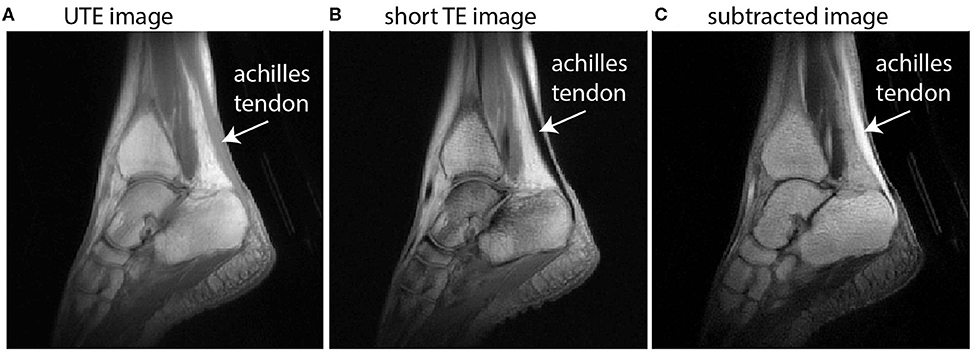
Achilles tendinitis, often abbreviated as AT, is a common condition that affects the Achilles tendon, the large band of tissue connecting the calf muscles to the heel bone. This condition typically results in pain, swelling, and limited mobility, making it a significant concern for athletes and individuals who engage in physical activities. In this article, we will explore the causes, symptoms, diagnosis, and treatment options available for this condition.
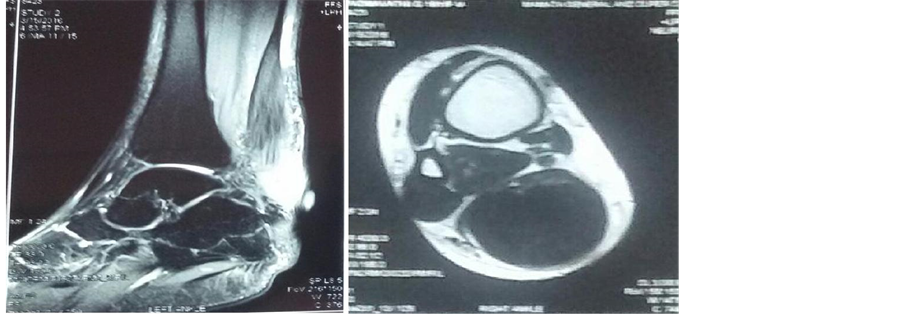
What is Achilles Tendinitis?
The Achilles tendon is one of the strongest and largest tendons in the human body. It plays a crucial role in walking, running, and jumping by allowing the foot to push off the ground. When this tendon becomes inflamed or irritated, the condition is known as Achilles tendinitis. This inflammation can occur due to overuse, injury, or other underlying factors.
Types of Achilles Tendinitis
- Noninsertional Achilles Tendinitis: This type occurs when fibers in the middle portion of the tendon begin to break down, swell, and thicken. It is more common in younger, active individuals.
- Insertional Achilles Tendinitis: This form affects the lower portion of the tendon where it attaches to the heel bone. It can occur in anyone, regardless of activity level, and is often associated with bone spurs.
Causes of Achilles Tendinitis
Several factors can contribute to the development of Achilles tendinitis. Understanding these causes can help individuals take preventive measures and reduce their risk of developing the condition.
Overuse and Repetitive Stress
One of the most common causes of Achilles tendinitis is overuse. Activities such as running, jumping, or sudden increases in physical intensity can place excessive stress on the tendon. Over time, this repetitive strain can lead to inflammation and microtears in the tendon fibers.
Inadequate Footwear
Wearing improper or worn-out shoes can increase the risk of developing Achilles tendinitis. Shoes that lack proper arch support or cushioning fail to absorb shock effectively, placing additional strain on the tendon.
Poor Training Techniques
Engaging in improper training practices, such as running on uneven surfaces or failing to warm up adequately, can also contribute to the condition. Sudden changes in exercise routines, such as increasing distance or intensity too quickly, are particularly problematic.
Underlying Medical Conditions
Certain medical conditions, such as arthritis or diabetes, can weaken the tendon and make it more susceptible to injury. Additionally, individuals with flat feet may experience extra strain on the Achilles tendon due to altered foot mechanics.
