Alcoholic liver disease, often abbreviated as ALD, is a condition that results from excessive alcohol consumption over time. This condition encompasses a range of liver-related problems, including fatty liver, alcoholic hepatitis, and cirrhosis. In this article, we will explore the causes, symptoms, and care options for alcoholic hepatitis, a severe form of alcoholic liver disease.
Understanding Alcoholic Hepatitis
Alcoholic hepatitis is an inflammation of the liver caused by prolonged and excessive alcohol intake. It is one of the most serious forms of alcoholic liver disease and can lead to severe complications if not addressed promptly. Unlike other forms of hepatitis, such as viral hepatitis, alcoholic hepatitis is directly linked to alcohol consumption.
How Alcohol Affects the Liver
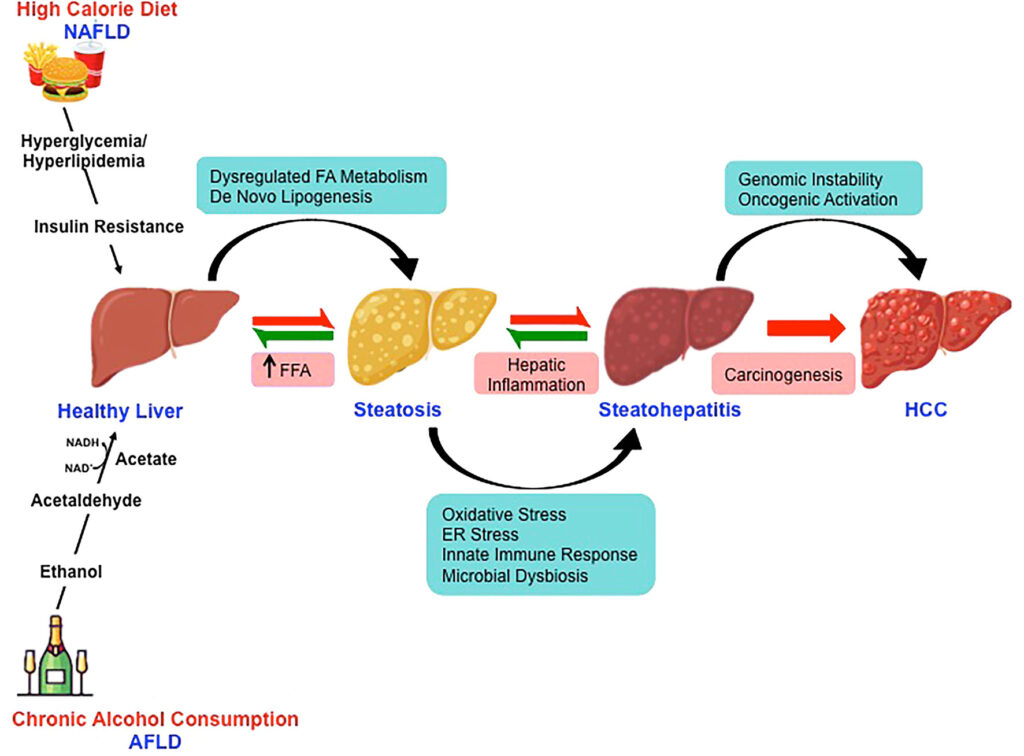
The liver plays a crucial role in processing alcohol. When alcohol is consumed, it is metabolized by the liver into acetaldehyde, a toxic substance that can damage liver cells. Over time, repeated exposure to alcohol leads to inflammation, scarring, and impaired liver function. The severity of alcoholic hepatitis depends on factors such as the amount and duration of alcohol consumption, genetic predisposition, and overall health.
Causes of Alcoholic Hepatitis
Excessive alcohol consumption is the primary cause of alcoholic hepatitis. However, several other factors can contribute to its development:
1. Quantity and Duration of Alcohol Consumption
- Heavy drinking over many years significantly increases the risk of developing alcoholic hepatitis.
- Women are more susceptible to alcohol-related liver damage than men due to differences in body composition and metabolism.
2. Genetic Factors
- Some individuals have genetic variations that affect how their bodies metabolize alcohol, making them more prone to liver damage.
- A family history of alcohol-related liver disease may also increase the risk.
3. Malnutrition
- Chronic alcohol use often leads to poor nutrition, which exacerbates liver damage.
- Vitamin deficiencies, particularly vitamin B1 (thiamine), can worsen the condition.
4. Coexisting Conditions
- Individuals with obesity or pre-existing liver conditions, such as non-alcoholic fatty liver disease, are at higher risk.
- Infections like hepatitis C can compound the effects of alcohol on the liver.
Symptoms of Alcoholic Hepatitis
The symptoms of alcoholic hepatitis can vary depending on the severity of the condition. Some individuals may experience mild symptoms, while others may develop life-threatening complications. Common signs and symptoms include:
1. Jaundice
- Yellowing of the skin and eyes is one of the hallmark signs of liver dysfunction.
- This occurs due to the buildup of bilirubin, a substance normally processed by the liver.
2. Abdominal Pain and Swelling
- Pain or discomfort in the upper right abdomen is common.
