis or inflammation of the central nervous system can lead to the formation of arachnoid cysts. These conditions may disrupt the normal flow of cerebrospinal fluid, creating pockets of fluid that eventually become cysts.
Surgical Complications
Rarely, surgical procedures involving the brain or spinal cord can result in the formation of arachnoid cysts. Post-surgical scarring or adhesions may interfere with the normal functioning of the arachnoid membrane, leading to cyst development.
Symptoms of Arachnoid Cysts
The symptoms associated with arachnoid cysts vary widely depending on their size, location, and whether they exert pressure on surrounding brain or spinal structures. Some individuals may remain asymptomatic throughout their lives, while others may experience significant neurological issues.
Common Symptoms
- Headaches: Persistent or severe headaches are one of the most frequently reported symptoms, especially when the cyst is located in the brain.
- Seizures: Seizures may occur if the cyst compresses brain tissue or disrupts electrical activity in the brain.
- Nausea and Vomiting: Increased intracranial pressure caused by the cyst can lead to nausea and vomiting.
- Balance and Coordination Issues: Cysts in the cerebellum or other parts of the brain responsible for motor control may result in difficulty walking or maintaining balance.
- Vision Problems: Blurred vision, double vision, or other visual disturbances may occur if the cyst affects the optic nerve or related structures.
Location-Specific Symptoms
Depending on where the cyst is located, it may produce unique symptoms:
- Suprasellar Region: Cysts in this area may cause hormonal imbalances, delayed puberty, or issues with growth.
- Posterior Fossa: These cysts may lead to hydrocephalus, a condition characterized by excessive accumulation of cerebrospinal fluid in the brain.
- Spinal Cord: Spinal arachnoid cysts can cause back pain, numbness, or weakness in the limbs.
Diagnosis of Arachnoid Cysts
Diagnosing arachnoid cysts requires a combination of clinical evaluation and advanced imaging techniques. Early and accurate diagnosis is essential to determine the appropriate course of treatment.
Medical History and Physical Examination
A healthcare provider will begin by taking a detailed medical history and performing a physical examination. Patients may be asked about the onset and duration of their symptoms, any history of head trauma, or family history of similar conditions.
Imaging Studies
Imaging plays a critical role in confirming the presence of an arachnoid cyst and assessing its size and location. Common imaging techniques include:
- Magnetic Resonance Imaging: MRI is the preferred method for diagnosing arachnoid cysts because it provides detailed images of the brain and spinal cord. It can distinguish between a cyst and other types of lesions.
- Computed Tomography Scan: CT scans are useful for identifying the presence of a cyst, although they may not provide as much detail as an MRI.
Differential Diagnosis
Other conditions, such as tumors, abscesses, or hydrocephalus, may mimic the symptoms of arachnoid cysts. A thorough evaluation is necessary to rule out these possibilities and ensure an accurate diagnosis.
Treatment Options for Arachnoid Cysts
The treatment approach for arachnoid cysts depends on several factors, including the size and location of the cyst, the severity of symptoms, and the patient’s overall health. Not all arachnoid cysts require intervention, particularly if they are small and asymptomatic.
Observation and Monitoring
For patients with small, asymptomatic cysts, regular monitoring may be the best course of action. Periodic imaging studies, such as MRI or CT scans, can help track any changes in the size or characteristics of the cyst over time.
Medication
In cases where symptoms such as headaches or seizures are present, medications may be prescribed to manage these issues. For example, anticonvulsant drugs can help control seizures, while pain relievers may alleviate headaches.
Surgical Interventions
Surgery is typically recommended for larger cysts or those causing significant symptoms. There are several surgical options available:
- Fenestration: This procedure involves creating a small opening in the cyst wall to allow cerebrospinal fluid to drain into surrounding areas.
- Shunt Placement: A shunt may be inserted to redirect excess cerebrospinal fluid from the cyst to another part of the body, such as the abdomen.
- Endoscopic Surgery: Minimally invasive endoscopic techniques can be used to remove or reduce the size of the cyst.
Recovery and Follow-Up
After surgery, patients will require close follow-up care to monitor recovery and ensure the cyst does not recur. Regular imaging studies and neurological assessments are typically part of the post-operative care plan.
Lifestyle Adjustments and Support
In addition to medical and surgical treatments, lifestyle adjustments can help improve quality of life for individuals with arachnoid cysts. These may include stress management techniques, dietary changes, and avoiding activities that could increase the risk of head injury. Support groups and counseling can also provide emotional support for patients and their families.
Emerging Research and Future Directions
Ongoing research aims to better understand the underlying causes of arachnoid cysts and develop more effective treatment strategies. Advances in imaging technology, minimally invasive surgical techniques, and genetic studies hold promise for improving outcomes for affected individuals.