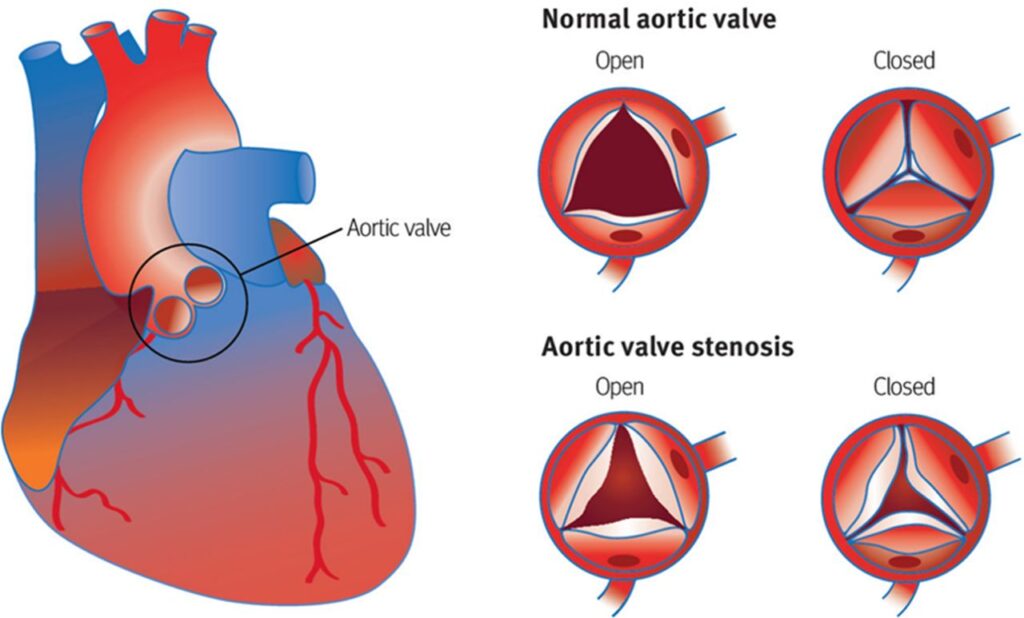
Aortic valve stenosis, often abbreviated as AS, is a serious heart condition that affects the aortic valve. This valve plays a critical role in ensuring proper blood flow from the heart to the rest of the body. When it becomes narrowed or stiff, it can lead to significant health complications. In this article, we will explore the causes, symptoms, diagnostic methods, and treatment options for this condition.
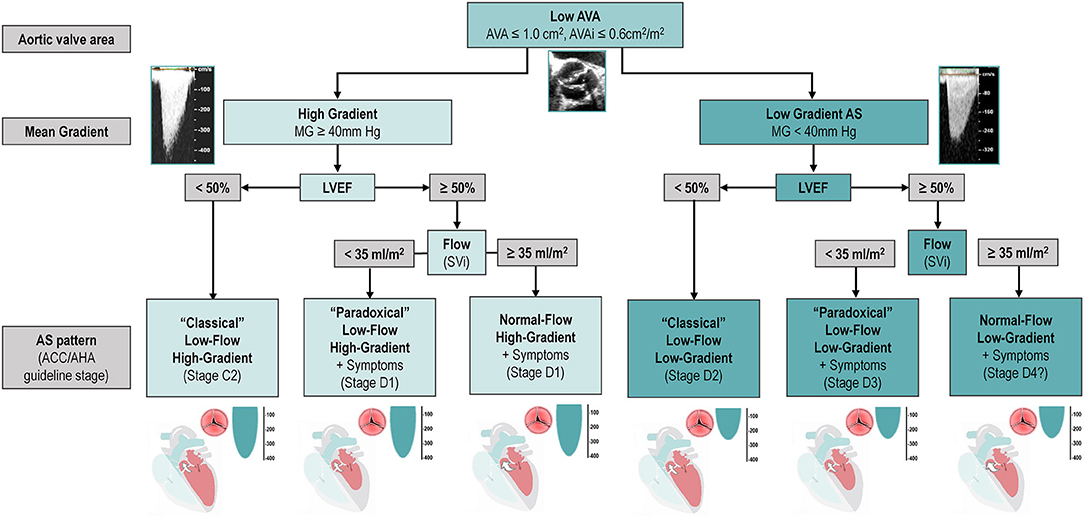
Understanding Aortic Valve Stenosis
The aortic valve is one of four valves in the heart that regulate blood flow. It is located between the left ventricle and the aorta, the main artery responsible for carrying oxygen-rich blood to the body. In a healthy heart, the aortic valve opens fully to allow blood to pass through without obstruction. However, in individuals with aortic valve stenosis, the valve does not open properly, leading to restricted blood flow.
This narrowing forces the heart to work harder to pump blood, which can eventually weaken the heart muscle and lead to complications such as heart failure. Understanding the underlying causes, recognizing the symptoms, and seeking timely medical intervention are essential for managing this condition effectively.
Causes of Aortic Valve Stenosis
Aortic valve stenosis can develop due to various factors. The most common causes include:
Age-Related Calcification
- As people age, calcium deposits can build up on the aortic valve, causing it to stiffen and narrow. This process is more common in individuals over the age of sixty-five.
