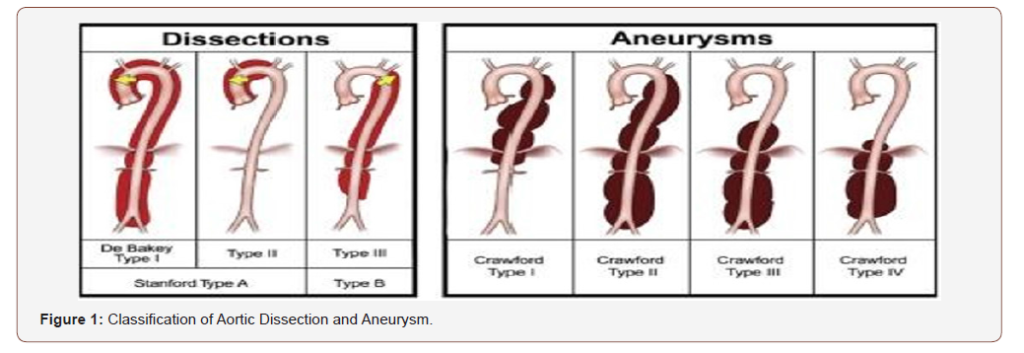
An aortic aneurysm, often abbreviated as AA, is a serious medical condition that occurs when the walls of the aorta weaken and bulge outward. The aorta is the largest blood vessel in the body, responsible for carrying oxygen-rich blood from the heart to the rest of the body. When an aneurysm develops, it poses a significant risk of rupture, which can lead to life-threatening internal bleeding. Understanding the causes, symptoms, and treatments of this condition is crucial for early detection and effective management.
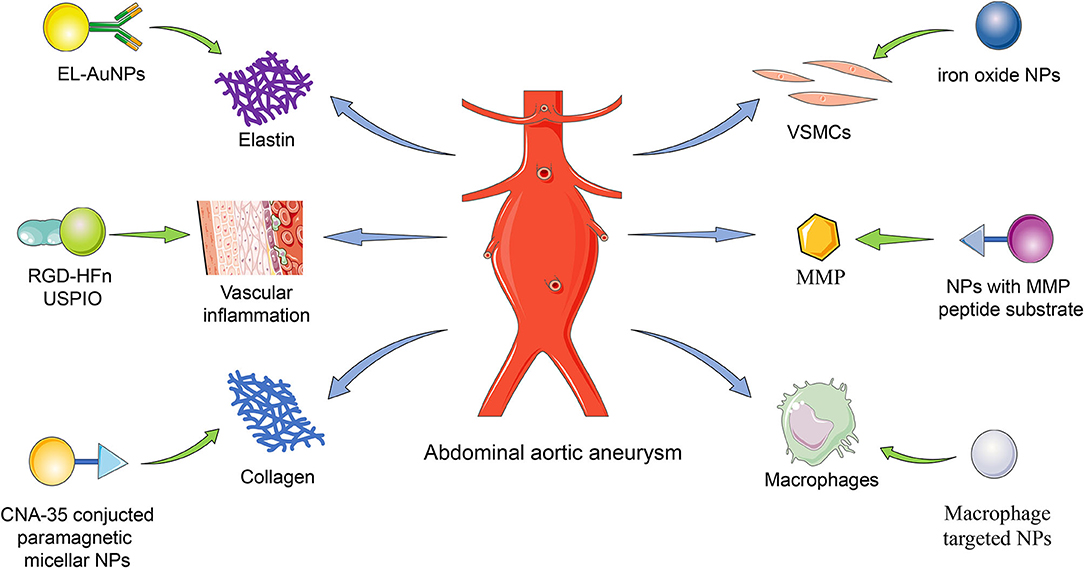
What Is an Aortic Aneurysm?
An aortic aneurysm is essentially a localized enlargement or bulging of the aorta. This condition can occur in different parts of the aorta, with two primary types being thoracic aortic aneurysms and abdominal aortic aneurysms. While both types share some similarities, their location, risk factors, and treatment options differ significantly.
- Thoracic Aortic Aneurysm: This type occurs in the part of the aorta that runs through the chest cavity.
- Abdominal Aortic Aneurysm: This type affects the portion of the aorta located in the abdomen.
Causes of Aortic Aneurysms
The exact cause of aortic aneurysms is not always clear, but several factors contribute to the weakening of the aortic walls. These include:
1. Age-Related Degeneration
As people age, the walls of the aorta naturally lose elasticity and strength. This degeneration makes them more susceptible to bulging under the pressure of blood flow. Most cases of aortic aneurysms are diagnosed in individuals over the age of sixty-five.
2. High Blood Pressure
Persistent high blood pressure places constant stress on the walls of the aorta. Over time, this increased pressure can weaken the walls and lead to the formation of an aneurysm. Managing blood pressure is therefore critical in reducing the risk of developing this condition.
3. Atherosclerosis
Atherosclerosis refers to the buildup of fatty deposits, cholesterol, and other substances on the inner walls of arteries. This process can damage the lining of the aorta, making it weaker and more prone to aneurysms.
