Anhidrosis, also known as hypohidrosis in its milder form, refers to a condition where the body is unable to produce sweat adequately. This disorder can affect individuals of all ages and may occur in localized areas or across the entire body. While it might seem like a minor inconvenience, an inability to sweat can have serious consequences for overall health and well-being. In this article, we will explore what Anhidrosis is, its causes, symptoms, diagnosis methods, and available treatments.
What Is Anhidrosis?
Sweating is one of the body’s primary mechanisms for regulating temperature. When the body overheats, sweat glands release moisture onto the skin’s surface, which evaporates to cool the body down. Without this process, the body cannot maintain a stable internal temperature, leading to potential overheating and heat-related illnesses such as heatstroke. Anhidrosis occurs when these sweat glands fail to function properly, resulting in little to no sweat production.
How Does Sweating Work Normally?
To understand Anhidrosis, it is essential to first grasp how sweating works under normal circumstances. The human body contains millions of sweat glands distributed across the skin. These glands are controlled by the autonomic nervous system, which triggers them to release sweat when the body’s core temperature rises. Factors such as physical activity, environmental heat, and emotional stress can all stimulate sweat production.
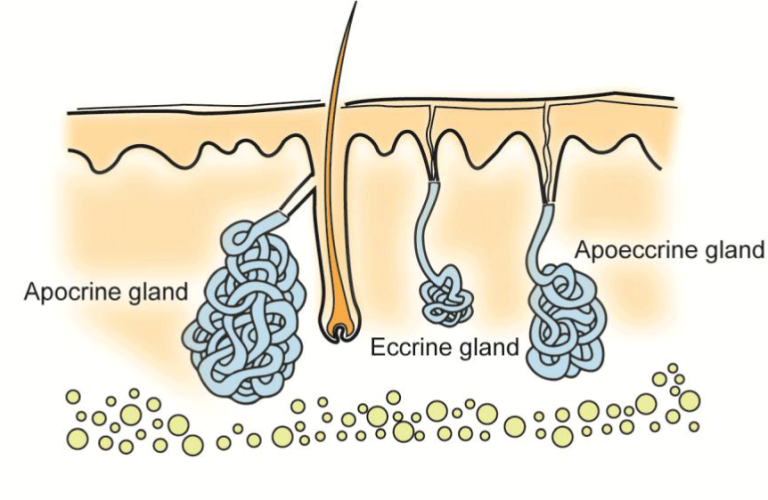
- Eccrine Glands: These are the most common type of sweat glands, found throughout the body. They produce a clear, odorless fluid primarily used for thermoregulation.
- Apocrine Glands: Located in areas like the armpits and groin, these glands become active during puberty and produce a thicker fluid that can mix with bacteria to cause body odor.
In individuals with Anhidrosis, one or both types of sweat glands may be affected, disrupting the body’s ability to cool itself effectively.
Causes of Anhidrosis
The causes of Anhidrosis can vary widely, ranging from genetic factors to acquired conditions. Below are some of the most common reasons why someone might develop this sweat disorder.
Genetic Disorders
Certain inherited conditions can interfere with the development or function of sweat glands. For example, a rare genetic disorder called congenital insensitivity to pain with anhidrosis prevents individuals from feeling pain or producing sweat. This condition is caused by mutations in specific genes responsible for nerve signaling.
Skin Damage
Injuries to the skin, such as severe burns, radiation therapy, or chronic skin diseases like psoriasis, can damage sweat glands and impair their ability to produce sweat. Similarly, certain cosmetic procedures, such as deep chemical peels, may inadvertently harm sweat gland function.
Nerve Damage
The autonomic nervous system plays a crucial role in regulating sweat production. Any condition that damages the nerves controlling sweat glands can lead to Anhidrosis. Examples include diabetes, multiple sclerosis, and spinal cord injuries. Nerve damage can also result from surgeries involving the chest or abdomen, where nerves connected to sweat glands may be severed or compressed.
