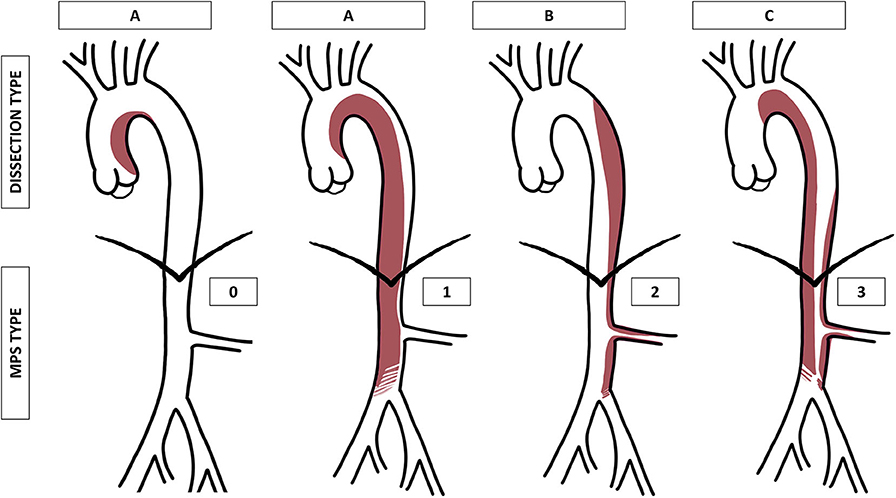
Aortic dissection, often abbreviated as AD, is a life-threatening condition that occurs when there is a tear in the inner layer of the aorta, the main artery responsible for carrying blood from the heart to the rest of the body. This tear allows blood to flow between the layers of the aortic wall, potentially leading to severe complications if not treated promptly. Understanding the causes, recognizing the symptoms, obtaining an accurate diagnosis, and exploring treatment options are critical steps in managing this serious medical emergency.
What Causes Aortic Dissection?
The primary cause of aortic dissection is a weakening or damage to the aortic wall, which can result from various factors. Below are some of the most common causes:
High Blood Pressure
- Chronic high blood pressure is one of the leading risk factors for aortic dissection. Over time, elevated pressure within the arteries can weaken the walls of the aorta, making them more susceptible to tearing.
Connective Tissue Disorders
- Conditions such as Marfan syndrome, Ehlers-Danlos syndrome, and Loeys-Dietz syndrome affect the strength and elasticity of connective tissues, including those in the aorta. These disorders increase the likelihood of aortic dissection due to structural weaknesses in the arterial walls.
Trauma
- Blunt trauma to the chest, such as that sustained during a car accident or fall, can cause a sudden tear in the aortic wall. This type of injury is often referred to as traumatic aortic dissection.
Atherosclerosis
- Hardening and narrowing of the arteries caused by plaque buildup can contribute to the development of aortic dissection. The presence of atherosclerosis weakens the arterial walls and increases the risk of tears.
Bicuspid Aortic Valve
- Individuals born with a bicuspid aortic valve, instead of the normal tricuspid valve, may have an increased risk of developing aortic dissection. This congenital condition often leads to abnormal blood flow patterns that place additional stress on the aortic wall.
Pregnancy
- In rare cases, pregnancy can be associated with aortic dissection, particularly in women who have underlying connective tissue disorders. The increased cardiovascular demands during pregnancy can exacerbate existing vulnerabilities in the aortic wall.
Symptoms of Aortic Dissection
Recognizing the symptoms of aortic dissection is crucial because timely intervention can save lives. The signs and symptoms vary depending on the location and severity of the tear but generally include:
Chest Pain
- The hallmark symptom of aortic dissection is sudden, severe chest pain. Patients often describe it as a sharp, tearing sensation that radiates to the back or abdomen. Unlike a heart attack, the pain associated with aortic dissection tends to move along the path of the aorta.
Shortness of Breath
- Difficulty breathing may occur if the dissection affects the part of the aorta near the heart or lungs. This symptom can indicate reduced blood flow to vital organs or fluid accumulation around the heart.
