Acute Kidney Injury, often abbreviated as AKI, is a sudden episode of kidney failure or damage that occurs within a few hours or days. This condition can be life-threatening if not promptly addressed. The kidneys play a crucial role in filtering waste products, balancing fluids, and maintaining electrolyte levels in the body. When they are impaired, it can lead to severe complications. In this article, we will explore the causes, symptoms, diagnosis, and treatment options for Acute Kidney Injury.
What Causes Acute Kidney Injury?
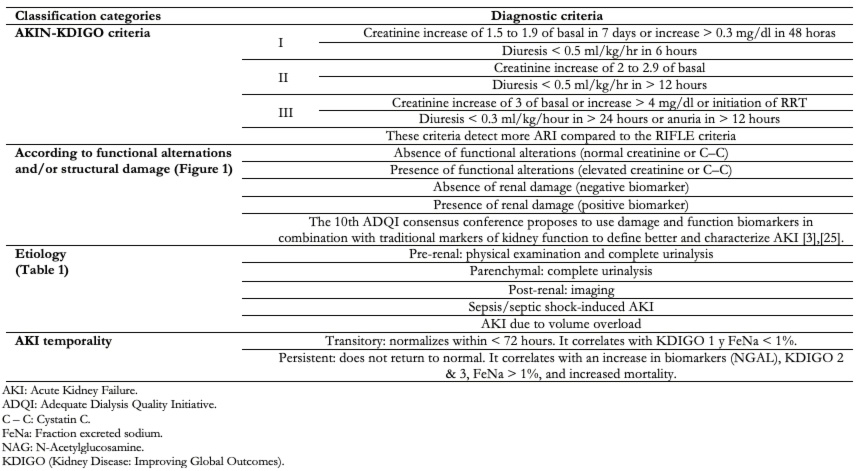
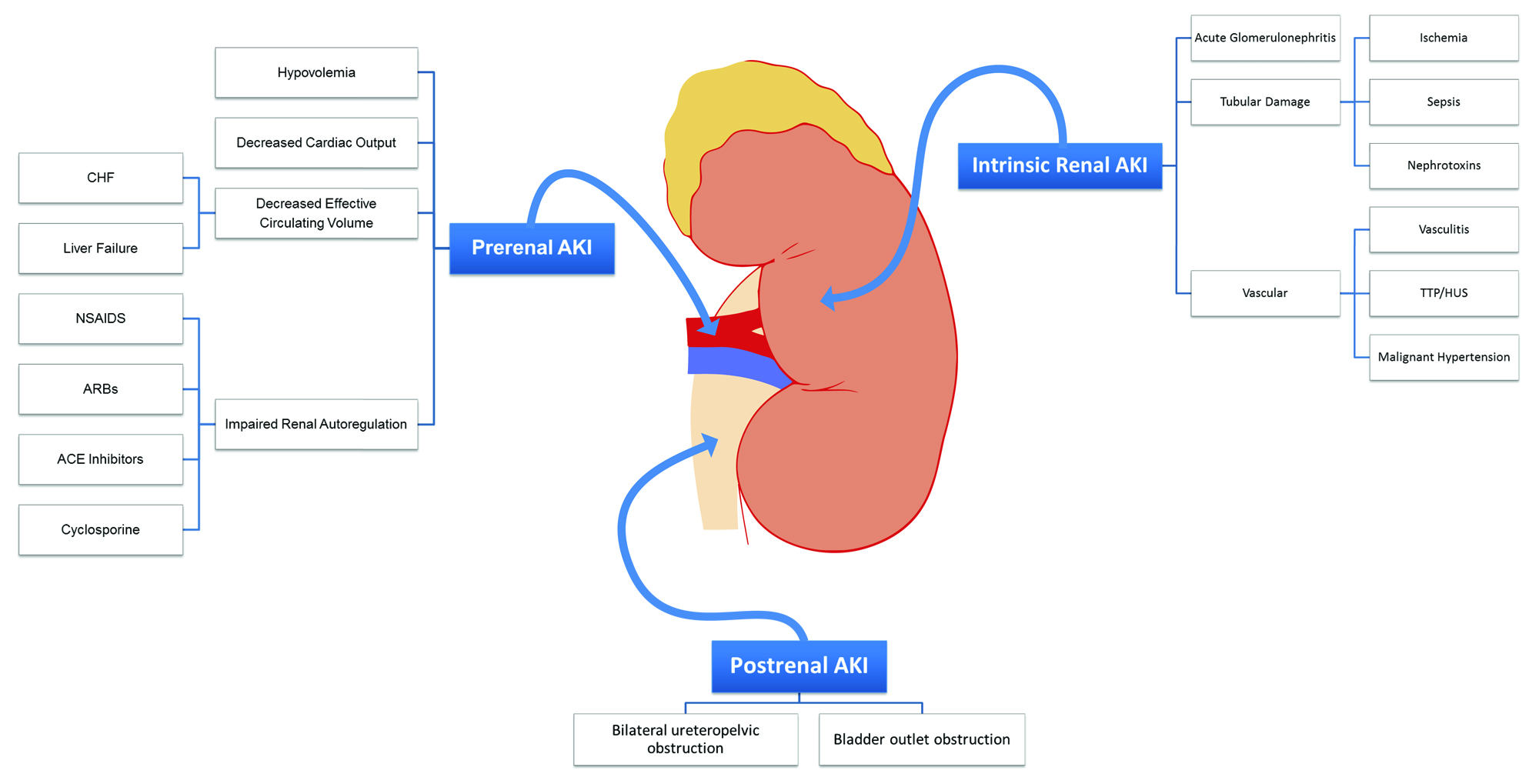
The causes of Acute Kidney Injury can be broadly categorized into three groups: pre-renal, intrinsic renal, and post-renal causes. Understanding these categories helps healthcare providers identify the underlying issue and initiate appropriate treatment.
Pre-Renal Causes
Pre-renal causes refer to conditions that reduce blood flow to the kidneys. These include:
- Dehydration: Severe dehydration due to excessive sweating, vomiting, diarrhea, or insufficient fluid intake can impair kidney function.
- Blood Loss: Significant blood loss from trauma, surgery, or internal bleeding reduces the amount of blood reaching the kidneys.
- Heart Failure: Heart conditions that impair the heart’s ability to pump blood effectively can lead to reduced kidney perfusion.
- Low Blood Pressure: Conditions like septic shock or severe infections can cause dangerously low blood pressure, affecting kidney function.
Intrinsic Renal Causes
Intrinsic renal causes involve direct damage to the kidneys themselves. Some common examples include:
- Acute Tubular Necrosis: This is one of the most common forms of intrinsic kidney injury, often caused by toxins, medications, or prolonged low blood flow to the kidneys.