Medications and Toxins
Some medications and toxins can interfere with sweat gland function. Anticholinergic drugs, often prescribed for conditions like overactive bladder or Parkinson’s disease, can reduce sweat production as a side effect. Additionally, exposure to heavy metals like mercury or arsenic may damage sweat glands over time.
Dehydration
Severe dehydration can temporarily impair the body’s ability to produce sweat. When the body lacks sufficient water, sweat glands cannot generate enough fluid to cool the body effectively. This is why staying hydrated is critical, especially in hot environments or during physical activity.
Symptoms of Anhidrosis
The symptoms of Anhidrosis can vary depending on the extent and location of the affected sweat glands. Some individuals may experience only mild discomfort, while others face significant health risks. Common signs and symptoms include:
- Dry skin in areas where sweating typically occurs
- Feeling excessively hot or overheated, even in moderate temperatures
- Muscle cramps or weakness during physical activity
- Dizziness or lightheadedness due to overheating
- Frequent episodes of heat exhaustion or heatstroke
In cases where Anhidrosis affects only specific parts of the body, individuals may notice contrasting patterns of sweating. For instance, they might sweat heavily on one side of the body but not at all on the other.
Diagnosing Anhidrosis
Diagnosing Anhidrosis involves a combination of medical history evaluation, physical examinations, and specialized tests. Since the symptoms of Anhidrosis can mimic those of other conditions, accurate diagnosis is essential for effective treatment.
Medical History and Physical Examination
A healthcare provider will begin by asking about the patient’s symptoms, including when they started and whether they worsen under certain conditions. They will also inquire about any underlying medical conditions, medications, or recent injuries that could contribute to the problem.
Sweat Tests
Several tests can measure sweat production and identify areas of reduced or absent sweating:
- Thermoregulatory Sweat Test: This test involves coating the skin with a powder that changes color when exposed to moisture. The patient is then placed in a heated chamber to induce sweating, allowing doctors to observe which areas of the body produce sweat.
- Quantitative Sudomotor Axon Reflex Test: Also known as QSART, this test uses electrodes to stimulate sweat glands and measures the amount of sweat produced.
Blood Tests and Imaging
In some cases, blood tests may be ordered to check for underlying conditions like diabetes or autoimmune disorders. Imaging studies, such as MRI or CT scans, may also be performed if nerve damage is suspected.
Treatment Options for Anhidrosis
While there is no universal cure for Anhidrosis, several strategies can help manage the condition and reduce the risk of complications. Treatment approaches depend on the underlying cause and severity of the disorder.
Lifestyle Modifications
For many individuals with Anhidrosis, making lifestyle changes is key to managing symptoms. These modifications include:
- Avoiding extreme heat and humidity whenever possible
- Staying hydrated by drinking plenty of water throughout the day
- Wearing loose, breathable clothing to promote airflow and prevent overheating
- Using cooling devices, such as fans or portable air conditioners, during warm weather
Addressing Underlying Conditions
If Anhidrosis is caused by another medical condition, treating that condition may improve sweat gland function. For example, better management of diabetes through medication and lifestyle changes can sometimes restore partial sweating ability. Similarly, addressing nutritional deficiencies or discontinuing problematic medications may alleviate symptoms.
Medical Interventions
In severe cases, medical interventions may be necessary to prevent complications. These could include:
- Prescription medications to stimulate sweat production
- Physical therapy to improve nerve function in cases of nerve damage
- Surgical options, though these are rare and typically reserved for extreme situations
Emergency Measures for Heat-Related Illnesses
Individuals with Anhidrosis are at higher risk of developing heat-related illnesses, such as heat exhaustion or heatstroke. It is crucial to recognize the warning signs and take immediate action:
- Move to a cooler environment immediately
- Apply cool, wet cloths to the skin to lower body temperature
- Drink cool water or electrolyte-rich beverages to rehydrate
- Seek emergency medical attention if symptoms do not improve quickly
Living with Anhidrosis
Managing Anhidrosis requires vigilance and proactive measures to protect against overheating. Education about the condition and awareness of personal triggers are vital components of living well with this sweat disorder. Support groups and online communities can provide valuable resources and encouragement for individuals navigating life with Anhidrosis.