Fainting or Dizziness
- A sudden drop in blood pressure or interruption of blood flow to the brain can lead to fainting or dizziness. These symptoms should never be ignored, as they may signal a life-threatening complication.
Weakened Pulse
- In some cases, patients may notice differences in pulse strength between their arms or legs. For example, one arm might have a weaker pulse compared to the other, indicating restricted blood flow due to the dissection.
Stroke-Like Symptoms
- If the dissection extends into branches of the aorta supplying the brain, individuals may experience stroke-like symptoms such as difficulty speaking, weakness on one side of the body, or vision changes.
Abdominal Pain
- When the dissection involves the abdominal section of the aorta, patients may report severe abdominal pain accompanied by nausea or vomiting.
Diagnosing Aortic Dissection
Because the symptoms of aortic dissection overlap with those of other conditions, such as heart attacks or pulmonary embolisms, diagnosing it accurately requires careful evaluation using advanced imaging techniques. Here are the key diagnostic tools used:
Computed Tomography Angiography
- This imaging test uses X-rays and contrast dye to create detailed pictures of the aorta. Computed tomography angiography is highly effective at identifying tears and determining the extent of the dissection.
Magnetic Resonance Imaging
- Magnetic resonance imaging provides clear images of soft tissues without exposing patients to radiation. It is especially useful for assessing chronic or stable cases of aortic dissection.
Transesophageal Echocardiogram
- A transesophageal echocardiogram involves inserting a probe down the esophagus to capture ultrasound images of the heart and nearby structures. This method offers excellent visualization of the aorta and its branches.
Chest X-Ray
- While not definitive, a chest X-ray can reveal abnormalities such as widening of the aorta or fluid around the heart, prompting further investigation with more specialized tests.
Treatment Options for Aortic Dissection
The treatment approach for aortic dissection depends on several factors, including the location of the tear, the patient’s overall health, and the presence of complications. Treatment typically falls into two categories: surgical and medical management.
Surgical Management
Surgery is usually required for Type A dissections, which involve the ascending portion of the aorta closest to the heart. Common surgical procedures include:
- Aortic Root Replacement: In this procedure, the damaged section of the aorta is removed and replaced with a synthetic graft. If the aortic valve is also affected, it may be repaired or replaced simultaneously.
- Endovascular Repair: For certain types of dissections, minimally invasive techniques such as endovascular stent grafting may be performed. This involves inserting a fabric-covered metal tube through a small incision in the groin to reinforce the weakened area of the aorta.
Medical Management
Type B dissections, which affect the descending portion of the aorta, are often managed medically unless complications arise. Key components of medical management include:
- Blood Pressure Control: Medications such as beta-blockers and vasodilators are administered to lower blood pressure and reduce strain on the aortic wall.
- Pain Management: Strong analgesics are prescribed to alleviate severe pain, which can help prevent spikes in blood pressure caused by stress and discomfort.
- Monitoring: Regular follow-up appointments and imaging studies are essential to monitor the progression of the dissection and detect any new complications early.
Lifestyle Modifications
In addition to medical and surgical interventions, lifestyle changes play a significant role in preventing recurrence and promoting recovery:
- Dietary Adjustments: Adopting a heart-healthy diet low in sodium and saturated fats can help manage blood pressure and improve overall cardiovascular health.
- Exercise: Engaging in regular physical activity under medical supervision can strengthen the cardiovascular system while avoiding excessive strain.
- Smoking Cessation: Quitting smoking is imperative, as tobacco use accelerates the progression of atherosclerosis and increases the risk of complications.
Emerging Treatments and Research
Ongoing research continues to explore innovative approaches to treating aortic dissection. Some promising developments include:
- Genetic Testing: Advances in genetic testing allow doctors to identify individuals at higher risk of developing aortic dissection due to inherited connective tissue disorders.
- Novel Surgical Techniques: Researchers are refining minimally invasive procedures to make them safer and more accessible for a broader range of patients.
- Pharmacological Innovations: New medications targeting specific pathways involved in aortic wall degradation are being investigated to enhance long-term outcomes.
Understanding these advancements underscores the importance of staying informed about cutting-edge treatments and participating in clinical trials when appropriate.