- Glomerulonephritis: Inflammation of the kidney’s filtering units can result from infections, autoimmune diseases, or other systemic conditions.
- Interstitial Nephritis: This condition involves inflammation of the kidney tissue surrounding the tubules, often triggered by allergic reactions to medications.
- Vascular Diseases: Conditions like blood clots or cholesterol emboli can block blood vessels in the kidneys, leading to damage.
Post-Renal Causes
Post-renal causes occur when there is an obstruction preventing urine from leaving the kidneys. Common examples include:
- Kidney Stones: Large stones can block the urinary tract, causing a buildup of pressure and damage to the kidneys.
- Tumors: Growths in the urinary tract or bladder can obstruct urine flow.
- Enlarged Prostate: In men, an enlarged prostate gland can compress the urethra, leading to urine retention and kidney damage.
- Nerve Damage: Conditions affecting the nerves that control bladder function can lead to urine retention and subsequent kidney injury.
Symptoms of Acute Kidney Injury
The symptoms of Acute Kidney Injury can vary depending on the severity of the condition and the underlying cause. In some cases, the symptoms may be subtle, while in others, they can be more pronounced. Common signs and symptoms include:
Changes in Urination
- Decreased Urine Output: One of the hallmark signs of Acute Kidney Injury is a significant reduction in urine production.
- Blood in Urine: Hematuria, or the presence of blood in the urine, can indicate kidney damage.
- Foamy Urine: Excessive protein in the urine, known as proteinuria, can cause urine to appear foamy.
Swelling and Fluid Retention
- Swollen Legs, Ankles, or Feet: Fluid buildup due to impaired kidney function can lead to noticeable swelling in the lower extremities.
