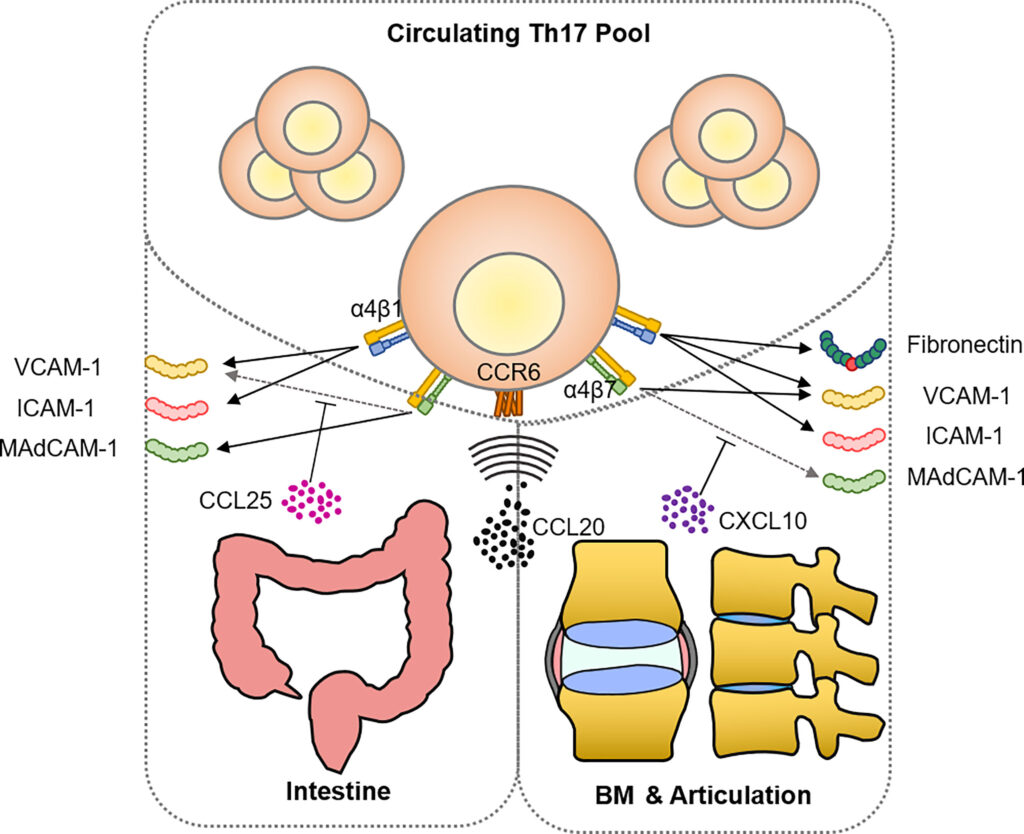
Ankylosing Spondylitis, commonly abbreviated as AS, is a chronic inflammatory disease that primarily affects the spine and sacroiliac joints. This condition can lead to severe pain, stiffness, and in advanced cases, fusion of the vertebrae. While it predominantly targets the spine, it can also impact other parts of the body, including the eyes, heart, and lungs. Understanding this condition requires a comprehensive look at its causes, symptoms, diagnostic methods, and available treatments.
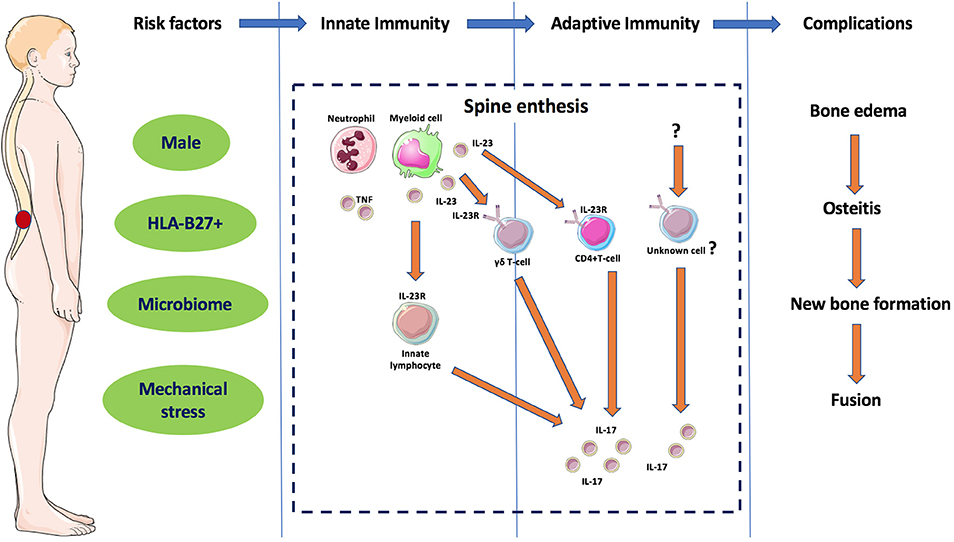
What Causes Ankylosing Spondylitis?
The exact cause of Ankylosing Spondylitis remains unknown, but researchers have identified several factors that contribute to its development. These include genetic predisposition, immune system dysfunction, and environmental triggers.
Genetic Factors
One of the most significant risk factors for developing Ankylosing Spondylitis is genetics. A specific gene known as HLA-B27 has been strongly associated with the condition. Individuals who carry this gene are at a higher risk of developing the disease, although not everyone with the gene will experience symptoms. Studies suggest that approximately 90 percent of patients diagnosed with Ankylosing Spondylitis test positive for HLA-B27, highlighting its importance in disease susceptibility.
