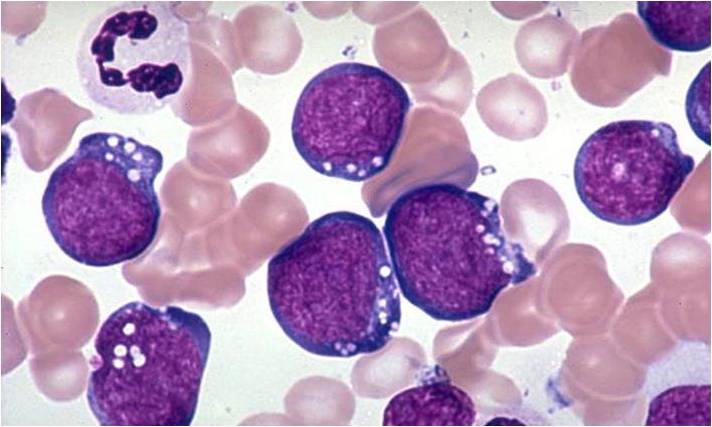
Acute Lymphoblastic Leukemia, commonly abbreviated as ALL, is a type of cancer that primarily affects the blood and bone marrow. This condition occurs when the body produces an excessive number of immature white blood cells, known as lymphoblasts or leukemic blasts. These abnormal cells crowd out healthy blood cells, leading to a variety of complications. In this article, we will explore the nature of this disease, its symptoms, diagnostic methods, and approaches to care.
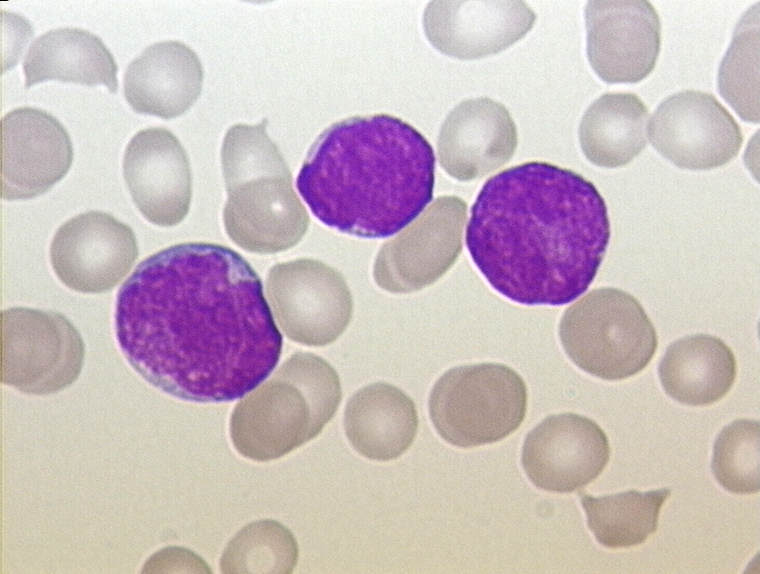
Understanding Acute Lymphoblastic Leukemia
Acute Lymphoblastic Leukemia is a fast-growing form of cancer that begins in the bone marrow, the soft tissue inside bones where blood cells are produced. It specifically targets lymphocytes, which are a type of white blood cell responsible for fighting infections. When someone develops this condition, their bone marrow produces too many immature lymphocytes, leaving little room for the production of healthy red blood cells, white blood cells, and platelets.
This type of leukemia is most commonly diagnosed in children but can also occur in adults. While it is one of the more treatable forms of cancer in children, the prognosis in adults tends to be less favorable. Understanding the underlying causes and risk factors is essential for early detection and treatment.
Potential Causes and Risk Factors
The exact cause of Acute Lymphoblastic Leukemia remains unknown, but researchers have identified several factors that may increase the risk of developing the condition:
- Genetic Mutations: Changes in certain genes can lead to the uncontrolled growth of abnormal white blood cells.
- Exposure to Radiation: High levels of radiation exposure, such as from nuclear accidents or radiation therapy for other cancers, may elevate the risk.
- Chemical Exposure: Certain chemicals, including benzene, have been linked to an increased likelihood of developing this disease.
- Previous Cancer Treatments: Chemotherapy or radiation therapy for other types of cancer may predispose individuals to develop this condition later in life.
- Genetic Disorders: Conditions like Down syndrome or certain inherited syndromes can raise the risk of developing this type of leukemia.
Symptoms of Acute Lymphoblastic Leukemia
The symptoms of this condition often appear suddenly and worsen quickly due to the rapid progression of the disease. These symptoms are typically caused by the overproduction of abnormal white blood cells and the suppression of healthy blood cells. Some common signs include:
Fatigue and Weakness
One of the earliest and most noticeable symptoms is fatigue. This occurs because the bone marrow is producing fewer red blood cells, leading to anemia. Anemia reduces the amount of oxygen carried to tissues, resulting in persistent tiredness and weakness.