Congenital Heart Defects
- Some individuals are born with an abnormal aortic valve. For example, a bicuspid aortic valve, which has two leaflets instead of the usual three, is more prone to narrowing over time.
Rheumatic Fever
- Rheumatic fever, a complication of untreated strep throat, can damage the aortic valve and lead to scarring. This scarring may cause the valve to narrow later in life.
Radiation Therapy
- In rare cases, radiation therapy used to treat cancer in the chest area can damage the heart valves, including the aortic valve.
Other Factors
- Chronic kidney disease and certain autoimmune conditions, such as lupus, may also contribute to the development of aortic valve stenosis.
Symptoms of Aortic Valve Stenosis
In its early stages, aortic valve stenosis may not produce noticeable symptoms. However, as the condition progresses, individuals may experience the following signs:
Chest Pain
- Chest pain, also known as angina, occurs when the heart muscle does not receive enough oxygen-rich blood. This pain may feel like pressure or tightness in the chest and can radiate to the arms, neck, or jaw.
Shortness of Breath
- Difficulty breathing, especially during physical activity or when lying down, is a common symptom. This occurs because the heart cannot pump enough blood to meet the body’s demands.
Fatigue
- Individuals with aortic valve stenosis often feel unusually tired or weak, even after minimal exertion. This fatigue is a result of reduced blood flow to the body’s tissues.
Dizziness or Fainting
- Dizziness or fainting spells, also known as syncope, may occur due to insufficient blood flow to the brain. These episodes can be alarming and require immediate medical attention.
Heart Murmur
- A heart murmur, an abnormal sound heard during a heartbeat, is often one of the first signs detected by a healthcare provider. It occurs due to turbulent blood flow through the narrowed valve.
Diagnosing Aortic Valve Stenosis
Early diagnosis of aortic valve stenosis is crucial for preventing complications. Healthcare providers use several methods to diagnose this condition:
Physical Examination
- During a routine check-up, a doctor may detect a heart murmur using a stethoscope. This finding often prompts further investigation.
Echocardiogram
- An echocardiogram uses sound waves to create detailed images of the heart. This test helps assess the structure and function of the aortic valve and measures the severity of the narrowing.
Electrocardiogram
- An electrocardiogram records the electrical activity of the heart. It can identify abnormalities such as an enlarged heart, which may indicate aortic valve stenosis.
Chest X-Ray
- A chest X-ray provides images of the heart and lungs. It can reveal an enlarged heart or calcium deposits on the aortic valve.
Cardiac Catheterization
- In some cases, a cardiac catheterization may be performed to measure the pressure difference across the aortic valve. This invasive procedure involves inserting a thin tube into a blood vessel and guiding it to the heart.
Magnetic Resonance Imaging
- Magnetic resonance imaging provides detailed images of the heart and can help assess the severity of the condition.
Treatment Options for Aortic Valve Stenosis
Treatment for aortic valve stenosis depends on the severity of the condition and the presence of symptoms. In mild cases, regular monitoring may be sufficient, while more severe cases may require surgical intervention.
Lifestyle Modifications
- For individuals with mild aortic valve stenosis, lifestyle changes can help manage symptoms and reduce the risk of complications. These include maintaining a healthy weight, exercising regularly, avoiding smoking, and managing conditions such as high blood pressure or diabetes.
Medications
- While medications cannot cure aortic valve stenosis, they can help manage symptoms and reduce the strain on the heart. Common medications include beta-blockers, calcium channel blockers, and diuretics.
Valve Repair or Replacement
- In severe cases, surgery may be necessary to repair or replace the damaged valve. There are two main types of valve replacement procedures:
- Mechanical Valve Replacement: This involves replacing the damaged valve with an artificial valve made of durable materials. While mechanical valves are long-lasting, patients must take blood-thinning medications for life to prevent blood clots.
- Biological Valve Replacement: Biological valves are made from animal tissue or human donor valves. They do not require lifelong blood-thinning medication but may need to be replaced after ten to fifteen years.
Transcatheter Aortic Valve Replacement
- Transcatheter aortic valve replacement is a minimally invasive procedure used for individuals who are not candidates for traditional open-heart surgery. It involves inserting a new valve through a catheter, typically via a blood vessel in the leg.
Balloon Valvuloplasty
- Balloon valvuloplasty is another minimally invasive procedure that involves inflating a balloon at the tip of a catheter to widen the narrowed valve. While effective for some patients, the results may not be permanent, and the procedure may need to be repeated.
Managing Aortic Valve Stenosis
Living with aortic valve stenosis requires ongoing care and collaboration with healthcare providers. Regular follow-ups are essential to monitor the progression of the condition and adjust treatment plans as needed. Patients should also be aware of warning signs, such as worsening chest pain or fainting, and seek immediate medical attention if these occur.
Education and support are vital components of managing aortic valve stenosis. Joining support groups or connecting with others who have the condition can provide valuable insights and emotional support. Additionally, staying informed about advancements in treatment options can empower patients to make informed decisions about their care.