Anthrax, also known as Bacillus anthracis infection, is a serious infectious disease that affects both humans and animals. The name “anthrax” originates from the Greek word for coal, due to the characteristic black lesions it causes on the skin. While the disease is rare in humans, it remains a significant concern due to its potential use as a bioterrorism agent. Understanding the types of anthrax, how it spreads, its symptoms, and available treatments is crucial for prevention and management.
What is Anthrax?
Anthrax is caused by a bacterium called Bacillus anthracis. This organism forms spores, which are highly resistant structures that allow it to survive in harsh environmental conditions for long periods. These spores can be found naturally in soil and are most commonly associated with agricultural regions where livestock such as cattle, sheep, and goats are raised. Anthrax primarily affects herbivorous animals, but humans can become infected through contact with infected animals or contaminated animal products.
Types of Anthrax
Anthrax manifests in different forms depending on how the bacteria enter the body. Each type has distinct characteristics and levels of severity. Below are the main types of anthrax:
- Cutaneous Anthrax
- Inhalation Anthrax
- Gastrointestinal Anthrax
- Injection Anthrax
Cutaneous Anthrax
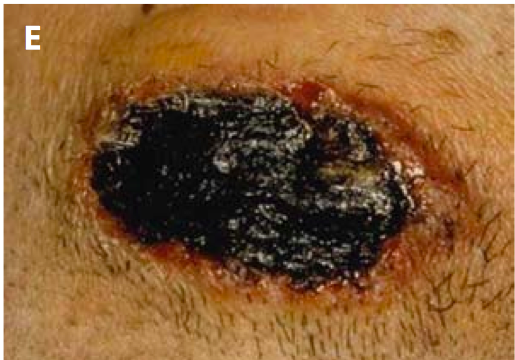
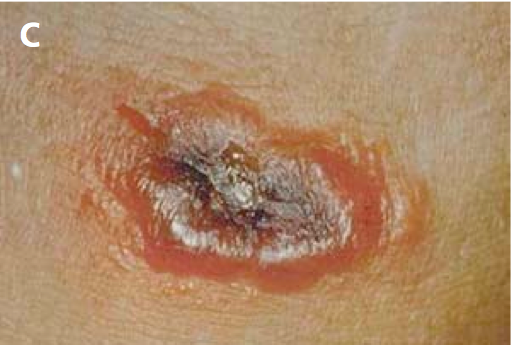
Cutaneous anthrax is the most common form of the disease and occurs when the spores of Bacillus anthracis enter the body through a cut or abrasion on the skin. It accounts for approximately ninety-five percent of all human cases. The initial symptom is usually a small, painless sore that develops into a blister. Over time, this blister turns into a black ulcer with a characteristic dark center. Swelling and redness around the sore may also occur. If left untreated, cutaneous anthrax can spread to the bloodstream and become life-threatening, although it is rarely fatal with proper medical care.
Inhalation Anthrax
Inhalation anthrax, also referred to as pulmonary anthrax, occurs when a person breathes in the spores of Bacillus anthracis. This form of the disease is particularly dangerous because it often presents with nonspecific symptoms at first, such as fever, fatigue, mild chest discomfort, and coughing. As the infection progresses, severe respiratory distress, shock, and even death can occur. Inhalation anthrax is considered one of the deadliest forms of the disease and is often associated with bioterrorism incidents.
Gastrointestinal Anthrax
Gastrointestinal anthrax results from consuming meat from an infected animal. The bacteria invade the gastrointestinal tract, leading to symptoms such as nausea, vomiting, abdominal pain, bloody diarrhea, and fever. In severe cases, the infection can spread to other parts of the body, including the bloodstream, causing systemic complications. Gastrointestinal anthrax is less common than cutaneous anthrax but carries a higher mortality rate if not promptly treated.
Injection Anthrax
Injection anthrax is a relatively new form of the disease that has emerged among individuals who inject drugs, particularly heroin. It resembles cutaneous anthrax but tends to progress more rapidly and severely. The infection can lead to deep tissue damage, abscess formation, and systemic illness. Injection anthrax poses unique challenges in diagnosis and treatment due to its association with drug use and the potential for delayed medical intervention.
