Addison’s Disease, also known as Adrenal Insufficiency (AI), is a rare but serious medical condition that affects the adrenal glands. These small organs, located above the kidneys, are responsible for producing essential hormones such as cortisol and aldosterone. When the adrenal glands fail to produce adequate amounts of these hormones, it can lead to a wide range of symptoms and complications. This article provides an in-depth overview of Addison’s Disease, including its causes, symptoms, diagnosis, and management strategies.
Understanding the Adrenal Glands
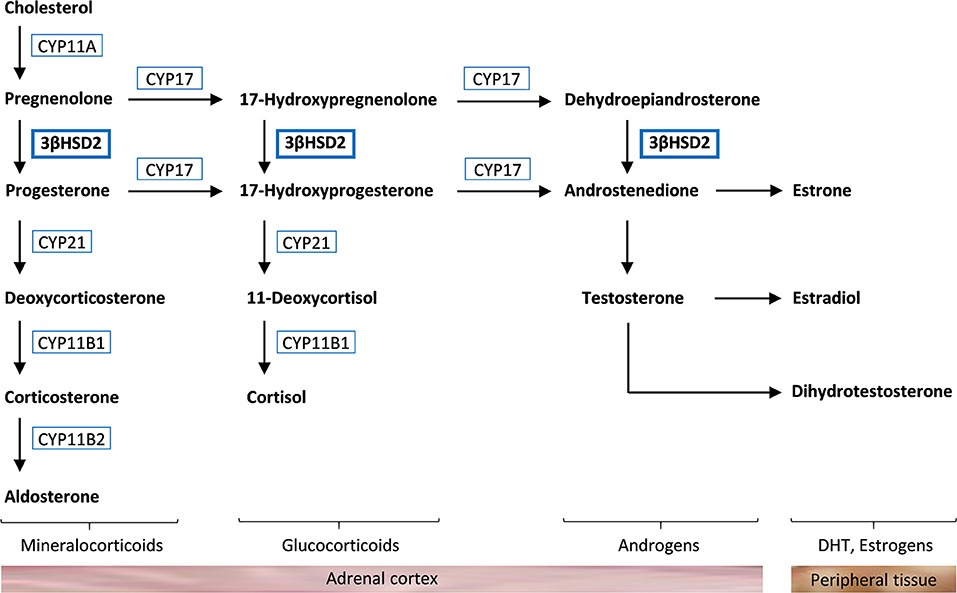
The adrenal glands play a crucial role in maintaining overall health by producing hormones that regulate various bodily functions. The two primary hormones produced by these glands are cortisol and aldosterone. Cortisol helps the body respond to stress, regulates metabolism, and controls blood sugar levels. Aldosterone, on the other hand, helps maintain blood pressure and balance sodium and potassium levels in the body.
When the adrenal glands are damaged or malfunctioning, they may not produce enough of these hormones, leading to a condition known as adrenal insufficiency. Addison’s Disease specifically refers to primary adrenal insufficiency, which occurs when the problem originates in the adrenal glands themselves.
Causes of Addison’s Disease
There are several potential causes of Addison’s Disease, with autoimmune disorders being the most common. In autoimmune Addison’s Disease, the immune system mistakenly attacks the adrenal cortex, the outer layer of the adrenal glands, impairing its ability to produce hormones. Other possible causes include:
- Infections, such as tuberculosis, which can damage the adrenal glands.
- Cancer that spreads to the adrenal glands.
- Bleeding into the adrenal glands, often due to blood-thinning medications or severe infections.
- Genetic disorders that affect the development or function of the adrenal glands.
- Surgical removal of the adrenal glands.
Symptoms of Addison’s Disease
The symptoms of Addison’s Disease often develop gradually and may be vague at first, making the condition difficult to diagnose. Common signs and symptoms include:
Physical Symptoms
- Fatigue and weakness, which may worsen over time.
- Weight loss and decreased appetite.
- Low blood pressure, leading to dizziness or fainting.
- Salt cravings due to imbalances in sodium levels.
- Muscle and joint pain.
- Nausea, vomiting, or diarrhea.
