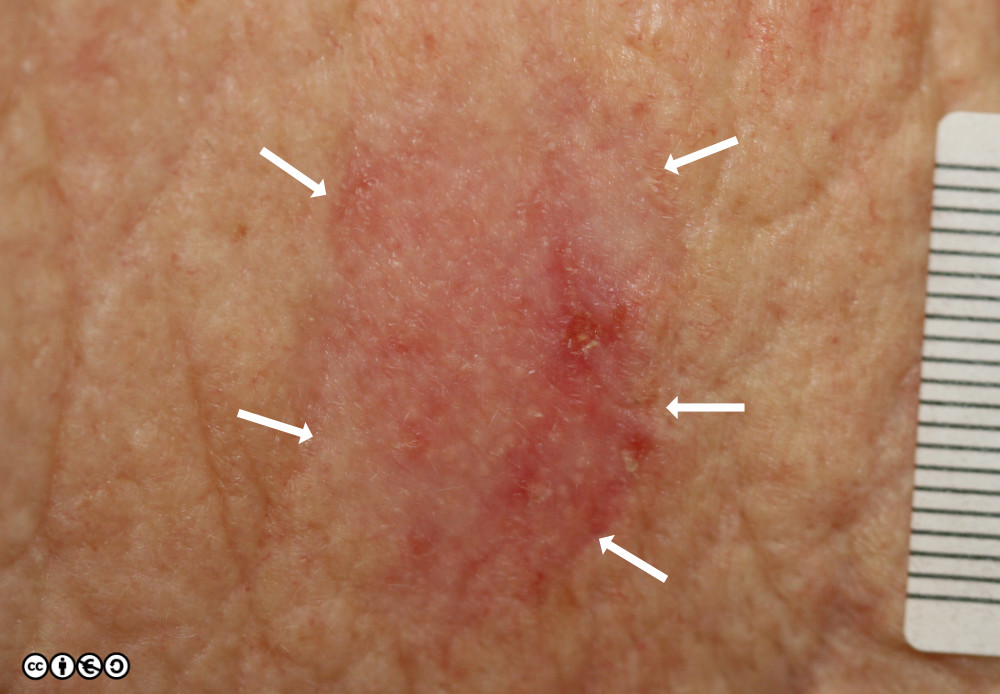
Basal cell carcinoma, commonly abbreviated as BCC, is one of the most frequently diagnosed types of skin cancer. It originates in the basal cells, which are located in the deepest layer of the epidermis, the outermost layer of the skin. While it is generally slow-growing and rarely spreads to other parts of the body, untreated cases can lead to significant damage to surrounding tissues and structures. This article provides an in-depth overview of basal cell skin cancer, including its symptoms, causes, risk factors, and available treatments.
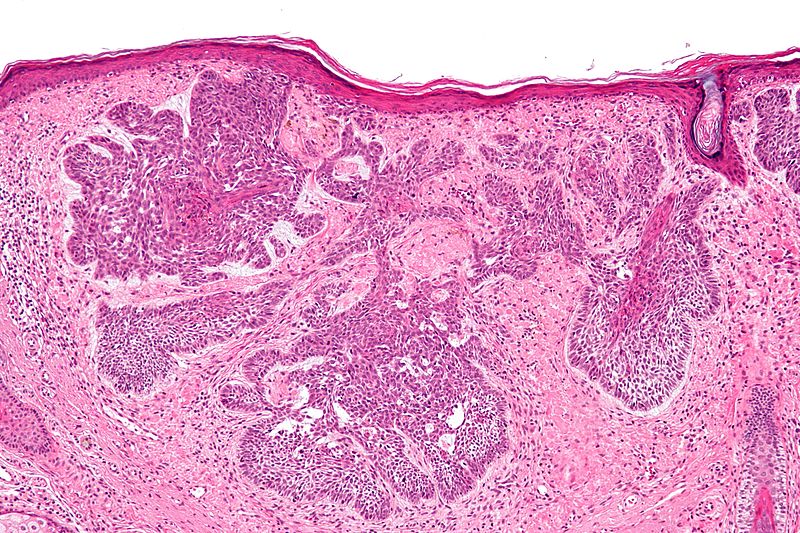
Understanding Basal Cell Carcinoma
Basal cell carcinoma develops when the DNA of basal cells is damaged, leading to uncontrolled growth. These cells are responsible for producing new skin cells as old ones die off. When this process is disrupted, abnormal cells accumulate and form a tumor. Basal cell carcinoma typically appears on areas of the skin that are frequently exposed to sunlight, such as the face, ears, neck, scalp, shoulders, and back.
Although basal cell carcinoma is highly treatable, especially when detected early, it is essential to understand its characteristics to prevent complications. Unlike other forms of skin cancer, such as melanoma, basal cell carcinoma rarely metastasizes, meaning it seldom spreads to distant organs. However, it can invade nearby tissues, causing disfigurement if left untreated.
Symptoms of Basal Cell Carcinoma
The signs and symptoms of basal cell carcinoma can vary depending on the type and location of the lesion. Some of the most common manifestations include:
- Pearly or Waxy Bumps: These are often flesh-colored or pinkish and may have visible blood vessels. They are commonly found on the face, ears, or neck.
- Flat, Scaly Patches: These lesions may appear brown or reddish and are more common on the back or chest.
- Bleeding or Crusting Sores: A sore that repeatedly bleeds, crusts over, and then reopens without fully healing could be a sign of basal cell carcinoma.
- White, Waxy Scar-Like Areas: Known as morpheaform basal cell carcinoma, this rare subtype can resemble a scar and may go unnoticed until it grows larger.