- Swelling in the abdomen, known as ascites, may occur due to fluid accumulation.
3. Fatigue and Weakness
- Chronic fatigue and weakness are frequent complaints among individuals with alcoholic hepatitis.
- These symptoms are often attributed to the body’s inability to metabolize nutrients effectively.
4. Nausea and Vomiting
- Frequent nausea and vomiting can result from liver inflammation and impaired digestion.
- These symptoms may worsen after consuming alcohol.
5. Loss of Appetite and Weight Loss
- A diminished appetite and unintended weight loss are common in advanced cases.
- This is often due to malnutrition and the body’s reduced ability to absorb nutrients.
6. Fever
- Low-grade fever may accompany alcoholic hepatitis, indicating an inflammatory response.
- Fever should be monitored closely, as it can signal infection or worsening liver damage.
7. Confusion and Cognitive Impairment
- In severe cases, individuals may experience confusion, memory problems, or difficulty concentrating.
- This is often a sign of hepatic encephalopathy, a condition caused by the liver’s inability to remove toxins from the blood.
Diagnosis of Alcoholic Hepatitis
Diagnosing alcoholic hepatitis involves a combination of medical history, physical examination, and diagnostic tests. Healthcare providers typically follow these steps:
1. Medical History and Physical Examination
- Doctors will inquire about alcohol consumption patterns, dietary habits, and any family history of liver disease.
- A physical exam may reveal signs such as jaundice, abdominal swelling, or an enlarged liver.
2. Blood Tests
- Blood tests can assess liver function and detect elevated levels of liver enzymes, bilirubin, and other markers of inflammation.
- Tests for nutritional deficiencies and infections may also be conducted.
3. Imaging Studies
- Ultrasound, CT scans, or MRI may be used to visualize the liver and identify abnormalities such as scarring or swelling.
- Imaging can help rule out other potential causes of liver disease.
4. Liver Biopsy
- In some cases, a small sample of liver tissue may be taken for analysis to confirm the diagnosis and assess the extent of damage.
- This procedure is typically reserved for complex or unclear cases.
Treatment and Care for Alcoholic Hepatitis
Managing alcoholic hepatitis requires a comprehensive approach that addresses both the underlying cause and the symptoms. Treatment options include:
1. Abstinence from Alcohol
- The single most important step in treating alcoholic hepatitis is complete abstinence from alcohol.
- Continued alcohol consumption can lead to rapid progression of liver damage and even death.
2. Nutritional Support
- A balanced diet rich in vitamins and minerals is essential for recovery.
- Supplements may be prescribed to address specific deficiencies, such as thiamine or folate.
3. Medications
- Corticosteroids may be prescribed to reduce inflammation in severe cases.
- Other medications, such as pentoxifylline, may be used to improve liver function and reduce complications.
4. Management of Complications
- Treatment for complications such as ascites, hepatic encephalopathy, or infections may be necessary.
- Hospitalization may be required for individuals with severe symptoms or complications.
5. Liver Transplant
- In cases of advanced liver failure, a liver transplant may be considered.
- However, candidates must demonstrate a commitment to long-term sobriety before being eligible for transplantation.
Prevention of Alcoholic Hepatitis
Preventing alcoholic hepatitis involves adopting healthy lifestyle choices and addressing risk factors early. Key preventive measures include:
1. Limiting Alcohol Consumption
- Adhering to recommended guidelines for safe alcohol intake can significantly reduce the risk of liver damage.
- For most adults, this means no more than one drink per day for women and two drinks per day for men.
2. Maintaining a Healthy Diet
- Eating a balanced diet rich in fruits, vegetables, whole grains, and lean proteins supports liver health.
- Avoiding processed foods and high-fat diets can also reduce the risk of fatty liver disease.
3. Regular Health Checkups
- Routine medical checkups can help detect early signs of liver damage and allow for timely intervention.
- Individuals with a history of heavy drinking should discuss their alcohol use with their healthcare provider.
4. Seeking Help for Alcohol Use Disorder
- Individuals struggling with alcohol dependence should seek professional help through counseling, support groups, or rehabilitation programs.
- Addressing alcohol use disorder is critical for preventing further liver damage.
Lifestyle Changes for Long-Term Recovery
Recovery from alcoholic hepatitis requires ongoing commitment and lifestyle changes. These adjustments can help improve liver function and overall well-being:
1. Exercise Regularly
- Engaging in regular physical activity promotes weight management and reduces the risk of fatty liver disease.
- Exercise also improves mood and reduces stress, which can aid in maintaining sobriety.
2. Avoid Harmful Substances
- Avoiding tobacco, recreational drugs, and unnecessary medications can protect the liver from further damage.
- Always consult a healthcare provider before taking new medications or supplements.
3. Build a Support Network
- Connecting with friends, family, or support groups can provide encouragement and accountability during recovery.
- Organizations like Alcoholics Anonymous offer resources and community for individuals seeking sobriety.
4. Practice Stress Management
- Stress-reducing techniques such as meditation, yoga, or deep breathing exercises can support mental and physical health.
- Managing stress is particularly important for individuals recovering from alcohol use disorder.