Skin Changes
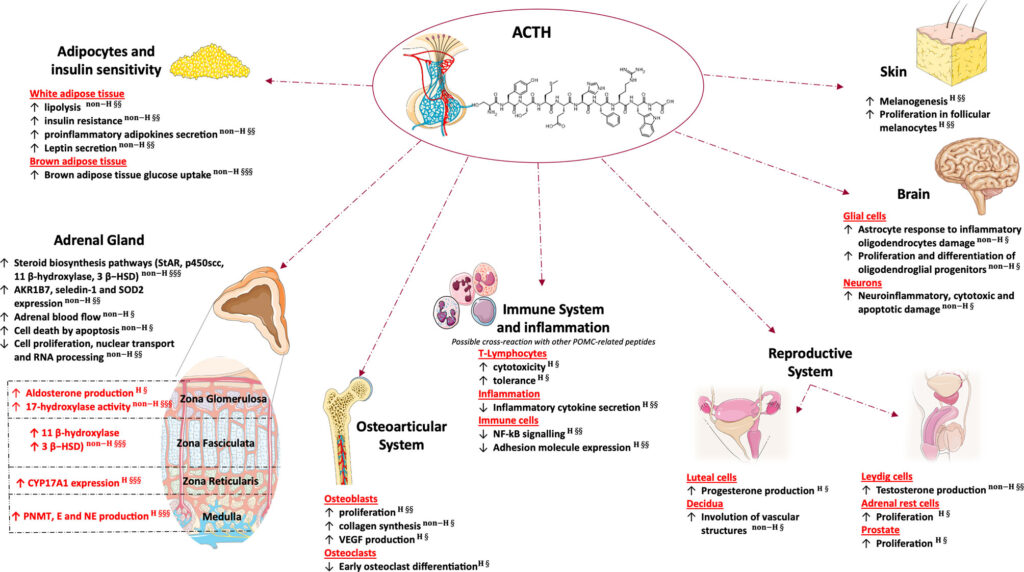
One of the hallmark features of Addison’s Disease is hyperpigmentation, or darkening of the skin. This occurs because the body produces excess adrenocorticotropic hormone (ACTH) in an attempt to stimulate the adrenal glands. ACTH also stimulates melanin production, leading to patches of darker skin, particularly in areas exposed to the sun, scars, or skin folds.
Emotional and Cognitive Symptoms
- Irritability and mood swings.
- Depression or anxiety.
- Difficulty concentrating or memory problems.
Acute Symptoms: Addisonian Crisis
In severe cases, individuals with Addison’s Disease may experience an Addisonian crisis, a life-threatening condition that requires immediate medical attention. Symptoms of an Addisonian crisis include:
- Sudden, severe pain in the lower back, abdomen, or legs.
- Extreme weakness and confusion.
- High fever and dehydration.
- Rapid heart rate and low blood pressure.
Diagnosis of Addison’s Disease
Diagnosing Addison’s Disease can be challenging due to its nonspecific symptoms. A thorough evaluation typically involves a combination of medical history, physical examination, and laboratory tests.
Blood Tests
Blood tests are used to measure hormone levels, including cortisol and aldosterone. Low levels of these hormones may indicate adrenal insufficiency. Additionally, doctors may check sodium, potassium, and glucose levels, as imbalances in these electrolytes are common in Addison’s Disease.
ACTH Stimulation Test
The ACTH stimulation test is one of the most reliable methods for diagnosing Addison’s Disease. During this test, a synthetic form of adrenocorticotropic hormone is injected into the bloodstream, and cortisol levels are measured before and after the injection. In healthy individuals, cortisol levels rise significantly. However, in people with Addison’s Disease, the response is minimal or absent.
Imaging Studies
Imaging studies, such as computed tomography (CT) scans or magnetic resonance imaging (MRI), may be performed to assess the size and structure of the adrenal glands. These tests can help identify abnormalities, such as tumors or bleeding, that may be contributing to the condition.
Treatment and Management of Addison’s Disease
While there is no cure for Addison’s Disease, it can be effectively managed with hormone replacement therapy and lifestyle adjustments. The goal of treatment is to replace the deficient hormones and prevent complications.
Hormone Replacement Therapy
The cornerstone of treatment for Addison’s Disease is hormone replacement therapy. This typically involves taking medications that mimic the effects of cortisol and aldosterone. Common treatments include:
- Hydrocortisone or prednisone to replace cortisol.
- Fludrocortisone to replace aldosterone and maintain electrolyte balance.
Patients are usually instructed to take these medications daily and adjust the dosage during times of stress, illness, or surgery to prevent an Addisonian crisis.
Dietary and Lifestyle Adjustments
In addition to medication, individuals with Addison’s Disease can benefit from certain lifestyle changes to support their overall health. These include:
- Consuming a balanced diet rich in fruits, vegetables, whole grains, and lean proteins.
- Incorporating more salt into the diet, especially during hot weather or exercise, to compensate for sodium loss.
- Staying hydrated to prevent dehydration.
- Avoiding excessive physical exertion and managing stress effectively.
Emergency Preparedness
People with Addison’s Disease should always carry an emergency injection of hydrocortisone and wear a medical alert bracelet indicating their condition. This ensures that healthcare providers can administer appropriate treatment quickly in the event of an Addisonian crisis.
Living with Addison’s Disease
Living with Addison’s Disease requires ongoing commitment to treatment and self-care. Regular follow-up appointments with an endocrinologist are essential to monitor hormone levels and adjust medications as needed. Education about the condition and recognizing early warning signs of an Addisonian crisis can empower patients to manage their health effectively.
Support Networks
Connecting with support groups and other individuals living with Addison’s Disease can provide valuable emotional support and practical advice. Sharing experiences and coping strategies can help reduce feelings of isolation and improve quality of life.
Advances in Research
Ongoing research into Addison’s Disease aims to improve diagnostic techniques and develop new treatment options. Scientists are exploring the potential of stem cell therapy and gene therapy to restore adrenal gland function, offering hope for future advancements in care.