Frequent Infections
Since the abnormal white blood cells produced in this condition cannot fight infections effectively, individuals may experience frequent or severe infections. Common sites of infection include the respiratory system, urinary tract, and skin.
Bruising and Bleeding
A decrease in platelet count can lead to easy bruising, bleeding gums, nosebleeds, or prolonged bleeding from minor cuts. Platelets are essential for blood clotting, and their deficiency makes it difficult for the body to stop bleeding.
Bone and Joint Pain
Many patients report pain in their bones or joints, particularly in the arms, legs, and back. This discomfort arises because the bone marrow becomes overcrowded with abnormal cells, causing pressure and inflammation.
Swollen Lymph Nodes
Lymph nodes in the neck, armpits, or groin may become swollen and tender. This swelling occurs because the abnormal white blood cells accumulate in the lymphatic system, causing the lymph nodes to enlarge.
Other Symptoms
Additional symptoms may include fever, night sweats, loss of appetite, weight loss, and difficulty breathing. In some cases, patients may develop a pale complexion due to anemia or small red spots on the skin called petechiae, which result from bleeding under the skin.
Diagnosing Acute Lymphoblastic Leukemia
Early and accurate diagnosis is crucial for effective treatment. If a doctor suspects this condition based on symptoms and medical history, they will order a series of tests to confirm the diagnosis and determine the extent of the disease.
Blood Tests
A complete blood count is usually the first step in diagnosing this condition. Blood tests can reveal abnormalities such as a high number of white blood cells, low red blood cell count, and low platelet count. Additionally, a peripheral blood smear may show the presence of immature white blood cells in the bloodstream.
Bone Marrow Biopsy
To confirm the diagnosis, a sample of bone marrow is extracted, typically from the hip bone, and examined under a microscope. This procedure, known as a bone marrow biopsy, allows doctors to identify the presence of abnormal cells and classify the specific type of leukemia.
Imaging Tests
Imaging tests such as X-rays, CT scans, or MRIs may be performed to check for enlarged lymph nodes, liver, or spleen. These tests help assess the spread of the disease and guide treatment decisions.
Spinal Tap
In some cases, a lumbar puncture, also known as a spinal tap, is performed to check for the presence of abnormal cells in the cerebrospinal fluid. This test is particularly important because this condition can sometimes spread to the central nervous system.
Genetic Testing
Advanced genetic testing may be conducted to identify specific mutations or chromosomal abnormalities associated with the disease. This information helps doctors tailor treatment plans and predict outcomes more accurately.
Treatment Options for Acute Lymphoblastic Leukemia
Treatment for this condition typically involves a combination of therapies aimed at destroying abnormal cells and restoring normal blood cell production. The choice of treatment depends on various factors, including the patient’s age, overall health, and the specific characteristics of the disease.
Chemotherapy
Chemotherapy is the primary treatment for this condition. It involves the use of powerful drugs to kill rapidly dividing cells, including cancerous ones. Chemotherapy is usually administered in phases:
- Induction Therapy: The goal is to achieve remission by eliminating as many abnormal cells as possible.
- Consolidation Therapy: Also known as intensification, this phase aims to destroy any remaining cancer cells.
- Maintenance Therapy: Lower doses of chemotherapy are given over an extended period to prevent the disease from returning.
Radiation Therapy
Radiation therapy uses high-energy beams to target and destroy cancer cells. It is often used to treat areas of the body where the disease has spread, such as the brain or spinal cord. Radiation may also be used before a bone marrow transplant to prepare the body for the procedure.
Bone Marrow Transplant
Also known as a stem cell transplant, this procedure involves replacing damaged bone marrow with healthy cells from a donor. Before the transplant, high-dose chemotherapy or radiation is used to destroy the existing bone marrow. The transplanted cells then grow and produce new, healthy blood cells.
Targeted Therapy
Targeted therapy involves drugs that specifically attack cancer cells without harming normal cells. This approach is often used for patients with certain genetic mutations that make their cancer cells vulnerable to these medications.
Immunotherapy
Immunotherapy harnesses the power of the immune system to fight cancer. One example is CAR T-cell therapy, where a patient’s own immune cells are modified in a lab to recognize and attack cancer cells.
Supportive Care
In addition to treating the disease itself, supportive care is essential to manage symptoms and side effects. This may include blood transfusions to address anemia, antibiotics to treat infections, and medications to relieve pain or nausea.
Living with Acute Lymphoblastic Leukemia
Managing this condition requires not only medical treatment but also emotional and psychological support. Patients and their families often face significant challenges, including frequent hospital visits, financial burdens, and emotional stress. Support groups, counseling, and educational resources can provide valuable assistance during this difficult time.
Diet and lifestyle modifications may also play a role in improving quality of life. A balanced diet rich in nutrients, regular exercise (as tolerated), and adequate rest can help boost energy levels and support overall well-being.
Regular follow-up appointments with healthcare providers are critical to monitor the disease and detect any signs of relapse early. Advances in research and treatment continue to improve outcomes, offering hope to patients and their loved ones.