An anal fissure, often abbreviated as AF, is a common yet painful condition that affects the lining of the anus. It is essentially a small tear or cut in the skin around the opening of the anus, which can cause significant discomfort and disrupt daily life. This article delves into the causes, symptoms, diagnosis, and treatment options for this condition, offering a comprehensive guide to understanding and managing it effectively.
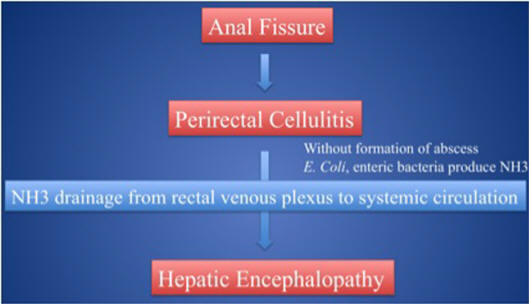
What is an Anal Fissure?
An anal fissure refers to a tear in the thin, moist tissue lining the anus. These fissures are typically located in the posterior midline of the anus but can also occur on the sides or front. While they are usually small, their impact on an individual’s quality of life can be substantial due to the associated pain and discomfort.
Types of Anal Fissures
- Acute Anal Fissures: These are short-term fissures that heal within a few weeks with proper care and treatment.
- Chronic Anal Fissures: If a fissure persists for more than six weeks, it is considered chronic and may require more intensive treatment.
Causes of Anal Fissures
The primary cause of anal fissures is trauma or injury to the anal canal. Several factors can contribute to the development of these tears:
Passing Hard Stools
One of the most common causes of anal fissures is passing hard or large stools during bowel movements. The excessive strain required to expel such stools can stretch and tear the delicate tissue around the anus.
Diarrhea
Frequent episodes of diarrhea can irritate and inflame the lining of the anus, making it more susceptible to tearing. The constant passage of loose stools can also prevent the area from healing properly.
Childbirth
During childbirth, the pressure exerted on the pelvic floor can lead to tears in the anal region. Women who experience difficult deliveries are particularly at risk of developing anal fissures.
Tight Anal Sphincter Muscles
Some individuals have naturally tight anal sphincter muscles, which can increase the likelihood of fissures. The tension in these muscles reduces blood flow to the area, impairing the healing process.
Underlying Medical Conditions
Certain medical conditions, such as Crohn’s disease, ulcerative colitis, and sexually transmitted infections, can predispose individuals to anal fissures. These conditions often cause inflammation and weaken the tissues in the anal region.
Symptoms of Anal Fissures
The symptoms of anal fissures are often unmistakable and can significantly affect an individual’s daily activities. Some of the most common symptoms include:
Pain During Bowel Movements
Individuals with anal fissures often experience sharp, stinging, or burning pain during bowel movements. This pain can persist for hours after the movement has ended.
Bleeding
Small amounts of bright red blood may appear on toilet paper or in the toilet bowl after a bowel movement. While alarming, this bleeding is usually minor and not a cause for concern unless it becomes excessive.
Itching and Irritation
The area around the anus may feel itchy or irritated due to the presence of the fissure. Scratching or rubbing the area can exacerbate the condition and delay healing.
A Visible Tear or Skin Tag
In some cases, individuals may notice a visible tear or a small lump near the anus, known as a sentinel pile or skin tag. This is a common sign of a chronic fissure.
Diagnosing Anal Fissures
Diagnosing an anal fissure typically involves a physical examination and a review of the patient’s medical history. In most cases, healthcare providers can identify a fissure by simply inspecting the anal area.
Physical Examination
During the examination, the healthcare provider will gently inspect the anus for signs of a tear, swelling, or other abnormalities. They may use a gloved finger or a specialized instrument called an anoscope to get a closer look at the anal canal.
Ruling Out Other Conditions
Since the symptoms of anal fissures can overlap with those of other conditions, such as hemorrhoids or anal abscesses, additional tests may be necessary. These tests can include:
- Digital Rectal Examination: A procedure where the healthcare provider inserts a gloved finger into the rectum to check for abnormalities.
- Anoscopy: The use of a small tube to examine the inside of the anus and lower rectum.
- Colonoscopy: In cases where underlying conditions like inflammatory bowel disease are suspected, a colonoscopy may be recommended to evaluate the entire colon.
Treatment Options for Anal Fissures
The treatment for anal fissures depends on their severity and duration. Most acute fissures heal on their own with conservative measures, while chronic fissures may require more advanced interventions.
Lifestyle and Home Remedies
For mild or acute fissures, simple lifestyle changes and home remedies can promote healing:
- Increase Fiber Intake: Consuming a diet rich in fiber can soften stools and reduce strain during bowel movements. Foods like fruits, vegetables, whole grains, and legumes are excellent sources of fiber.
- Stay Hydrated: Drinking plenty of water helps keep stools soft and prevents constipation.
- Sitz Baths: Soaking the anal area in warm water for 15 to 20 minutes several times a day can relieve pain and promote healing.
- Avoid Straining: Taking steps to avoid straining during bowel movements, such as using a footstool to elevate the legs, can reduce pressure on the anal region.
Medications
If home remedies are insufficient, medications may be prescribed to alleviate symptoms and accelerate healing:
- Topical Pain Relievers: Creams or ointments containing lidocaine can numb the area and provide temporary relief from pain.
- Nitroglycerin Ointment: This medication helps relax the anal sphincter muscles and improve blood flow to the area, promoting faster healing.
- Calcium Channel Blockers: Applied topically, these medications also help relax the anal sphincter and reduce pain.
- Stool Softeners: Over-the-counter or prescription stool softeners can make bowel movements easier and less painful.
Medical Procedures
For chronic or severe fissures that do not respond to conservative treatments, medical procedures may be necessary:
- Botox Injections: Injecting botulinum toxin into the anal sphincter can temporarily paralyze the muscle, reducing spasms and allowing the fissure to heal.
- Lateral Internal Sphincterotomy: This surgical procedure involves cutting a small portion of the anal sphincter muscle to reduce tension and improve blood flow to the area.
- Fissurectomy: In some cases, the fissure itself may be surgically removed to facilitate healing.
Preventing Anal Fissures
While not all anal fissures can be prevented, certain measures can significantly reduce the risk of developing them:
- Maintain a high-fiber diet to ensure regular and soft bowel movements.
- Drink plenty of fluids to stay hydrated and prevent constipation.
- Avoid prolonged sitting on the toilet, as this can increase pressure on the anal area.
- Engage in regular physical activity to promote healthy digestion and prevent constipation.
- Seek prompt treatment for any underlying medical conditions that may predispose you to fissures.
When to See a Doctor
While many anal fissures heal on their own, there are situations where medical attention is necessary:
- If the pain becomes unbearable or interferes with daily activities.
- If bleeding is heavy or persistent.
- If the fissure does not improve after several weeks of home treatment.
- If there are signs of infection, such as pus drainage or fever.
Consulting a healthcare provider ensures that the condition is properly diagnosed and treated, preventing complications and promoting faster recovery.