- Puffiness Around the Eyes: Swelling around the eyes can also occur as a result of fluid retention.
Systemic Symptoms
- Fatigue: Feeling unusually tired or weak is a common symptom of Acute Kidney Injury.
- Nausea and Vomiting: Accumulation of waste products in the blood can cause gastrointestinal symptoms.
- Shortness of Breath: Fluid overload or metabolic imbalances can lead to difficulty breathing.
- Chest Pain: In severe cases, chest pain may occur due to inflammation around the heart or fluid accumulation in the lungs.
How is Acute Kidney Injury Diagnosed?
Diagnosing Acute Kidney Injury involves a combination of clinical evaluation, laboratory tests, and imaging studies. Early detection is critical to prevent further kidney damage and complications.
Clinical Evaluation
A thorough medical history and physical examination are essential components of the diagnostic process. Healthcare providers will assess risk factors, such as recent illnesses, medication use, and pre-existing conditions. They will also look for signs of fluid overload, such as swelling or high blood pressure.
Laboratory Tests
Several laboratory tests are used to evaluate kidney function and identify potential causes of Acute Kidney Injury:
- Blood Tests: Measuring serum creatinine and blood urea nitrogen levels helps assess how well the kidneys are filtering waste products.
- Urine Tests: Analyzing urine for abnormalities, such as protein, blood, or specific markers of kidney damage, provides valuable diagnostic information.
- Electrolyte Panels: Imbalances in electrolytes like potassium, sodium, and calcium can indicate kidney dysfunction.
Imaging Studies
Imaging techniques are often used to visualize the kidneys and urinary tract:
- Ultrasound: This non-invasive test uses sound waves to create images of the kidneys and detect obstructions or structural abnormalities.
- CT Scan: A computed tomography scan provides detailed images of the kidneys and can help identify tumors, stones, or other issues.
- MRI: Magnetic resonance imaging may be used in certain cases to obtain detailed images of the kidneys and surrounding structures.
Kidney Biopsy
In some cases, a kidney biopsy may be necessary to determine the exact cause of Acute Kidney Injury. During this procedure, a small sample of kidney tissue is removed and examined under a microscope.
Treatment Options for Acute Kidney Injury
The treatment of Acute Kidney Injury depends on the underlying cause and the severity of the condition. The primary goals of treatment are to address the root cause, support kidney function, and prevent complications.
Treating Underlying Causes
Identifying and addressing the underlying cause is a critical step in managing Acute Kidney Injury:
- Restoring Blood Flow: For pre-renal causes, treatments focus on improving blood flow to the kidneys. This may involve intravenous fluids, medications to raise blood pressure, or interventions to stop bleeding.
- Removing Obstructions: For post-renal causes, procedures like removing kidney stones, draining fluid collections, or relieving urinary tract obstructions are essential.
- Discontinuing Harmful Medications: If medications are contributing to kidney damage, they may need to be stopped or adjusted.
Supportive Care
Supportive care measures aim to stabilize the patient and manage complications:
- Fluid Management: Careful monitoring and adjustment of fluid intake are crucial to prevent fluid overload or dehydration.
- Electrolyte Balance: Correcting imbalances in electrolytes, particularly potassium and sodium, is vital to avoid complications like arrhythmias.
- Dialysis: In severe cases where the kidneys are unable to filter waste products adequately, dialysis may be required. This procedure removes excess fluids, toxins, and waste products from the blood.
Medications
Various medications may be prescribed to manage symptoms and complications:
- Diuretics: These medications help increase urine output and reduce fluid retention.
- Antibiotics: If an infection is contributing to kidney injury, antibiotics may be necessary to treat the underlying infection.
- Medications for High Blood Pressure: Controlling blood pressure is important to protect the kidneys and prevent further damage.
Lifestyle Modifications
In addition to medical treatments, lifestyle changes can support recovery and reduce the risk of recurrence:
- Dietary Adjustments: A diet low in sodium, potassium, and phosphorus may be recommended to reduce the workload on the kidneys.
- Hydration: Maintaining adequate hydration is essential, but fluid intake should be carefully monitored to avoid overhydration.
- Regular Monitoring: Follow-up appointments with healthcare providers are necessary to monitor kidney function and adjust treatment as needed.