4. Genetic Factors
Some individuals are genetically predisposed to developing aortic aneurysms. Conditions such as Marfan syndrome, Ehlers-Danlos syndrome, and Loeys-Dietz syndrome affect the connective tissues in the body, including those in the aorta. Family history also plays a role, as having a close relative with an aortic aneurysm increases one’s risk.
5. Infections and Inflammation
In rare cases, infections such as syphilis or salmonella can weaken the aortic walls. Additionally, inflammatory diseases like Takayasu arteritis or giant cell arteritis may contribute to the development of aneurysms.
6. Trauma
Physical trauma to the chest or abdomen, such as from a car accident or fall, can damage the aorta and increase the likelihood of an aneurysm forming.
Symptoms of Aortic Aneurysms
One of the challenges in diagnosing aortic aneurysms is that they often do not produce noticeable symptoms until they grow large or rupture. However, certain signs may indicate the presence of an aneurysm, depending on its location.
1. Thoracic Aortic Aneurysm Symptoms
When a thoracic aortic aneurysm grows large enough to press on nearby structures, it may cause the following symptoms:
- Chest pain or discomfort, often described as sharp or tearing
- Back pain
- Shortness of breath
- Hoarseness or difficulty swallowing
- Coughing
2. Abdominal Aortic Aneurysm Symptoms
Similarly, abdominal aortic aneurysms may remain asymptomatic until they expand or rupture. Potential symptoms include:
- Deep, constant pain in the abdomen or lower back
- A pulsating sensation near the navel
- Gastrointestinal issues, such as nausea or vomiting
3. Signs of Rupture
A ruptured aortic aneurysm is a medical emergency and requires immediate attention. Symptoms of rupture include:
- Sudden, severe pain in the chest, abdomen, or back
- Rapid heart rate
- Low blood pressure
- Dizziness or fainting
- Shock
Diagnosis of Aortic Aneurysms
Early diagnosis is essential for preventing complications associated with aortic aneurysms. Several diagnostic tools are used to identify and assess these conditions:
1. Physical Examination
During a routine checkup, a healthcare provider may detect an abdominal aortic aneurysm by feeling a pulsating mass in the abdomen. Similarly, a stethoscope may reveal abnormal sounds in the chest indicative of a thoracic aneurysm.
2. Imaging Tests
Imaging tests provide detailed views of the aorta and help determine the size, shape, and location of an aneurysm. Common imaging techniques include:
- Ultrasound: Uses sound waves to create images of the aorta.
- Computed Tomography (CT) Scan: Provides cross-sectional images of the body using X-rays.
- Magnetic Resonance Imaging (MRI): Uses magnetic fields and radio waves to produce detailed pictures.
3. Blood Tests
Blood tests may be performed to check for signs of infection or inflammation, which could suggest underlying causes of the aneurysm.
Treatment Options for Aortic Aneurysms
Treatment for aortic aneurysms depends on factors such as the size of the aneurysm, its location, and the patient’s overall health. The goal of treatment is to prevent the aneurysm from growing larger or rupturing.
1. Monitoring
Small aneurysms that are not causing symptoms may only require regular monitoring through imaging tests. Healthcare providers will track the growth of the aneurysm and intervene if it reaches a critical size or shows signs of rapid expansion.
2. Medications
Medications are often prescribed to manage risk factors and reduce the likelihood of complications. Common medications include:
- Beta-blockers: Help lower blood pressure and reduce stress on the aortic walls.
- Statins: Lower cholesterol levels to slow the progression of atherosclerosis.
- Antihypertensive drugs: Control high blood pressure.
3. Surgical Interventions
For larger or rapidly growing aneurysms, surgical intervention may be necessary. Two main types of surgery are used to treat aortic aneurysms:
a. Open Repair Surgery
This traditional approach involves making an incision in the chest or abdomen to access the aneurysm. The damaged section of the aorta is removed and replaced with a synthetic graft.
b. Endovascular Aneurysm Repair
This minimally invasive procedure involves inserting a catheter into an artery, usually in the groin, and guiding it to the site of the aneurysm. A stent graft is then deployed to reinforce the weakened area of the aorta.
4. Lifestyle Modifications
In addition to medical and surgical treatments, lifestyle changes can play a significant role in managing aortic aneurysms. Recommendations include:
- Quitting smoking to improve cardiovascular health
- Eating a balanced diet low in saturated fats and cholesterol
- Exercising regularly to maintain a healthy weight
- Managing stress to reduce blood pressure spikes
Preventing Aortic Aneurysms
While not all cases of aortic aneurysms can be prevented, certain measures can reduce the risk of developing this condition:
- Regular checkups to monitor blood pressure and cholesterol levels
- Screening for individuals with a family history of aortic aneurysms
- Avoiding tobacco use and limiting alcohol consumption
- Seeking prompt treatment for infections or inflammatory conditions
By understanding the causes, recognizing the symptoms, and exploring available treatments, individuals can take proactive steps toward safeguarding their cardiovascular health.