How Anthrax Spreads
Anthrax transmission depends on the type of exposure. Here are the primary ways the disease spreads:
- Contact with Infected Animals: Humans can contract anthrax through direct contact with infected livestock or their products, such as hides, wool, or bones.
- Ingestion of Contaminated Meat: Eating undercooked or raw meat from an infected animal can lead to gastrointestinal anthrax.
- Inhalation of Spores: Breathing in airborne spores, either naturally occurring or intentionally released, can cause inhalation anthrax.
- Drug Use: Sharing needles or using contaminated substances can result in injection anthrax.
It is important to note that anthrax is not contagious between humans. Person-to-person transmission does not occur, making it different from many other infectious diseases.
Symptoms of Anthrax
The symptoms of anthrax vary depending on the type of infection. Early recognition of these symptoms is critical for timely diagnosis and treatment.
Symptoms of Cutaneous Anthrax
- A small, itchy bump on the skin that develops within a few days of exposure
- Formation of a painless ulcer with a black center
- Swollen lymph nodes near the affected area
Symptoms of Inhalation Anthrax
- Fever and chills
- Chest pain and shortness of breath
- Coughing, sometimes accompanied by blood-tinged sputum
- Rapid progression to severe respiratory distress
Symptoms of Gastrointestinal Anthrax
- Nausea and vomiting, which may include blood
- Severe abdominal pain and swelling
- Bloody diarrhea
- Fever and dehydration
Symptoms of Injection Anthrax
- Deep abscesses at the injection site
- Painful swelling and redness
- Fever and general malaise
Treatment Options for Anthrax
Early diagnosis and treatment are essential for improving outcomes in anthrax cases. Treatment typically involves antibiotics and supportive care tailored to the specific type of infection.
Antibiotic Therapy
Antibiotics are the cornerstone of anthrax treatment. Commonly prescribed medications include ciprofloxacin, doxycycline, and penicillin. The choice of antibiotic depends on factors such as the patient’s age, pregnancy status, and the severity of the infection. For inhalation and gastrointestinal anthrax, intravenous antibiotics are often required initially, followed by oral therapy to complete the course.
Supportive Care
In addition to antibiotics, patients with severe forms of anthrax may require intensive supportive care. This includes:
- Oxygen therapy for those experiencing respiratory distress
- Fluids and electrolyte replacement to address dehydration
- Pain management and wound care for cutaneous and injection anthrax
Vaccination
A vaccine against anthrax exists and is primarily used for individuals at high risk of exposure, such as laboratory workers, veterinarians, and military personnel. The vaccine requires multiple doses over several weeks and provides long-term protection when administered correctly. However, it is not routinely recommended for the general population.
Prevention Strategies
Preventing anthrax involves reducing exposure to the bacteria and implementing public health measures. Key strategies include:
- Vaccinating livestock in endemic areas to reduce the prevalence of the disease
- Proper handling and disposal of animal products to minimize contamination risks
- Educating healthcare providers and the public about recognizing early symptoms
- Implementing strict biosecurity protocols in laboratories and research facilities
Public Health Response to Bioterrorism Threats
Given the potential for anthrax to be used as a bioterrorism agent, governments and health organizations have developed emergency response plans. These plans focus on rapid detection, containment, and treatment of outbreaks. Stockpiles of antibiotics and vaccines are maintained to ensure swift action in the event of an attack.
Challenges in Managing Anthrax
Despite advances in medicine, managing anthrax presents several challenges:
- Delayed Diagnosis: The nonspecific early symptoms of inhalation and gastrointestinal anthrax can delay accurate diagnosis, allowing the infection to worsen.
- Antibiotic Resistance: Although rare, there is concern about the emergence of antibiotic-resistant strains of Bacillus anthracis.
- Limited Awareness: Many people are unfamiliar with anthrax, leading to missed opportunities for prevention and early treatment.
Research and Future Directions
Ongoing research aims to improve our understanding of anthrax and enhance diagnostic tools, treatments, and preventive measures. Scientists are exploring novel therapies, such as monoclonal antibodies, to complement traditional antibiotic approaches. Additionally, efforts are underway to develop faster and more reliable diagnostic tests to identify anthrax infections earlier.