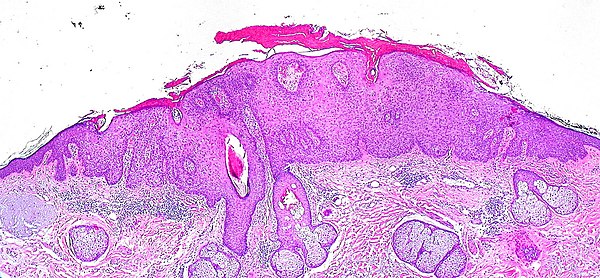
Actinic Keratosis, often abbreviated as AK, refers to rough, scaly patches on the skin that develop due to prolonged exposure to ultraviolet radiation. These patches are considered precancerous because they have the potential to progress into a type of skin cancer known as squamous cell carcinoma if left untreated. Understanding this condition is crucial for early detection and effective management. This article provides an in-depth overview of actinic keratosis, its causes, risk factors, symptoms, and available treatment options.
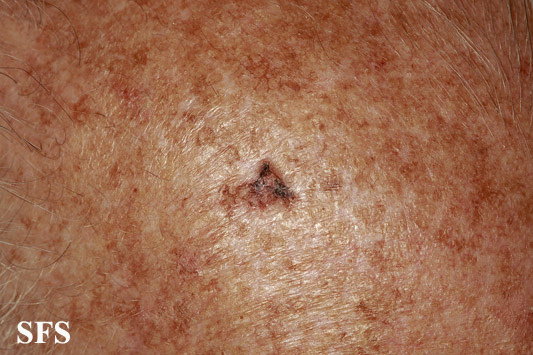
What is Actinic Keratosis?
Actinic keratosis is a common skin condition that primarily affects individuals with fair skin who have spent significant time exposed to the sun or artificial sources of ultraviolet light, such as tanning beds. The patches typically appear on areas of the body that receive frequent sun exposure, including the face, ears, scalp, neck, arms, and hands. While these patches may seem harmless at first, they are a warning sign that the skin has sustained damage at a cellular level.
The appearance of actinic keratosis can vary. Some patches may feel like sandpaper when touched, while others might be slightly raised, crusty, or discolored. The color of the patches can range from pink or red to brown or flesh-toned. Because the patches are often small and may blend with surrounding skin, they can sometimes go unnoticed without careful inspection.
Why Actinic Keratosis is Considered Precancerous
Actinic keratosis is classified as precancerous because the damaged skin cells in these patches have the potential to mutate further and develop into squamous cell carcinoma. Squamous cell carcinoma is one of the most common forms of skin cancer, and while it is usually treatable when caught early, it can become invasive and spread to other parts of the body if ignored. Therefore, addressing actinic keratosis promptly is essential to prevent more serious health complications.
Causes of Actinic Keratosis
The primary cause of actinic keratosis is cumulative exposure to ultraviolet radiation. This radiation damages the DNA within skin cells, leading to abnormal growth patterns. Over time, repeated exposure weakens the skin’s ability to repair itself, resulting in the formation of rough, scaly patches.
Sun Exposure
Ultraviolet radiation from the sun is the leading cause of actinic keratosis. Individuals who spend extended periods outdoors without adequate sun protection are at the highest risk. Activities such as gardening, hiking, or working in construction can increase exposure to harmful UV rays. Even short bursts of intense sun exposure, such as sunburns during childhood, can contribute to the development of actinic keratosis later in life.
Artificial UV Sources
In addition to natural sunlight, artificial sources of ultraviolet radiation, such as tanning beds, can also lead to actinic keratosis. Tanning beds emit concentrated levels of UV radiation, which penetrate deeply into the skin and accelerate cellular damage. Studies have shown that individuals who use tanning beds regularly are at a significantly higher risk of developing precancerous skin conditions, including actinic keratosis.
Other Contributing Factors
- Fair Skin: People with lighter skin tones are more susceptible to actinic keratosis because their skin contains less melanin, the pigment that provides some protection against UV radiation.
- Age: The risk of developing actinic keratosis increases with age, as cumulative sun exposure builds over time. Most cases occur in individuals over the age of 40.