- Pigmented Lesions: Some basal cell carcinomas may appear dark brown, blue, or black, resembling melanoma.
It is important to note that basal cell carcinoma can sometimes mimic other skin conditions, such as eczema or psoriasis. Therefore, any unusual changes in the skin should be evaluated by a healthcare professional.
Causes of Basal Cell Carcinoma
The primary cause of basal cell carcinoma is damage to the DNA of basal cells, which disrupts their normal growth and division. Several factors contribute to this damage, with ultraviolet radiation being the most significant.
Ultraviolet Radiation
Exposure to ultraviolet radiation from the sun or artificial sources like tanning beds is the leading cause of basal cell carcinoma. UV radiation penetrates the skin and damages the DNA in basal cells, leading to mutations that result in uncontrolled cell growth. People who spend extended periods outdoors or live in sunny climates are at higher risk.
Fair Skin
Individuals with fair skin have less melanin, the pigment that provides some protection against UV radiation. As a result, they are more susceptible to DNA damage and have a higher risk of developing basal cell carcinoma.
Age
Basal cell carcinoma is more common in older adults, as cumulative sun exposure over time increases the likelihood of DNA damage. However, younger individuals can also develop this condition, especially if they have a history of excessive sun exposure or use tanning beds.
Genetic Factors
Certain genetic conditions, such as Gorlin syndrome, increase the risk of developing multiple basal cell carcinomas. Gorlin syndrome is a rare inherited disorder that affects the development of bones and skin, predisposing individuals to this type of cancer.
Weakened Immune System
People with weakened immune systems, such as those undergoing organ transplants or living with HIV, are at a higher risk of developing basal cell carcinoma. A compromised immune system may struggle to repair DNA damage or eliminate abnormal cells effectively.
Risk Factors for Basal Cell Carcinoma
In addition to the causes mentioned above, several risk factors can increase the likelihood of developing basal cell carcinoma:
- History of Sunburns: Severe sunburns, especially during childhood, can significantly raise the risk of basal cell carcinoma later in life.
- Outdoor Occupations: Individuals who work outdoors, such as construction workers or farmers, are exposed to higher levels of UV radiation.
- Geographic Location: Living in regions closer to the equator or at higher altitudes increases UV exposure.
- Personal or Family History: A previous diagnosis of basal cell carcinoma or a family history of skin cancer can elevate the risk.
Treatments for Basal Cell Carcinoma
The treatment options for basal cell carcinoma depend on the size, location, and subtype of the tumor, as well as the patient’s overall health. Early detection and intervention are crucial for achieving the best outcomes. Below are some of the most common treatment approaches:
Surgical Excision
Surgical excision involves removing the tumor along with a margin of healthy tissue to ensure all cancerous cells are eliminated. This procedure is often performed under local anesthesia and is effective for small, well-defined tumors.
Mohs Surgery
Mohs surgery is a specialized technique used for treating larger or more complex basal cell carcinomas. During this procedure, thin layers of skin are removed and examined under a microscope until no cancer cells remain. Mohs surgery offers the highest cure rate and preserves as much healthy tissue as possible, making it ideal for tumors on the face or other cosmetically sensitive areas.
Cryotherapy
Cryotherapy involves freezing the cancerous cells with liquid nitrogen. This method is typically used for small, superficial tumors and may cause minimal scarring. However, it is not suitable for deeper or more aggressive forms of basal cell carcinoma.
Laser Therapy
Laser therapy uses focused beams of light to destroy cancerous cells. It is often employed for early-stage, superficial tumors and can minimize damage to surrounding tissues. However, laser therapy may require multiple sessions and is not appropriate for all cases.
Radiation Therapy
Radiation therapy uses high-energy beams to target and destroy cancer cells. It is typically reserved for patients who cannot undergo surgery due to medical reasons or for tumors located in difficult-to-reach areas. While effective, radiation therapy may require several weeks of treatment and can cause side effects such as skin irritation.
Topical Treatments
For very early or superficial basal cell carcinomas, topical medications such as imiquimod or fluorouracil may be prescribed. These creams stimulate the immune system or directly attack cancerous cells. Topical treatments are non-invasive but may take several weeks to show results.
Photodynamic Therapy
Photodynamic therapy combines a photosensitizing agent with a specific type of light to destroy cancer cells. This treatment is minimally invasive and often used for superficial tumors. However, it may cause temporary sensitivity to sunlight.
Prevention Strategies
While not all cases of basal cell carcinoma can be prevented, adopting certain habits can significantly reduce the risk:
- Avoid Excessive Sun Exposure: Limit time spent in direct sunlight, especially between 10 a.m. and 4 p.m., when UV rays are strongest.
- Wear Protective Clothing: Use wide-brimmed hats, long-sleeved shirts, and sunglasses to shield your skin from harmful UV rays.
- Apply Sunscreen Regularly: Use a broad-spectrum sunscreen with an SPF of 30 or higher, even on cloudy days.
- Avoid Tanning Beds: Artificial UV sources can increase the risk of basal cell carcinoma and other skin cancers.
- Perform Regular Skin Checks: Monitor your skin for any changes and consult a dermatologist if you notice anything unusual.
Living with Basal Cell Carcinoma
Receiving a diagnosis of basal cell carcinoma can be unsettling, but it is important to remember that this type of skin cancer is highly treatable. Many individuals successfully manage the condition with appropriate care and follow-up. Staying informed about treatment options and maintaining open communication with healthcare providers can help ease concerns and ensure the best possible outcomes.
Additionally, adopting preventive measures can reduce the risk of recurrence or the development of new tumors. By prioritizing skin health and practicing sun-safe behaviors, individuals can protect themselves from further damage and enjoy a higher quality of life.