Age and Gender Factors
As people age, tendons naturally lose elasticity and become more prone to injury. Middle-aged individuals are at a higher risk of developing Achilles tendinitis compared to younger adults. Men are also more likely to experience this condition than women.
Symptoms of Achilles Tendinitis
Recognizing the symptoms of Achilles tendinitis is essential for early diagnosis and treatment. The following signs may indicate the presence of this condition:
Pain Along the Tendon
Individuals with Achilles tendinitis often experience pain along the back of the leg, near the heel. This pain may develop gradually and worsen with activity. In some cases, the pain may be mild initially but intensify over time.
Stiffness and Swelling
Morning stiffness is a common symptom, with individuals noticing tightness in the tendon upon waking. Swelling around the affected area may also occur, particularly after physical activity.
Tenderness to Touch
The Achilles tendon may feel tender when pressed or touched. This tenderness is often accompanied by warmth and redness in the surrounding area.
Limited Range of Motion
As the condition progresses, individuals may find it difficult to flex their foot or point their toes downward. This limitation in range of motion can interfere with daily activities and athletic performance.
Diagnosis of Achilles Tendinitis
Accurate diagnosis is crucial for effective treatment. Healthcare providers use a combination of physical examinations and diagnostic tests to confirm the presence of Achilles tendinitis.
Physical Examination
During a physical examination, a healthcare provider will assess the affected area for signs of swelling, tenderness, and pain. They may also evaluate the individual’s gait and range of motion to identify any abnormalities.
Imaging Tests
In some cases, imaging tests may be necessary to rule out other conditions or assess the severity of the injury. Common imaging techniques include:
- X-rays: While X-rays do not show soft tissues like tendons, they can help identify bone spurs or other structural issues.
- Magnetic Resonance Imaging (MRI): MRI scans provide detailed images of the tendon and surrounding tissues, helping to detect tears or degeneration.
- Ultrasound: This non-invasive test uses sound waves to create images of the tendon, allowing healthcare providers to assess its thickness and integrity.
Treatment Options for Achilles Tendinitis
Treatment for Achilles tendinitis focuses on reducing pain, promoting healing, and preventing recurrence. The specific approach depends on the severity of the condition and the individual’s lifestyle.
Rest and Activity Modification
One of the first steps in treating Achilles tendinitis is to rest the affected tendon. Avoiding activities that exacerbate the pain allows the tendon to heal. Individuals may need to modify their exercise routines or switch to low-impact activities such as swimming or cycling.
Ice Therapy
Applying ice packs to the affected area can help reduce swelling and alleviate pain. Ice therapy is most effective when applied for 15 to 20 minutes at a time, several times a day.
Stretching and Strengthening Exercises
Gentle stretching exercises can improve flexibility and reduce tension in the tendon. Physical therapists often recommend eccentric strengthening exercises, which involve lengthening the tendon under load, to promote healing and prevent future injuries.
Orthotic Devices and Proper Footwear
Using orthotic devices, such as heel lifts or arch supports, can help reduce strain on the Achilles tendon. Wearing supportive footwear designed for specific activities is also essential for long-term recovery.
Medications
Over-the-counter pain relievers, such as ibuprofen or naproxen, can help manage pain and inflammation. However, these medications should be used under the guidance of a healthcare provider to avoid potential side effects.
Physical Therapy
A structured physical therapy program can address muscle imbalances, improve biomechanics, and enhance overall function. Therapists may use techniques such as massage, ultrasound therapy, or dry needling to accelerate recovery.
Corticosteroid Injections
In severe cases, healthcare providers may recommend corticosteroid injections to reduce inflammation. However, these injections carry risks, such as tendon weakening, and are typically used as a last resort.
Surgical Intervention
If conservative treatments fail to provide relief, surgery may be considered. Surgical options include removing damaged tissue, repairing tears, or addressing bone spurs. Surgery is generally reserved for chronic or severe cases of Achilles tendinitis.
Preventing Achilles Tendinitis
Taking proactive steps can significantly reduce the risk of developing Achilles tendinitis. These preventive measures include:
- Gradually increasing the intensity and duration of physical activities.
- Warming up properly before exercise and cooling down afterward.
- Wearing appropriate footwear with adequate support and cushioning.
- Incorporating strength and flexibility exercises into regular routines.
- Avoiding activities that place excessive stress on the tendon.
By understanding the causes, symptoms, and treatment options for Achilles tendinitis, individuals can take control of their health and minimize the impact of this condition on their daily lives.