- Geographic Location: Living in regions with high levels of sunlight, such as areas closer to the equator, raises the likelihood of developing actinic keratosis.
- Weakened Immune System: Conditions or treatments that suppress the immune system, such as organ transplants or chemotherapy, can make individuals more vulnerable to actinic keratosis.
Symptoms of Actinic Keratosis
Recognizing the signs of actinic keratosis is critical for early intervention. While the condition is not painful in most cases, it can cause discomfort or irritation, especially when the patches are located in areas subject to friction, such as the scalp or hands.
Common Signs and Characteristics
- Rough Texture: The patches often feel dry, rough, or gritty to the touch, resembling sandpaper.
- Color Variations: Actinic keratosis patches may appear pink, red, brown, or flesh-colored. In some cases, they may have a combination of colors.
- Size and Shape: The patches are typically small, ranging from a few millimeters to about an inch in diameter. They may be flat or slightly raised and can develop a hard, crusty surface over time.
- Itching or Burning: Some individuals experience mild itching or a burning sensation in the affected areas.
When to Seek Medical Attention
If you notice any unusual changes in your skin, such as persistent rough patches, discoloration, or sores that do not heal, it is important to consult a dermatologist. Early diagnosis and treatment can prevent the progression of actinic keratosis into more serious conditions.
Treatment Options for Actinic Keratosis
There are several treatment options available for managing actinic keratosis. The choice of treatment depends on factors such as the number of patches, their location, and the patient’s overall health. A dermatologist will evaluate the condition and recommend the most appropriate course of action.
Topical Medications
Topical treatments are often prescribed for mild to moderate cases of actinic keratosis. These medications are applied directly to the affected areas and work by targeting and destroying abnormal skin cells.
- 5-Fluorouracil Cream: This medication inhibits the growth of abnormal cells and is commonly used to treat multiple patches of actinic keratosis.
- Imiquimod Cream: Imiquimod stimulates the immune system to attack abnormal cells, promoting healing and reducing the risk of recurrence.
- Diclofenac Gel: This nonsteroidal anti-inflammatory drug helps reduce inflammation and slow the growth of precancerous cells.
Cryotherapy
Cryotherapy involves freezing the affected skin with liquid nitrogen to destroy abnormal cells. This procedure is quick and effective for treating isolated patches of actinic keratosis. After treatment, the treated area may blister and peel before healing with new, healthy skin.
Photodynamic Therapy
Photodynamic therapy combines a photosensitizing agent with a special light source to target and destroy precancerous cells. During the procedure, a topical solution is applied to the skin, making it sensitive to light. The area is then exposed to a specific wavelength of light, which activates the solution and destroys abnormal cells.
Laser Therapy
Laser therapy uses concentrated beams of light to remove damaged skin layers. This treatment is particularly effective for actinic keratosis on the face or other delicate areas. Laser therapy promotes the growth of new, healthy skin while minimizing scarring.
Surgical Removal
In cases where actinic keratosis has progressed or there is concern about potential malignancy, surgical removal may be necessary. Techniques such as curettage and electrodessication involve scraping away the affected tissue and using an electric current to seal the wound. Excisional surgery may also be performed to remove larger or more suspicious lesions.
Lifestyle Modifications and Prevention
While treatment is essential for existing patches, preventing new occurrences of actinic keratosis is equally important. Simple lifestyle changes can significantly reduce the risk of developing this condition.
- Sun Protection: Wearing protective clothing, such as wide-brimmed hats and long sleeves, and using broad-spectrum sunscreen with an SPF of 30 or higher can help shield the skin from harmful UV rays.
- Avoiding Tanning Beds: Eliminating the use of tanning beds is crucial for minimizing UV exposure and protecting the skin.
- Regular Skin Checks: Performing self-examinations and scheduling routine visits with a dermatologist can aid in the early detection of actinic keratosis and other skin abnormalities.
Conclusion
Actinic keratosis is a common yet serious skin condition that requires attention and care. By understanding its causes, recognizing its symptoms, and exploring available treatment options, individuals can take proactive steps to protect their skin and overall health.