Immune System Dysfunction
Ankylosing Spondylitis is classified as an autoimmune disorder, meaning that the immune system mistakenly attacks healthy tissues in the body. In this case, the immune system targets the joints and ligaments of the spine, leading to inflammation. Chronic inflammation can cause damage to the affected areas, resulting in pain and stiffness. Researchers are still working to understand why the immune system behaves this way in some individuals but not others.
Environmental Triggers
While genetics play a major role, environmental factors may also contribute to the onset of Ankylosing Spondylitis. These triggers could include infections, physical trauma, or exposure to certain toxins. For example, some studies suggest that gastrointestinal infections might activate the immune response that leads to the disease. However, more research is needed to confirm these connections and identify specific environmental factors.
Symptoms of Ankylosing Spondylitis
The symptoms of Ankylosing Spondylitis vary from person to person and can range from mild to severe. Early recognition of these symptoms is crucial for timely diagnosis and treatment. Below are the most common signs associated with the condition:
Chronic Back Pain and Stiffness
- Morning Stiffness: One hallmark symptom is stiffness in the lower back and hips, particularly in the morning or after periods of inactivity. This stiffness typically improves with movement and exercise.
- Persistent Pain: The pain caused by Ankylosing Spondylitis often starts in the lower back and gradually progresses upward, affecting the entire spine over time. Unlike mechanical back pain, which improves with rest, this type of pain tends to worsen when resting and improves with activity.
Fatigue and General Discomfort
Many individuals with this condition report feeling constantly tired or fatigued. This fatigue is often linked to the body’s ongoing inflammatory response. Additionally, general discomfort and a sense of malaise are common complaints among patients.
Inflammation Beyond the Spine
Ankylosing Spondylitis does not always remain confined to the spine. It can also affect other parts of the body, leading to:
- Eye Inflammation: Uveitis, or inflammation of the eye, occurs in up to 40 percent of patients. Symptoms include redness, pain, sensitivity to light, and blurred vision.
- Joint Pain: Other joints, such as the shoulders, knees, and ankles, may become inflamed and painful.
- Cardiovascular Issues: In rare cases, the condition can affect the heart, leading to complications like aortitis (inflammation of the aorta).
How Is Ankylosing Spondylitis Diagnosed?
Diagnosing Ankylosing Spondylitis can be challenging because its early symptoms often mimic those of other conditions, such as mechanical back pain or arthritis. A combination of medical history, physical examination, imaging tests, and laboratory analyses is typically used to confirm the diagnosis.
Medical History and Physical Examination
A healthcare provider will begin by taking a detailed medical history, asking about the nature, duration, and pattern of symptoms. They will also inquire about any family history of similar conditions, as genetics play a key role. During the physical exam, they will assess flexibility, posture, and range of motion in the spine and other joints.
Imaging Tests
X-rays are commonly used to detect changes in the spine and sacroiliac joints, such as erosion or fusion of the vertebrae. However, in the early stages of the disease, X-rays may appear normal. Magnetic resonance imaging (MRI) is often more effective at identifying early signs of inflammation and damage, making it a valuable tool for early diagnosis.
Laboratory Tests
Blood tests can help support the diagnosis of Ankylosing Spondylitis. While no single test can definitively confirm the condition, certain markers can provide useful information:
- HLA-B27 Test: As mentioned earlier, the presence of the HLA-B27 gene increases the likelihood of having the disease, though it is not definitive proof.
- Inflammatory Markers: Elevated levels of C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR) indicate systemic inflammation, which is consistent with the condition.
Treatment Options for Ankylosing Spondylitis
While there is currently no cure for Ankylosing Spondylitis, various treatments can help manage symptoms, slow disease progression, and improve quality of life. Treatment plans are highly individualized and often involve a combination of medications, physical therapy, lifestyle modifications, and, in some cases, surgery.
Medications
Several types of medications are used to treat Ankylosing Spondylitis, each targeting different aspects of the disease:
- Nonsteroidal Anti-Inflammatory Drugs (NSAIDs): These are usually the first line of treatment and help reduce pain and inflammation. Common examples include ibuprofen and naproxen.
- Disease-Modifying Antirheumatic Drugs (DMARDs): Medications like sulfasalazine may be prescribed if peripheral joints are involved, as they can slow disease progression.
- Biologic Therapies: Biologics, such as tumor necrosis factor (TNF) inhibitors, target specific components of the immune system responsible for inflammation. Examples include adalimumab and etanercept.
Physical Therapy and Exercise
Regular physical activity is essential for managing Ankylosing Spondylitis. Physical therapy programs focus on improving posture, flexibility, and strength. Specific exercises, such as stretching routines and swimming, are particularly beneficial because they promote spinal mobility without putting excessive strain on the joints.
Lifestyle Modifications
Making certain lifestyle changes can significantly enhance the effectiveness of treatment:
- Healthy Diet: Eating a balanced diet rich in anti-inflammatory foods, such as fruits, vegetables, and omega-3 fatty acids, can help reduce overall inflammation.
- Smoking Cessation: Smoking can exacerbate symptoms and accelerate disease progression, so quitting is highly recommended.
- Proper Sleep Posture: Maintaining good posture during sleep, such as sleeping on your back with a thin pillow, can prevent further spinal deformities.
Surgical Interventions
In severe cases where joint damage is extensive, surgical procedures may be necessary. Joint replacement surgery, such as hip replacement, can restore function and alleviate pain. In rare instances, corrective spinal surgery may be performed to address severe curvature of the spine.
Living with Ankylosing Spondylitis
Managing Ankylosing Spondylitis requires a proactive approach and a commitment to long-term care. By staying informed, adhering to treatment plans, and maintaining open communication with healthcare providers, individuals with this condition can lead fulfilling lives despite its challenges.